
Title: The essentials of bandaging
including the management of fractures and dislocations, with directions for using other surgical apparatus
Author: Berkeley Hill
Release date: March 21, 2023 [eBook #70330]
Language: English
Original publication: United Kingdom: James Walton, 1869
Other information and formats: www.gutenberg.org/ebooks/70330
Credits: Bob Taylor, deaurider and the Online Distributed Proofreading Team at https://www.pgdp.net (This file was produced from images generously made available by The Internet Archive)

ILLUSTRATED BY 122 ENGRAVINGS ON WOOD.
BY
BERKELEY HILL, M.B. Lond., F.R.C.S.,
Instructor in Bandaging, &c., in University College, Assistant Surgeon to University College Hospital, and Surgeon to Out-patients at the Lock Hospital.
SECOND EDITION, REVISED AND ENLARGED.
LONDON:
JAMES WALTON,
BOOKSELLER AND PUBLISHER TO UNIVERSITY COLLEGE,
137, GOWER STREET.
1869.
LONDON:
BRADBURY, EVANS, AND CO., PRINTERS, WHITEFRIARS.
[Pg iii]
In laying a Second Edition before the public, I have decided not to alter the scope of this little work, but simply to endeavour to increase its usefulness, by remedying omissions, and by adding new instructions where such appeared desirable. I have ventured to insert, as an Appendix, lists of the preparations requisite for the sick room and for the operating room before the ordinary operations of surgery are performed; also, lists of the instruments and appliances requisite, or possibly useful, in performing forty-nine different operations on the human body. It is hoped that, by giving the surgeon a list, such as most operators[Pg iv] draw up in manuscript for their private use, whereby they may check their preparations before proceeding to operate, some trouble may be saved.
14, Weymouth Street, W.
November, 1869.
[Pg v]
The descriptions and directions for using surgical apparatus in the following pages, are those originally prepared for oral delivery in a short course of practical lessons in bandaging and the application of surgical apparatus, given by me in University College Hospital. No attempt is made to include all efficient modes of treating surgical injuries: it is merely proposed to supply the student or practitioner with instructions by which he may refresh his memory when about to employ the ordinary surgical appliances.
The drawings are by Mr. R. W. Sherwin, who has taken much pains to furnish exact representations[Pg vi] of the apparatus, as it was applied by myself for his delineation. The directions for giving chloroform have had the advantage of Mr. Clover’s revision before publication.
14, Weymouth Street, W.
October, 1867.
[Pg vii]
| CHAPTER I. | |
| BANDAGING. | |
| PAGE | |
| General rules.—Different materials of bandages.—Position of the operator.—Mode of holding the bandage.—Varieties of turns; the simple spiral; the reverse; the figure of 8. | 1-3 |
| Bandaging the head.—The common roller.—The knotted bandage.—The Capelline bandage.—The shawl cap.—The four-tail bandage.—Fastening ice bladders to the head.—Compressing the jugular vein | 3-8 |
| Bandaging the trunk.—The breast.—The groin.—After operation for hernia.—For tapping the belly.—The T-bandage.—The strait jacket.—Manacles for delirious patients.—To suspend the testicles | 8-13 |
| Bandaging the upper extremity.—The fingers.—The thumb.—The hand.—The fore-arm.—The elbow.—The shoulder.—The axilla.—Wound of the palmar arch.—Bleeding at the elbow | 14-20 |
| Bandaging the lower extremity.—The foot.—The leg.—The thigh.—The heel.—The toe.—The knee.—A stump.—Extending a stump.—The many-tailed bandage.—Elastic socks | 21-24 |
| CHAPTER II.[Pg viii] | |
| STRAPPING. | |
| General rules.—Strapping the breast.—The testes.—Joints.—Ulcerated legs.—Scott’s mercurial dressing | 25-29 |
| CHAPTER III. | |
| TREATMENT OF FRACTURES. | |
| The head and trunk.—Of the lower jaw; by the external splint and bandage; by interdental splints, Morell Lavallée’s plan; fitting a cap to the teeth.—Of the ribs; by plaster; by a body roller.—Of the pelvis | 30-37 |
| The upper extremity.—Of metacarpal bones; by a gutta-percha glove; by a ball of tow.—Of phalanges.—Of the lower end of the radius; by the pistol splint; by the gutta-percha gauntlet.—Of both bones of the forearm.—Of the olecranon; by figures of 8 and an inside splint; by Hamilton’s plan.—Of the humerus near the elbow; by lateral hollowed splints; by a gutta-percha L-shaped splint.—Of the shaft of the humerus.—Of the anatomical or surgical neck, and of the great tuberosity of the humerus, by a cap for the shoulder.—Of the acromion.—Of the clavicle; by an axillary pad and elevation of the elbow; by a figure of 8 behind the back; the American ring pad | 37-59 |
| The lower extremity.—Rupture of the tendo Achillis.—Separation of the epiphysis of the os calcis.—Fracture of the fibula, by Dupuytren’s splint.—Of the tibia, by McIntyre’s splint; slinging the splint; elevating it on a block.—Transverse fracture of the tibia, by lateral splints; in the flexed position.—Of the patella; by back splint and figures of 8; by Malgaigne’s hooks; by strapping plaster and stick.—Of the shaft of the femur; by Liston’s method of using the long splint; by using elastic[Pg ix] extension; Coxeter’s elastic perineal band; elastic stirrup. By continuous extension with the limb bent; tendency to angular union; double incline planes; slinging the double incline planes in fracture of the neck of the femur; by continuous extension of weight and pulley | 59-80 |
| The starch bandage.—The plaster of paris bandage.—Plaster of paris splint.—Gum and chalk and other stiffening mixtures.—Sand-bags.—Cradles; Salter’s swing cradle | 81-90 |
| Leather splints; Splint for the hip | 90-94 |
| CHAPTER IV. | |
| DISLOCATIONS. | |
| General rules.—Of the lower jaw.—Of the clavicle.—Of the shoulder; signs of dislocation into the axilla; when beneath the clavicle; when behind the scapula. Modes of reduction; by the heel in the axilla; by simple extension. The clove-hitch knot.—Of the elbow, signs when both bones go backwards; distinctions between dislocation and fracture near the elbow; the mode of reduction by the knee inside the fore-arm; by extension at the wrist.—Of the radius, only, by extension at the wrist.—Of the thumb and fingers; handle for commanding the phalanx.—At the hip; signs of dislocation backwards, reduction by extension; by manipulation or leverage; signs of dislocation downwards, mode of reduction; signs of dislocation on to the pubes, mode of reduction.—Of the knee; incomplete, lateral, and posterior; mode of reduction.—Of the patella, mode of reduction.—Of the foot, mode of reduction | 94-110 |
| Scarpa’s shoes.—Varieties of talipes; equinus, varus, valgus; points to be attended to in fitting the shoe.—Casting in plaster of paris | 111-114 |
| CHAPTER V.[Pg x] |
|
| MISCELLANEOUS. | |
| The Hair suture.—The eye douche, drops for the eye.—Syringing the ears.—Epistaxis; Ice-cold injection; Plugging the nares; Belloc’s sound.—Drawing teeth; varieties of forceps; extracting incisors and canines, bicuspids, upper molars, lower molars, wisdom molars, roots; the elevator.—Stopping bleeding after extraction.—Sore nipples; nipple shields.—Plugging the vagina; Kite’s tail plug for vagina.—Injecting the urethra. Catheters, silver; different kinds of flexible catheters and bougies; conformation of the urethra.—Passing catheters and bougies; difficulties in doing so; passing the female catheter.—Washing out the bladder.—Tying in catheters.—Position for lithotomy.—Bed-sores, applications to prevent the formation of bed-sores; the floating bed; the water-cushion.—The stomach-pump, when used to empty the stomach or to inject food.—Transfusion of blood; precautions; mode of using the apparatus.—Tourniquets; the Ring; Petit’s; Signoroni’s; Carte’s; Lister’s; the make-shift.—Mercurial fumigation; general; local.—Hot air baths.—Vapour baths.—Sick carriage.—Cupping.—Junod’s boot.—Leeches.—Stopping leech bites.—Tents.—Setons.—Drainage tubes.—Issues.—Trusses, requirements of, inguinal, femoral, umbilical, Salmon and Ody’s.—Cauteries, iron; gas; galvanic. Caustics.—Vesicants, mustard, cantharides, iodine.—Corrigan’s hammer.—Poultices and fomentations.—Lister’s mode of dressing with carbolic acid.—Irrigation; Esmarch’s irrigator.—Administration of chloroform, precautions; dangers; methods; Clover’s inhaler.—Artificial respiration.—Local anæsthesia.—Ether spray, pulverised fluids.—Chloroform vapour to the uterus.—Subcutaneous injection.—Collodion.—Vaccination | 116-192 |
| List of Appliances for the Operating Room and the Sick[Pg xi] Room.—List of Sedatives and Restoratives.—For the arrest of Hæmorrhage | 195-197 |
| List of Instruments employed in Operations— | |
| On the Head and Neck. | |
| Trephining the skull.—Operations on the eye.—Hare-lip.—Resection of the jaw.—Excision of the tongue.—Cleft palate.—Excision of tonsils.—Laryngotomy.—Tracheotomy | 198-202 |
| On the Trunk. | |
| Removal of breast or tumours.—Nævus.—Tapping the pleura.—Tapping the belly.—Colotomy.—Ovariotomy.—Cæsarian section.—Strangulated hernia.—Radical cure of hernia.—Hæmorrhoids.—Fistula in ano.—Cleft perinæum.—Extirpation of the cervix uteri.—Amputation of the penis.—Circumcision.—Excision of testis.—Tapping a hydrocele.—Vesico-vaginal fistula.—Retention of urine.—External urethrotomy.—Lithotomy.—Lithotrity.—For removing foreign bodies from the urethra and bladder | 203-210 |
| On the Limbs. | |
| Ligature of the larger arteries.—Resections: of the head of the humerus, the elbow, the hip, the knee.—Removal of necrosed bone.—Amputations: at the shoulder-joint; arm; fore-arm and wrist; metacarpus; hip; thigh and leg; Syme and Chopart’s operation; metatarsus and toes | 211-215 |
[Pg 1]
THE
ESSENTIALS OF BANDAGING,
&c.
General Rules.—Ordinary bandages are strips of unbleached calico 6 or 8 yards long, having a breadth of ¾ inch for the fingers and toes, 2¼ inches for the head and upper limb, 3 inches for the lower limb, and 6 inches for the body. These, when tightly rolled for use, are termed rollers. Besides these rollers for general use there are special bandages, such as rollers of muslin for using with plaster of paris, of stocking-webbing when elasticity is needed; four- and many-tailed bandages for particular fractures, &c. Messrs. J. & J. Cash, the cambric frilling makers of Coventry, now make a very firm light bandage of unbleached cambric woven in the necessary widths and lengths for use; these are very cool and pleasant, and a decided improvement on the ordinary calico strips generally used.
Position of the Operator.—He should place himself[Pg 2] opposite his patient, not at the side of the limb to be bandaged; the limb too should be bent to the position it will occupy when the bandage is completed.
Before applying any kind of apparatus, the surgeon should see that the limb is carefully washed and dried.
How to hold a Roller.—When applying a roller it is best to begin by placing the outer surface of the roller next the skin (see fig. 1, page 3), for it then unwinds more readily, and the first turns are more easily secured; moreover the bandage should be carried from the inner side of the limb by the front to the outer side, for the muscles are thus more firmly and pleasantly confined than by turns passing in the opposite direction; of course this observation supposes the hand and forearm to be in their usual position of semi-pronation.
Varieties of Turns.—In carrying a bandage up a limb, it is necessary, in order to support the parts evenly, to employ a combination of three different turns. The simple spiral, reverse, and the figure of 8.
The simple spiral turn is used only where the circumference of the part increases slightly, as the wrist; but when the limb enlarges too fast to allow the fresh turn to overlap the previous one regularly, the turn must be interrupted, and the bandage brought back again by reverse, or by figure of 8.

Fig. 1.—Figure of 8 turn.
To reverse the bandage, the thumb of the unoccupied hand is placed on the lower border of the bandage while the roller is turned over in the other, and then passed downwards to overlap and fix the previous turn evenly. At the moment of reversing,[Pg 3] the bandage should be held quite slack, and not unrolled more than is necessary to make the reverse. All the reverses must be carried one above the other along the outer side of the limb, and only employed where really necessary.
Figures of 8 are made, as their name implies, by passing the roller alternately upwards and downwards as it enwraps the limb (see fig. 1). They are adopted where the enlargement is too great and irregular for reverses to sit evenly, over the ankle and elbow joint for instance.
Bandages for the Head.—A roller is commonly applied in three different ways to the head. 1st. For keeping simple dressings in place.
Apparatus.—1. A roller 2 inches wide, and of the usual length.
2. Some pins.
A turn is first carried round the head, over the brows and below the occipital protuberance, and fastened by a pin; this being done, the roller is carried across the dressing, and getting into the line of the first turn, is passed round the head again, then across the dressing,[Pg 4] and round the head by horizontal and oblique turns alternately, the former to fix the latter, and prevent their slipping off the dressing (see fig. 2). In the figure the oblique turns have been doubled, and would fix dressings on each side of the head.
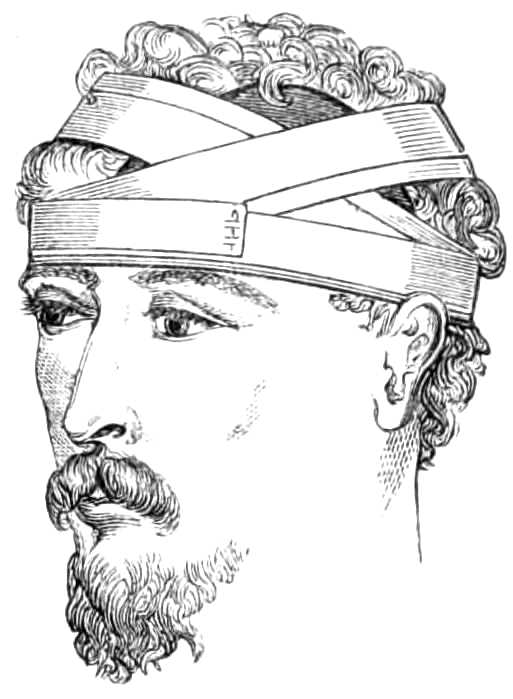
Fig. 2.—Bandage for retaining dressings in position, showing two sets of oblique turns.
Knotted Bandage.—This is used when pressure on the superficial temporal artery is required.
Apparatus.—1. A roller 8 yards long, 2 inches wide, one-third being rolled into one head, the rest into another head.
2. Some lint.
3. A piece of a wine cork one-third of an inch thick.
4. Needle, thread, and pins.
The cork is folded in a double thickness of lint; over this are placed six or eight more folds of lint of gradually increasing size, and the whole are kept in shape by a stitch passed through them and through the cork. This forms a graduated compress, and is then laid on the wound small end downwards.
One head of the roller is taken in each hand, its middle laid over the compress on the injured temple, say the right; the ends are carried round the head, one just above the eyebrows to the left temple, and the other backwards below the occipital protuberance, to the same point; the ends are then crossed and[Pg 5] changed from one hand to the other to be brought to the wounded temple. Here they are again tightly crossed, one end being carried under the chin and by the left side to the vertex, there meeting the other end, which has passed over the head, in the opposite direction (see fig. 3); at the right temple the ends are again crossed or “knotted,” but this time they are passed horizontally round the head. Having done this the ends are pinned and cut off, or if necessary the knots repeated before fastening; the first pair, if tightly drawn, usually suffice as well as several.

Fig. 3.—Knotted Bandage.
The Capelline Bandage is rarely required, but is used when the restlessness of the patient renders it difficult to keep dressings or ice-bags in place.
Apparatus.—1. A double-headed roller, 2 inches wide and 12 yards long.
2. Some pins.
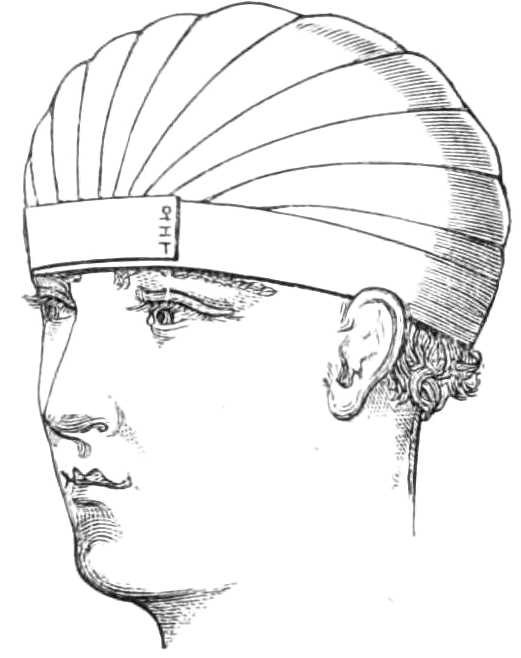
Fig. 4.—Capelline Bandage.
The middle of the roller is laid against the forehead[Pg 6] just above the brows, and the ends passed behind the occiput, where they are crossed, and while one continues the circular turns round the head, the other head of the bandage is brought over the top along the middle to the front, passing under the encircling turn, which fixes it. It is then carried back to the occiput, on one side of the first transverse band, when again fixed behind by the circular band it is brought forward on the opposite side of the first, and fixed in front. This arrangement is repeated until the head is covered in a closely fitting cap (see fig. 4).
In beginning this bandage, it is necessary to keep the first circle low down, close to the brows in front, and below the occipital protuberance behind, or the cap will not fit firmly over the skull.
A Shawl Cap is readily improvised with a silk or cambric handkerchief folded diagonally into a triangle; the base of the triangle is then carried over the brow, the apex let fall behind the occiput, where the ends cross, and catching in the apex, come round to the front to be tied on the forehead.

Fig. 5.—Shawl Cap.
The Four-tail Bandage.—Instead of applying the handkerchief in the manner just described, it may be split from each end to within six inches of the middle, and so converted into a broad four-tail bandage; the[Pg 7] middle is laid on the top of the head, the hinder ends tied under the chin, and the forward ones behind the nape of the neck (see fig. 6). Or a piece of calico, 1½ yards long and 4 or 6 inches wide, is split from each end 3 inches short of the centre—one pair of tails being rather wider than the other. If used on the face, the middle is put against the point of the chin, the two narrow tails are carried backwards to the nape, crossed, and pinned together on the forehead above the brows. The two broader tails are carried upwards in front of the ears, where they turn round the two narrow tails, to be either tied or pinned at the vertex. Four-tail bandages are used elsewhere, as in the axilla, to keep poultices in place, &c.
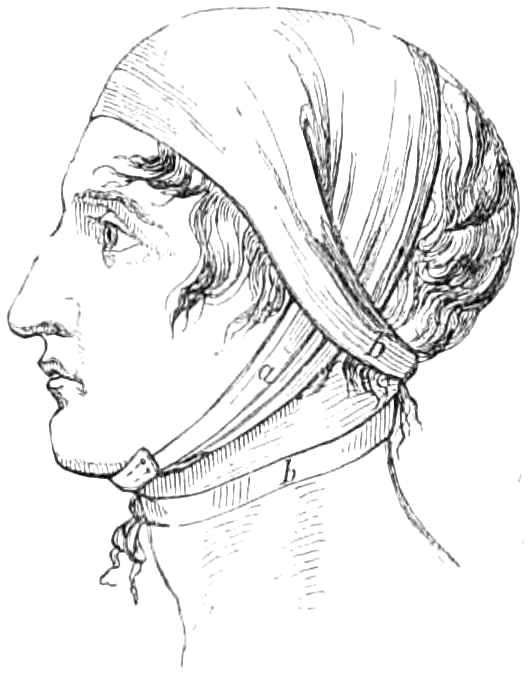
Fig. 6.—Four-tail Bandage.
To retain Ice Bladders on the Head.—This is done by folding a thin napkin over the bladder, which is then laid against the head or part to be kept cool, and the ends of the napkin are pinned tightly down to the pillow at each side. In this way the bag cannot slip, and its weight is at the same time prevented from pressing on the head.
To compress the Jugular Vein after bleeding.—After venæsection of the external jugular vein it is requisite to keep a compress of lint on the wound. This is done by fastening the bandage on the neck with[Pg 8] two simple turns, then carrying it in a figure of 8 round the neck, over the compress and under the axilla of the opposite side, then round the neck again; if the figure of 8 is passed pretty firmly, sufficient pressure is made in this way without interfering with the circulation through the vessels, and the turns round the neck of course must not be tight.
To bandage the Breast.
Apparatus.—1. A roller 3 inches wide and 8 yards long.
The roller is first carried once round the body below the breast, beginning in front and passing towards the sound side. When the bandage is fixed, the roller ascends over the lower part of the diseased breast, to the opposite shoulder, and comes back by the arm-pit to the horizontal turn; it is then passed round the chest to fix the oblique turn. Having done this, it again is carried up over the breast and shoulder, and round the body in alternate turns until the breast is fully compressed, each turn over the breast being carried higher than the preceding one, and each turn round the body overlapping the oblique turn to keep it in place (see fig. 7).
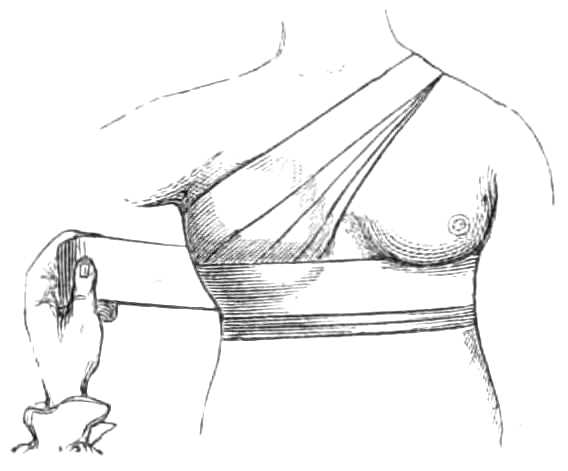
Fig. 7.—Bandage for a Breast.
To bandage both Breasts.—This is readily done by first bandaging one breast and then, carrying the[Pg 9] roller over the shoulder of the side already bandaged, bringing it across the sternum and under the second breast on to the horizontal turns, which it follows alternately with the oblique ones, as was done in bandaging the first breast. The only difference is, that in compressing the first breast the bandage was passed obliquely upwards, for the second it is carried obliquely downwards over the breast.
Spica Bandage.
Apparatus.—1. A roller or 2½ or 3 inches wide.
2. Some pins.
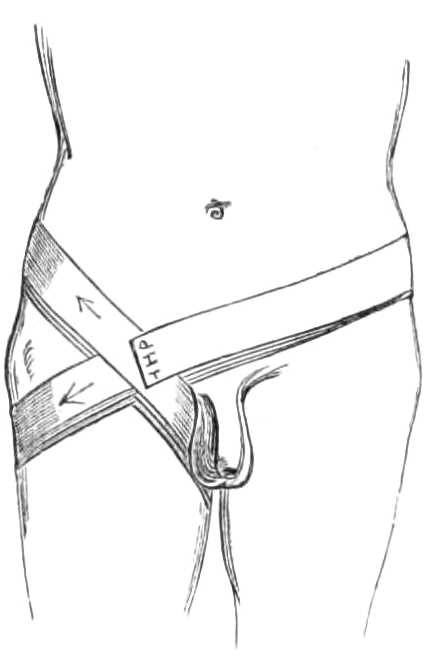
Fig. 8.—Spica for the Groin.
Lay the end on the groin to be bandaged, carry the roller between the great trochanter and the crista ilii round the pelvis to the other side, passing there also between the crista ilii and trochanter; next take the roller downwards in front of the pubes to the injured groin, then outwards round the thigh below the trochanter to the gluteal fold, and pass it up between the thighs to the groin, where the figure of 8 is completed. A second and a third are to be passed in the same way, carrying them exactly one over the other, round the body and below the buttock (see fig. 8); at the groin they should overlap, each lying a little above the preceding turn. A pin, when the necessary number of turns is completed, fastens down the end.
[Pg 10]
Hernia Spica.—The spica bandage is usually required to keep dressings and compresses in place over wounds after operation for strangulated hernia, sinuses, &c., in the groin; when the figure of 8 has been put on the first time it may be cut across in front; and, the dressings being changed, the ends may be fastened together by pins. If additional strips are laid across and fastened to the figure of 8 underneath, the required pressure is obtained, and much tedious lifting of the patient is saved (see fig. 9.)
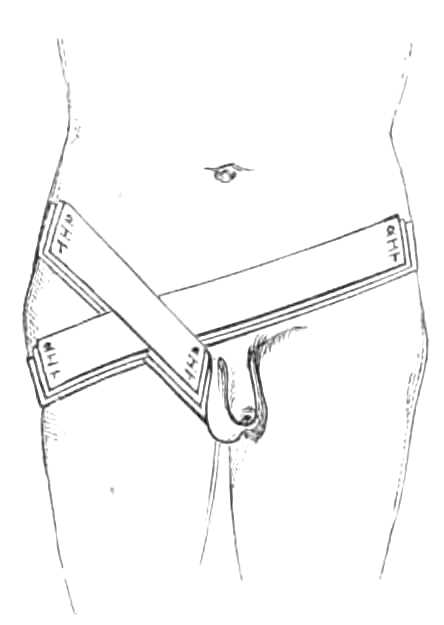
Fig. 9.—Hernia Spica.
Body bandage for tapping the Belly in Ascites.—This is made of two thicknesses of stout flannel, 2 feet wide in the middle, where it forms a continuous sheet for 18 inches, but beyond that it is split into 3 tails, 6 inches wide and 3 feet long. In the middle line, 4 inches below the centre, is a round hole 2 inches across, through which the surgeon reaches the skin to insert the trocar.
When in use, the middle of the bandage is placed in front with the hole in the mesial line of the body, and midway between the umbilicus and pubes; the ends of the right side are passed behind the back to the left, interlacing with those from the left side. When all is ready, an assistant standing on each side of the bed pulls steadily on the ends to keep up continuous pressure on the abdominal viscera as the fluid escapes.[Pg 11] After the fluid is evacuated the ends are wound firmly round the body in front, while the puncture in the wall of the belly is closed by a fold of lint attached with a strip of plaster.
The T Bandage is used to apply dressings, compresses, &c., to the anus or perinæum. A roller 3 inches wide is fastened by a couple of turns round the pelvis, and then fixed by a pin at the middle line in front. From this point the roller is carried tightly over the dressings to the corresponding point behind, and returned once or twice more until sufficient pressure is gained, when it is fastened off.
The Strait Jacket is made of jean or stout canvas. It is cut long enough to reach below the waist, around which a strong tape is carried to be drawn tight and tied after the jacket is put on. The sleeves are several inches longer than the arms, and their ends can be drawn close by a tape which runs in the gathers; a similar tape confines the garment round the neck, and it is tied behind by tapes down the sides. When the jacket is to be put on a patient it is first turned inside out, then one of the nurses or assistants thrusts his own arms through the sleeves, and facing the patient, invites him to shake hands; having thus obtained possession of the patient’s hands he holds them fast while a second assistant, standing behind the patient, pulls the jacket off the first assistant on to the patient, whose hands are thus drawn through the sleeves before he perceives the object of the manœuvre; the jacket is next tied round the neck and behind, the tapes of the sleeves are carried round the body, drawn tight till the arms are folded across the chest, and[Pg 12] fastened to the bed on each side, or tied round the body.
Manacles for Delirious Patients.—Instead of the strait jacket a double leathern muff is now generally used to restrain unruly patients. It irritates them less, and is far more easily applied.
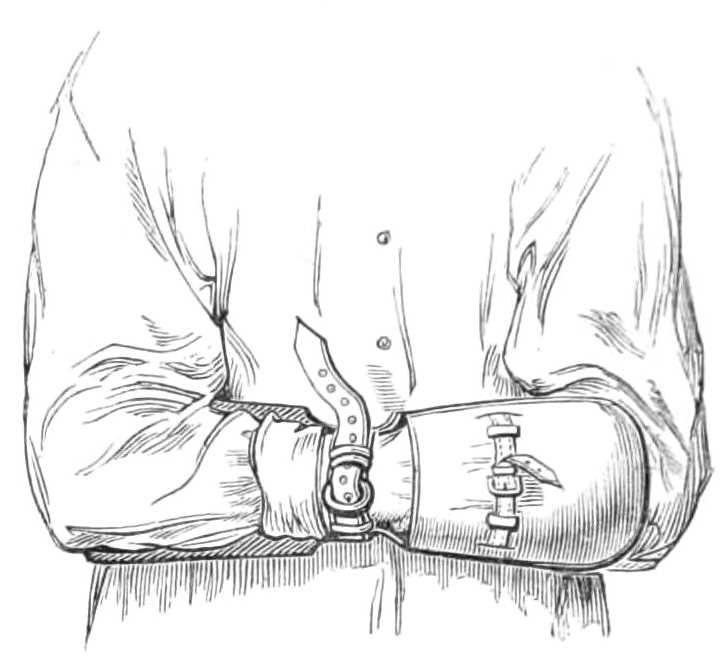
Fig. 10.—Manacles for confining the arms of delirious patients.
In wearing it the arms are crossed in front, and a strap drawn tight round both wrists. Each hand is thrust into a stout leathern glove, or muff, connected with the wrist-strap, and capable of being tightened over the fingers by a strap and buckle across the glove.
To suspend the Testicles.—Suspensories are made specially for this purpose. The best are fastened round the neck by a loop of elastic tape, but a very efficient one can be improvised with a pocket handkerchief and a piece of bandage. The bandage is tied tightly round the hips for a girdle, the handkerchief is[Pg 13] folded three-corner wise, and its longest side slipped behind the testes, the ends being passed over the girdle (see fig. 11), and tied again behind the scrotum. The loose apex of the handkerchief is drawn up in front over the girdle and pinned to it, which is all that is required (see fig. 12).
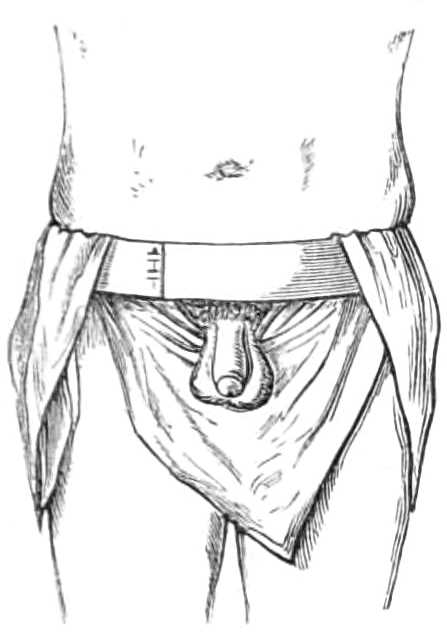
Fig. 11.—Shawl Suspensory for the Testes, in the first stage of application.

Fig. 12.—Suspensory for Testes completed.
When the patient is recumbent, the testes may be supported by a strip of diachylon plaster 2 feet long and 4 inches wide, passed across from hip to hip underneath the scrotum and testes, which lie supported on a shelf.
Another way of raising the testes is to place a soft pincushion between the thighs, and allow the swollen gland to rest on the cushion.
[Pg 14]
Bandage for the Fingers and Thumb.
Apparatus.—A ¾-inch wide roller.
The fingers are bandaged to prevent œdema when splints are tightly attached to the fore or upper arm. A roller ¾ inch wide is passed once round the wrist and then carried over the back of the hand to the little finger; then wound in spirals round it to the tip and returned up the finger, completed by a figure of 8 round the wrist and the root of the finger, and returned to the wrist before being brought across the back of the hand to the next finger, to which it is applied in the same manner till the four fingers are covered. It is a good precaution to place a shred of cotton wool between each finger before carrying the figure of 8 turn round the root; it prevents the bandages from chafing the tender skin.
The thumb is bandaged rather differently: the roller is commenced in the same way round the wrist, but the first turn is carried at once beyond the last joint, turned once or twice round the last phalanx, and continued by reverses to the metacarpo-phalangeal joint; the ball of the thumb is then covered by figures of 8 round the thumb and wrist. This is called the spica for the thumb.
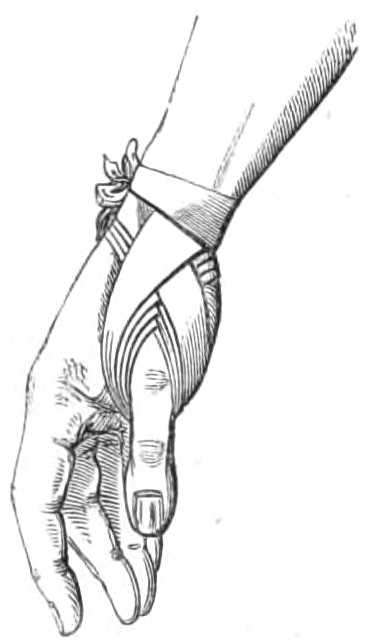
Fig. 13.—Spica for the Thumb.
[Pg 15]
This plan is sometimes employed to compress bleeding wounds of the ball of the thumb, and is applied without previously covering the phalanges, as in fig. 13.
The Hand and Arm.
Apparatus.—1. A roller 2¼ inches wide for an adult, but narrower for a child.
2. Some cotton wool.
A little cotton wool should fill the palm before applying the roller. The bandage commences with figures of 8 carried round the hand and wrist. The roller is first passed across the back of the hand from the radial border of the thumb to the root of the little finger (see fig. 14), and then across the palm, reaching the back of the hand between the thumb and forefinger.

Fig. 14.—Commencing to bandage the hand.
When the hand is covered by these figures of 8 the bandage is passed up the forearm by reverses placed over the extensor muscles till the elbow is nearly reached. Before going further a dossil of cotton wool is placed in the bend of the elbow, and on the inner condyle; the joint is bent to the degree that will be required by the splint, and the patient told to grasp some part of his dress, or the sleeve of the other arm, that he may not unconsciously extend the joint again while the bandage is being rolled round it.
[Pg 16]
The elbow is covered by first carrying the roller round the joint, so that the point of the olecranon rests on the centre of the turn (see dotted lines, fig. 15). The bandage is then continued in figures of 8, passing above and below the first turn until the elbow is covered in and the bandage of the forearm is completed.
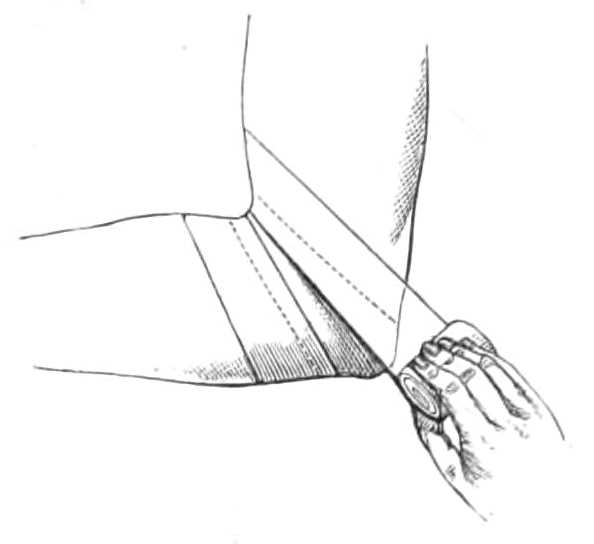
Fig. 15.—Bandage covering the elbow. The first turn over the point of the elbow is shown by the dotted lines.
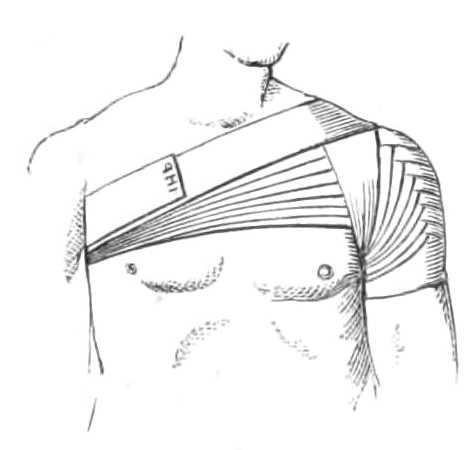
Fig. 16.—Spica Bandage for the shoulder.
The arm is covered by spirals and reverses till the armpit is reached. Before bandaging the shoulder the armpit is protected by cotton wool or a double fold of soft blanket; the roller is then carried in front of and over the shoulder, across the back to the opposite axilla, where also some wool should be placed, then across the chest to the top of the shoulder again, and under the armpit to the front (see fig. 16). These figures of 8 are repeated as often as necessary to complete the covering. The bandage is applied in this method for dressings; but when pressure is needed the first turn may be carried at once to the root of the neck, and each succeeding turn made to overlap below the last, until the point of the shoulder is gained, as[Pg 17] in fig. 37, p. 55. These are called the spica for the shoulder.
Wound of the Palmar arch.—Bleeding from this wound can usually be stopped by pressure on the bleeding point, when this fails an attempt should be made to tie the vessel at the wound, and if this be impracticable the arteries of the forearm must be deligated.
For compression the following is necessary:—
Apparatus.—1. Petit’s tourniquet.
2. Straight wooden splint.
3. Rollers 2 inches wide, and ¾ inch wide for fingers.
4. Pad and cotton wool.
5. Lint.
6. A slip of a wine cork.
7. Scissors and needle and thread.
8. Lunar caustic.
Step 1. First apply the tourniquet to the brachial artery, to control the hæmorrhage while the apparatus is being adjusted.
Step 2. Make a graduated compress by folding a sixpence or slip of a cork in two or three thicknesses of lint, trim the lint into circular disks and prepare a dozen similar disks of increasing size; lay these one on each other to form a round cone about one inch high with the piece of cork at the apex, and fasten them together by a thread.
Step 3. Clean and dry the wound, then rub its surface carefully with nitrate of silver, to lessen the suppuration.
Step 4. Bandage the fingers and thumb, and prepare the splint, which should be straight, as broad as[Pg 18] the forearm, and long enough to reach from the elbow to the tips of the fingers; it should be lightly padded.
Step 5. Envelope the wrist with a little wool; next lay the graduated compress on the wound, the small end downwards, and press it firmly in with the left thumb, while the splint is applied to the back of the hand and forearm. These are then fixed by a roller carried in figures of 8 round the hand and wrist across the compress until that is tightly pressed into the wound and the splint fixed to the limb. The roller is then carried along the forearm, a fold of wool laid in front of the elbow, the tourniquet removed and the roller carried to the axilla while the forearm is raised, flexed across the chest, and fastened to the side.
This apparatus is worn without being disturbed for three or four days if bleeding do not return; but at the end of this time it should be examined; if painful or if discharge ooze out at the wound, the bandage should be removed and readjusted less firmly than before, a piece of wet lint replacing the graduated compress.
Venæsection.—Bandage and bleeding at the bend of the elbow.
Apparatus.—1. Lancet.
2. Tape.
3. Pledget of lint.
4. Dish.
5. Staff.
In opening a vein at the bend of the elbow, the median basilic is selected, simply because it is usually the largest, but any branch that is superficial, and well filled with blood, may be opened.
[Pg 19]
The patient should sit or stand, in which positions, syncope, one of the objects of bleeding, is attained by the abstraction of a less amount of blood than in the horizontal posture.
The surgeon places a graduated bleeding dish on a chair or stool within his reach, and a pledget of lint in his waistcoat pocket; he next gives the patient a heavy book, or staff to grasp in his hand. The arm being bare to the shoulder, a tape, ¾ inch broad and 1¼ yard long, is tied round the arm tight enough to impede the venous, but not the arterial flow.
The surgeon standing opposite his patient and grasping the arm to be bled with his left hand, so that his thumb controls and steadies the swollen vein, takes his lancet between the right forefinger and thumb; then going through skin and vein at one stroke, carries the lancet upwards for about ¼ inch along the vein. The puncture of the lancet should be quite vertical, and the extraction also made quite vertically, that the slit in the vein may correspond to the slit in the skin.

Fig. 17.—Adjusting the tape after bleeding.
This being done, the operator lays aside his lancet, and takes up the dish, holding it so that the blood shall flow into it: when the dish is placed, he lifts his left thumb from the vein cautiously or the sudden spirt of blood will fall outside the dish and be lost. When the desired amount is drawn, the operator compresses the vein again with the left thumb, and setting down the dish, puts the pledget of lint over the wound. He keeps the pledget in place with his left thumb, while he releases the tape round the arm and places its middle obliquely across the pledget. His left thumb[Pg 20] presses the pledget on the wound, while the right hand takes the end of the tape which is farthest from his left, and passes it under the forearm below the elbow to his left fingers, which grasp it tightly. He then takes the other end with his right hand (see fig. 17), and bringing it round the arm above the elbow, carries it across the pledget: as he does this, he replaces his left thumb on the compress with his right forefinger, which he keeps there while he brings up the end of the tape he has already in his left fingers, and throws it over the arm above his right forefinger, then passing his left hand below the right forefinger, he catches the same end of the tape again and draws it back. The two ends thus locked in a loop over the compress, are secured by tying them in a bow outside the elbow and the operation is finished (see fig. 18).

Fig. 18.—The bandage completed.
[Pg 21]
For adults the most useful width for the rollers is 3 inches, and the length the ordinary one of 8 yards.
The Foot is usually bandaged without covering the heel, and the bandage is begun as follows:—
The roller being held in the right hand for the right foot, or in the left hand for the left foot; the unoccupied hand takes the end, and passing it under the sole, brings it up on the back of the foot just behind the toes, where it is made fast by carrying the roller outwards over the back. When one turn is completed, the bandaging is continued by reverses until the metatarsus is covered, then one or two figures of 8 round the foot and ankle carry the bandage to the leg, where it proceeds upwards by spiral turns round the small of the leg, and by reverses up the calf. The reverses lie at equal distance up the leg, on the muscles, not over the bone, that the skin be not pinched between the crease of the bandage and the bone. When the calf is passed, the roller is continued by figures of 8 above and below the knee, until that joint is covered in, then by reverses up the thigh to the groin, where the bandage terminates by a spica round the body (see page 9). This is the ordinary bandage for the lower limb. There are some varieties for particular parts, these are:—
To cover the Heel.—Holding the roller as for the foot, pass the end behind the heel, bring it out by the outside over the front of the ankle-joint, and complete the turn with the roller. In doing this, the point of the heel must catch the middle of the bandage. If the foot is a long one, the roller should be three[Pg 22] inches broad; but a narrower bandage is more easily fitted on a small foot. After the first turn, the bandaging is continued by carrying the roller in figures of 8 round the foot and ankle, passing alternately above and below the first turn until the ankle is covered as in fig. 19.
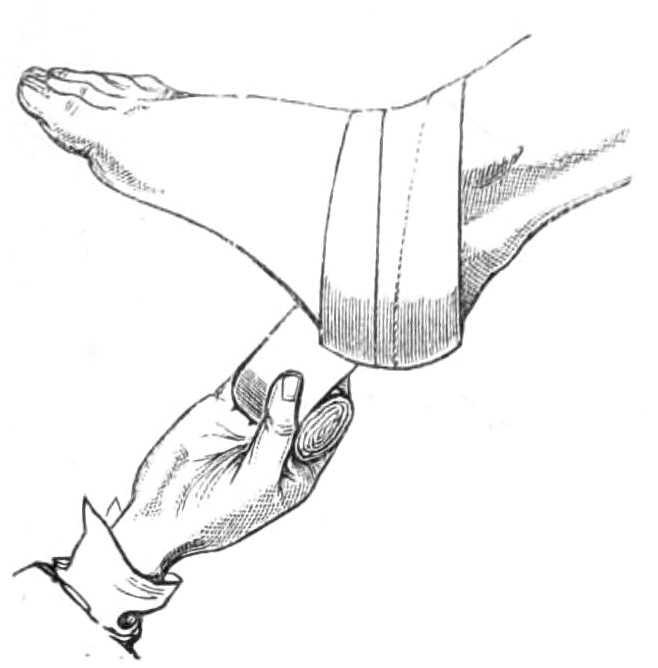
Fig. 19.—Covering the Heel.
To bandage a Toe.—Take two turns round the foot, with a bandage one inch wide, then go round the toe to be raised, and back again round the foot. This figure of 8 lifts a toe above the rest if taken from the dorsal, and depresses it if taken from the plantar surface.
The Knee is bandaged by beginning with a simple turn round the leg above the calf, then carrying the roller across the patella to the thigh above the knee: and next entwining it in a circular turn round the thigh before descending over the patella to the leg below the knee, where this is repeated until the knee is covered.
To bandage a Stump.—The flaps are first supported by two or more strips of plaster, one inch wide and ten or twelve long, carried from the under surface of the limb over the face of the stump, and a slip of wet lint and oilskin is applied to the wound. The muscles and soft parts are next confined by a bandage.[Pg 23] This is first fixed by simple turns below the nearest joint, and brought downwards in figures of 8 round the limb till the end of the stump is reached, which is next covered in by oblique and circular turns carried alternately over the face of the stump and round the limb, as is shown in fig. 2 for bandaging the head. Or, if a double-headed roller be used, in the manner directed for the capelline bandage on page 5.
Extending a Stump.—When the soft parts fall away from the bone they may be drawn down by attaching a weight by cord and pulley, as described for extending the hip-joint (see fig. 80). The stump should be lightly bandaged and the cord fastened to its upper and under surface. The weight is very small at first, and should be increased from time to time as required.
Many-tail, or 18-tail Bandage, or bandage of Scultetus.—A roller is cut into short lengths long enough to encircle the limb and to let the ends overlap 2 or 3 inches; these are applied separately, the lowest first, the next overlapping it, and the next overlapping the second until the requisite number are applied. Sometimes the tails are attached to each other before they are applied. To do this, the tails are laid out on a table, so that the second overlaps one-third of the width of the first strip, and the third strip overlaps the second, and so on. When all the tails are arranged, a strip is laid across their middle and fastened to each tail by a stitch; but this is not a necessary part of the bandage, and it prevents single tails from being removed. This bandage is used in compound fractures and other wounds, as the soiled[Pg 24] strips can be replaced without raising the limb to pass the roller under it.
Elastic Socks and Stockings are made to support varicose veins of the legs. They are woven of india-rubber webbing with silk or cotton. The latter are the lowest priced and often even the most comfortable to wear. The stockings should fit carefully everywhere, especially at the small of the leg, where they generally are too slack, while they cut at the upper end below the knee.
[Pg 25]
Strapping is a method of supporting weak or swollen joints and other parts. Sheets of calico, wash-leather, or white buckskin, spread with lead or soap plaster, are prepared for this purpose. A sheet should be rubbed with a dry cloth before using, to remove adherent dust, &c. It is then cut into strips varying in width between ¾ inch and 2 inches, according to the evenness of the surface to be covered: narrow strips fit best over joints and irregular surfaces. When applied to a limb, the strips should be about one-third longer than its circumference. Each strip or strap is first warmed by holding it to a fire, or by applying its unplastered side to a can of boiling water; when hot, the strip is then drawn tightly and evenly over the part. If the surface to be strapped be irregular, it is best to dip each strip of plaster in hot water before applying it, being thus quite supple the strap fits the limb more exactly. When the limb is thickly beset with hairs, it is a good plan to shave the part where the plaster will lie before putting on the straps.
Strapping the Breast.—Strapping is put on the breast in the same way as the bandage (page 8). The straps should be not more than 2 inches wide, and long[Pg 26] enough to pass forward under the axilla and breast from the lower angle of the scapula on the same side as the injured breast, across the chest as far as the spine of the other scapula. The strips are then warmed and laid on alternately over the breast and across the chest, until the former is fairly supported.
Strapping has this advantage over a bandage—its circular strips do not pass round the chest completely and thereby hamper the breathing as the roller does.
To strap the Testicle.
Apparatus.—1. Strips of soap plaster spread on calico, or better, on wash-leather, ½ inch wide and 12 inches long.
2. A can of boiling water.
3. Razor and soap.
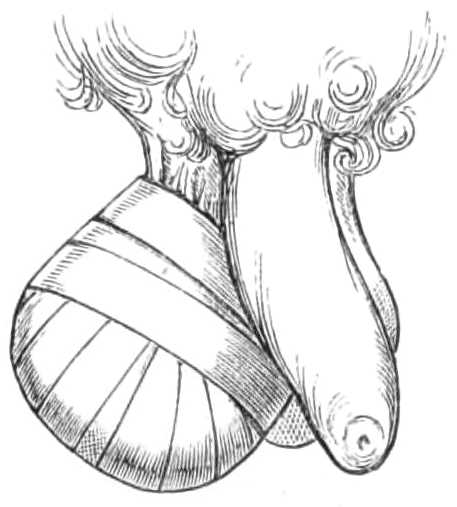
Fig. 20.—Strapping the Testis.
First, shave the scrotum; then tighten the skin over the testis with the left thumb and forefinger passed above it; take a strip of plaster 6 inches long and ½ inch wide, and encircle the cord tightly with it; next pass another strap of the same width, 9 or 10 inches long, from the back of this ring, over the testicle to the front, drawing it tight also (see fig. 20). The strapping is continued by laying fresh straps over each other until the whole testis is covered in. Lastly, take a strip 15 or 20 inches long, and, beginning at the ring above, wind[Pg 27] it round and round the testicle until all the vertical strips are confined in place by this spiral strip.
The strapping should be re-applied the second or third day, as the testicle by that time will have shrunk within its case.
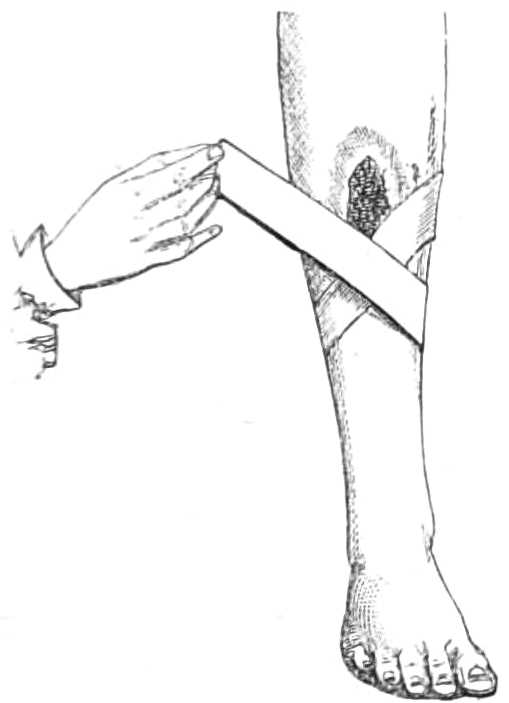
Fig. 21.—Strapping an Ulcer.

Fig. 22.—Strapping the Ankle.
Strapping Ulcers and Joints.—Cut strips of plaster one-third longer than the circumference of the part to be strapped; if that is irregular, as the ankle or wrist, they must be narrow: commonly the width varies between ¾ inch and 1½ inch. The strips are warmed, the middle passed behind the limb, the ends crossed in front (see fig. 21) and drawn tight, but with sufficient obliquity for the margins of the strip to lie evenly. The strapping is begun as low down the limb as requisite, and continued upwards by laying on more strips, each overlapping about two-thirds of the preceding strap. When the process is finished, the ends[Pg 28] should meet along the same line, and all the uppermost ones be on the same side.
The ankle is strapped differently. Strips are prepared about ¾ inch wide; one is carried behind the heel and its ends brought forward till they meet on the dorsum of the foot; a second, encircling the foot at the toes, secures the first; a third is again carried behind the heel above the first, and is fixed by a fourth round the foot. This is continued until the foot and ankle are firmly supported (see fig 22).
Strapping a Joint with Mercurial Ointment.
(Scott’s Bandage.)
Apparatus.—1. Mercurial ointment.
2. Diachylon plaster.
3. Lint.
4. Spirit of camphor.
5. Cotton wool.
6. Freshly scalded starch, or solution of gum.
7. Binder’s millboard.
Spread the ointment on a piece of lint large enough to cover the joint, and to extend four or six inches above and below it; then wash the joint with warm water and soap and dry it carefully; next sponge it well with the spirit of camphor for five minutes. Tear the lint into strips and wrap it round the joint; then strap the part firmly from below upwards over the lint with strips of diachylon plaster, each overlapping the preceding. Lastly, envelope the joint in a thin layer of cotton wool, and roll a bandage soaked in starch over all. If the patient wears no other kind of splint the bandage may be strengthened by laying a piece of millboard well softened in boiling water along each[Pg 29] side of the joint before the starch bandage is applied. As the enlargement of the joint shrinks, this application must be renewed, usually every fortnight is often enough.
[Pg 30]
Fracture of the lower Jaw.—The External Splint and Bandage.—A method requiring the lower jaw to be firmly fixed against the upper one while the broken bone knits.
Apparatus.—1. One and a half yards of bandage four inches wide.
2. A piece of gutta-percha, sole leather, or binder’s millboard.
3. Dentists’ silk or wire.
4. Boiling hot, and cold water.
Step 1. The fracture is first reduced. While the apparatus is being fitted, the recurrence of the displacement is prevented by the hands of an assistant, or by lacing the teeth together with stout silk or wire. It is well also to wet the patient’s chin with a sponge and cold water, to prevent the gutta-percha from sticking to his beard while it is soft.
Step 2. A piece of gutta-percha is prepared 2½ inches wide and long enough to reach from one angle of the jaw to the other when passing in front of the chin. This is softened thoroughly by immersion in boiling[Pg 31] water, and when quite pliable should be quickly removed from the hot and plunged for a moment into cold water: if a towel be previously laid in the hot basin, the gutta-percha can be lifted on it without stretching. It should be laid on a table, and its surface sponged with cold water to prevent it sticking to the skin, it is then slit from each end into tails 1 inch and 1½ inch wide, leaving 2 inches uncut at the centre. So prepared, the splint is applied to the jaw with the middle pressing against the chin, the narrower ends being carried horizontally backwards to the angles of the jaw; the broader part is next bent up beneath the chin, its ends overlapping the horizontal ones. While the splint is still soft, the surgeon presses it firmly upwards that the gutta-percha may mould itself accurately to the chin. When set, the splint is removed, trimmed, and punched with holes here and there for evaporation. A covering of wash-leather may be added, if desired. When the splint is finished, it is replaced on the chin. If sole leather or pasteboard be used instead of gutta-percha, they must be prepared in the same way, but allowed to remain on the chin twenty-four hours that they may set before the final trimming and adjustment.
Step 3. A bandage, 4 inches wide and 1½ yard long, and slit from each end to about 2 inches from the centre, is then applied to the splint, and a small pad of folded flannel should be placed at the nape of the neck to protect the skin from the crossed bandage. When all is ready, the two upper ends are carried behind the neck, crossed, drawn tight, and tied or pinned on the forehead; the lower ends are carried[Pg 32] upwards, taking a turn round the first pair at the temples, and fastened at the vertex (see fig. 23).

Fig. 23.—Outside splint for fracture of the lower jaw.
The ligatures that may have been used on the teeth can now be removed, or if they cause no pain, they may be left for a week or two.
It is a useful precaution to place a piece of soap plaster spread on soft leather, under the chin and along the throat, to protect the skin from the chafing of the splint while it is worn.
Sometimes the jaws close too nearly to allow food to be taken between them. It is then necessary to place a thin wedge of softened gutta-percha, 1½ inch long, ½ inch wide, and about ⅓ inch thick, between the molars on each side. The gutta-percha must not be softened much, or when the bite is taken the teeth will pass through it. These plugs should be omitted unless absolutely required, as the fragments keep a better position without them.
On emergency, when gutta-percha, leather, or pasteboard are not at hand, the jaw may be set, and then kept in position by a four-tail bandage, made from a pocket-handkerchief, until more complicated apparatus can be prepared.
The apparatus must be worn five weeks before it is laid aside and mastication permitted.
[Pg 33]
Interdental Splints.—In cases of unusual difficulty, interdental splints may be employed. To fashion some of these, the mechanical skill of a dentist is requisite, unless Morel Lavallée’s plan is resorted to. He applied a mould or socket to the line of the teeth, and kept it in place by pressure underneath the jaw. He first brought the fragments into apposition by means of threads and wire. Then he took a piece of gutta-percha, about ⅓ inch thick and ½ inch broad, and long enough to extend, when bent along the lower jaw, from one wisdom molar to the other. This was softened in water, and pressed on the teeth; next a well-padded horse-shoe plate was placed under the chin, reaching from one angle of the jaw to the other, and two wires were passed through the side of this plate opposite the angle of the mouth; these were drawn through the plate by a screw nut; their upper ends being curved into hooks with sharpened points. The points catch into the gutta-percha; by screwing up the nuts, the chinplate was raised, and the teeth driven up and bedded into the splint.
This method, however, has its disadvantages. If the fracture take place behind the first molar, the bearing on the upper fragment is too slight to keep it down in its place.
In the New York Medical Journal for September and October, 1866, Mr. Gunning, of that city, has published a mode of applying caps fitted to the teeth for fracture of the jaw-bone. External support is abandoned wherever it is possible. In simple fractures, the caps or interdental splints, being accurately fitted, require no fastening to the teeth.
[Pg 34]
The jaw should be adjusted in its splint as quickly as possible after the accident. The fragments are first brought into their true position. Gaps through loss of teeth at the line of fracture, are filled by plugs of hard wood, and the fragments kept in place by wiring the teeth together tightly. Continued strain on the teeth causes much pain; hence all means for keeping the fragments in place while the splint is being fitted should be removed when that is accomplished, though ligatures used solely to support loosened teeth may be left, as there is no traction upon them. Stumps, and teeth loose before the accident are best taken out, if they interfere with the arrangement of the splint.
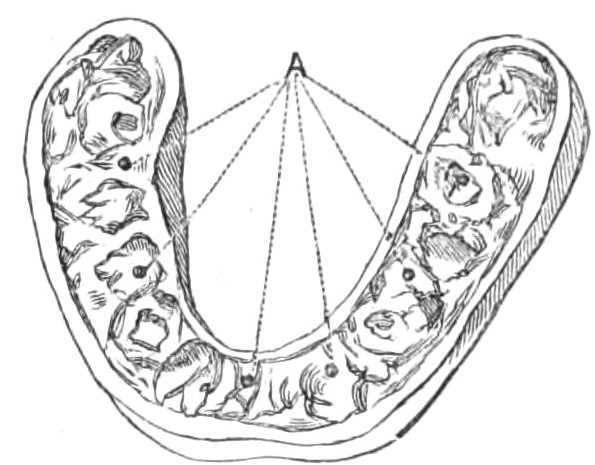
Fig. 24.—Vulcanite Interdental Splint to fit the arch of the teeth of the lower jaw, seen upside down. The holes marked a pass through to the upper surface, to allow water to be injected between the splint and the teeth, while it is worn, for cleaning.
The next thing is to take a mould of the lower jaw in wax softened by heat, holding the wax in an ordinary dentist’s tray. From this mould a plaster cast of the jaw is made. If the line of teeth be uneven in the cast, it is to be sawn through, the pieces raised to the right level, and cast again. In this cast a vulcanite plate is made exactly fitting the teeth (see fig. 24). The margins of the mould or splint should be carried down below the line of the gums, to grasp the jaw beyond the alveolar border; and when the fracture takes place behind the teeth, its outer side should be prolonged backwards as far as the muscles will allow,[Pg 35] to prevent the displacement of the anterior fragment outwards which muscular action produces in these fractures. Holes should be made in the top of the splint, to permit a stream of water to be sent between the splint and the teeth daily, for cleanliness. Also, in difficult cases, a hole should be cut opposite a tooth in each fragment, for ascertaining from time to time that each part continues in its proper position while the splint is worn.
Metal is used for the plate by English dentists, instead of vulcanite. It can be made thinner, and is less brittle than the latter.
The perfect fit thus secured suffices, in simple fracture, to keep the parts in close apposition; while the movements of eating and speaking are very little interfered with.
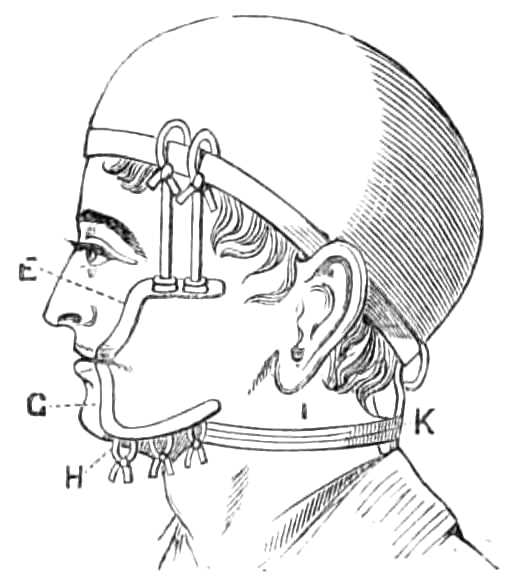
Fig. 25.—Showing the method for supporting externally the jaws in the splint, when the teeth are not fastened to it by screws, E. Upper wing; G. Lower wing; H. Mental band to keep the jaw up in the splint; I. Neck-strap to keep the band back; K. Balance-strap to hold skull-cap in place. The upper wings are of course dispensed with, when a single splint only is used.
When the displacement is considerable the fragments are held in place by riveting one or more teeth to the cap, or, when circumstances prevent support being obtained in this way, external support is supplied to the splint by steel wings, fixed into the splint at the angles of the mouth (see fig. 25), and carried outside the cheek to the angles of the jaw. A piece of stout jean or canvas, cut to fit under the chin, is then connected[Pg 36] with these wings, and also fastened by a tape behind the neck.
If the case require that a bearing be made on the upper jaw as well as the lower one, as in fracture of both jaws in edentulous persons, the two splints are articulated behind, so that they may open and shut with the lower jaw. Each piece then carries a wing, the lower one supporting a chin-piece, and the upper one being connected by strings attached at the temples to a close-fitting skull-cap. The skull-cap is prevented from slipping forward by connexion with a strap fastened to both shoulders.
A fractured Rib is very well treated by strapping the injured side alone, without enrolling the chest in a tight bandage, which harasses the patient by impeding respiration.
Apparatus.—1. Diachylon plaster.
2. Can of boiling water.
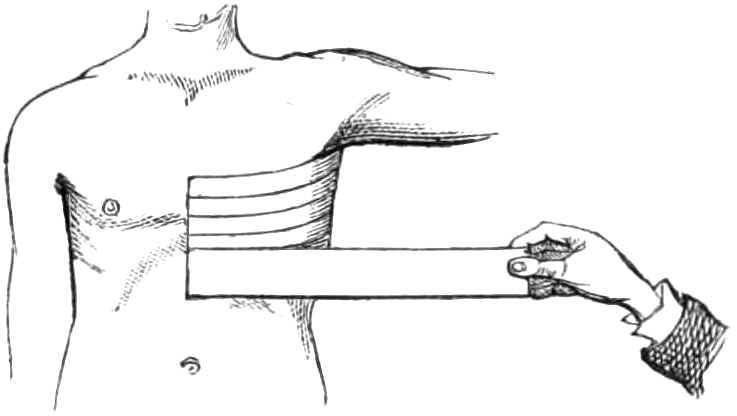
Fig. 26.—Strapping a broken Rib.
Strips of plaster long enough to reach from the spinal column to the sternum, and 2 inches wide, are to be firmly drawn round the injured side. The first strip should be carried as high as can be managed under the arm-pit. The next strip overlaps it about an inch (fig. 26), each succeeding strip overlapping and fixing the preceding one until the lower ribs are covered in. The arm[Pg 37] should then be bandaged to the side, and supported in a sling.
A second mode of treating fractured ribs, is to take a flannel roller 6 inches wide, and 8 yards long, and carry it firmly round the chest in successive spirals, beginning at the armpits, and passing down till the waist is reached. The turns of the roller may be kept from slipping down by throwing across the shoulders two strips of bandage like a pair of braces, and stitching each turn to the brace in front and behind. The arm should be confined to the side as in the other method. This plan has the inconvenience before mentioned of interfering with respiration.
In Fracture of the Pelvis, the fragments are kept in position by a broad roller carried several times round the pelvis and fastened.
Fracture of the Metacarpal Bones.
Apparatus.—1. A piece of gutta-percha.
2. A roller 2 inches wide.
In treating this fracture it is important to keep the broken bone in place without confining the wrist or fingers.
A pattern of the palm and dorsum of the hand is cut out of paper, which is doubled round the radial side, letting the thumb out through a hole of convenient size to clear it (see fig. 27). The piece of paper is then laid on a sheet of gutta-percha ¼ inch thick, and the requisite quantity cut off; a hole as big[Pg 38] as a pea is next punched in the gutta-percha in the middle, about 1 inch from the lower border, or at a point corresponding to the hole in the paper for the thumb. The fragments are then pushed into place and held so by an assistant, while the surgeon softens the gutta-percha in boiling water; when thoroughly soft, he draws the thumb through the little hole punched in the gutta-percha, and moulds the splint to the palm and back of the hand, bringing the ends of the gutta-percha together at the ulnar side of the hand; the fragments are held carefully in position till the splint is set. The splint is afterwards removed and trimmed. A few holes should be punched in it after it is moulded to allow perspiration to escape. The splint may then be covered with wash-leather, and a pair of straps with buckles stitched on to keep it in place. It is worn for three or four weeks, or until the fragments are united.

Fig. 27.—Gutta-percha Glove for fractured Metacarpal Bone.
Should gutta-percha not be at hand, another plan is effectual.
Apparatus.—1. A firm ball of tow large enough to fill the palm, stitched in old linen.
2. A roller 2 inches wide.
The broken bone is first replaced; then the hand and fingers bound on to the ball by carrying the roller around them until they are all immoveably confined.
This plan has the disadvantage of confining the whole hand for the fracture of one metacarpal bone;[Pg 39] the gutta-percha allows free use of all but the metacarpal bones.
Broken phalanges are treated by bandaging them on to a slip of wood long enough to reach into the palm; the slip must be well padded, that the somewhat concave anterior surface of the digit may accommodate itself on the flat splint. If more than one finger be injured, and the fracture be compound, the splint should then reach up the palmar aspect of the forearm and hand. Fingers should be cut in it to correspond with the fingers to be fastened to the splint.
Fracture of the lower end of the Radius.—Colles’ Fracture.—The displacement in this fracture is mainly due to the lower end of the radius and the carpus being carried backwards while the shaft projects in front.
Apparatus.—1. A straight splint of wood. A second splint, curved at its lower end.
2. Pads and cotton wool.
3. A roller 2 inches wide.
4. A sling.
5. A strip of plaster.
The objects to be attained in treating this fracture are to press the lower fragment forwards and to draw (adduct) the hand towards the ulnar side of the limb. For this purpose a straight and a curved splint are used.
No bandage should be placed under the splints in treating any fracture of the shaft of the radius or ulna, lest the broken ends be pressed into the interosseous space.
Step 1. Prepare the splints. The straight splint[Pg 40] should reach, when the arm is bent, to a right angle with the thumb upwards, from a little below the inner condyle to the lower end of the upper fragment or shaft; the curved or pistol splint extends from the outer condyle to the joint of the first and second phalanges. The width of both splints should slightly exceed that of the forearm. The bend of the lower end of the pistol splint should be abrupt, and directed towards the ulnar border opposite the wrist, where the margin of the splint should make an obtuse angle of about 1½ right angles (see fig. 28).

Fig. 28.—Pistol Splint for fracture of the Radius near the lower end.
Pads used with these and other wooden splints are made of layers of cotton wool, carded sheep’s wool, tow, or folds of old blanket. These materials should be stitched in old linen or calico, and covered outside with oiled silk where likely to be stained with the discharge from wounds.
The pads must be thicker below than above, to keep the splints parallel along the forearm; and that of the pistol splint is thickest opposite the carpus, to push the lower fragment forwards.
Fixed deformity opposite the wrist is usually present from impaction of the fragments; moderate extension may be employed to remove this, but forcible or continued efforts give great pain and do harm, by further straining the already wrenched ligaments. After these preparations the splints are applied.
Step 2. Put a very little cotton wool in the palm[Pg 41] and across the root of the thumb, before the roller is begun, lest it chafe the carpus in front. The curved splint, with the barrel or longer part inclined downwards below the forearm, is next attached to the back of the hand by a roller carried in figures of 8 round the hand and root of the thumb, but not above the wrist (see fig. 29). This is made fast by a pin.
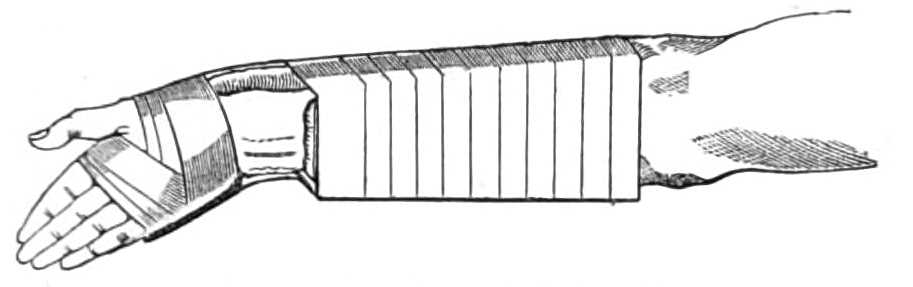
Fig. 29.—Fracture of the Radius.
Step 3. Raise the straight part of the outside splint till parallel to the forearm, thus adducting the hand to the ulnar side; and fix the splint by a strap of plaster an inch wide carried round it and the forearm below the elbow.
Step 4. Apply the inside straight splint next, keeping the front of the carpus and of the lower fragment exposed. Draw the two splints together by simple spiral turns of a roller, begun just below the elbow and carried down to the lower end of the inside splint, there fasten it off.
Step 5. Put a narrow sling under the forearm between the elbow and the wrist to support the limb comfortably.
When the apparatus is finished the position of the broken fragments should be visible (see fig. 29) and not concealed by bandage. The hand should also be quite free of the sling, lest it be drawn from its proper[Pg 42] adducted position. The fragments are in good position when the hollow on the anterior aspect of the wrist and the prominence on the corresponding posterior surface are removed.
The Gutta-percha Gauntlet is another plan of treating fracture of the lower end of the radius that may often be adopted from the first, and may always replace the wooden splints and bandage when the swelling has subsided. It was contrived by Mr. Heather Bigg, and permits the patient to use his hand to some extent while the bone is uniting.
Apparatus.—1. A piece of gutta-percha ¼ inch thick, wide enough to enwrap the metacarpus and wrist, and long enough to reach up the lower half of the forearm. Two thirds across the width, and about 1 inch from the lower end, a small round hole is punched. The sheet is then softened in hot water, and applied to the hand, the thumb being thrust through the hole punched to receive it, which rapidly enlarges when soft. The gutta-percha is then adjusted to the hand and forearm, its borders meeting at the ulnar side of the limb, rather nearer the inner border of the arm than is depicted in fig. 30.
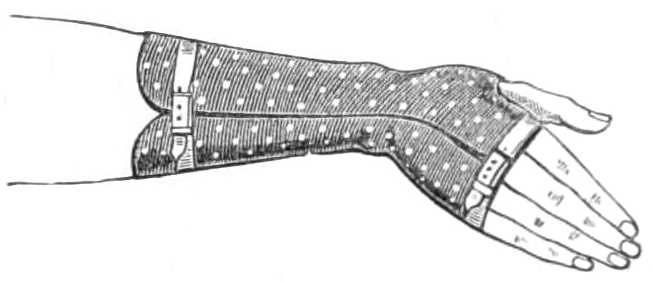
Fig. 30.—Gutta-percha Gauntlet for Colles’ Fracture.
If the fracture is recent, it must be reduced while the splint is soft by extending the hand and holding the parts in the required position until the gutta-percha is set. Before removing the splints superfluous[Pg 43] edges should be marked, and, when the splint is off, trimmed away with a knife. Holes must also be punched at frequent intervals that the perspiration may escape. The splint is next lined with wash-leather, and fitted with a pair of straps and buckles to keep it in place.
By this plan the fingers are left free, and some motion allowed also to the thumb. The only joints kept immoveable are those of the carpus and wrist.
Apparatus of some kind must be worn three weeks continuously; then for a fortnight longer, while it is removed every day to allow passive motion of the fingers and gradually of the wrist also to be practised. Care should be taken to warn the patient that pain and stiffness last long in these fractures, lest he blame the surgeon because he does not quickly recover full use of his arm.
Fracture of the Shaft of one or both Bones of the Forearm.
Apparatus.—1. Two straight wooden splints.
2. Pads and wool.
3. 2-inch wide roller.
4. Sling.
The treatment is the same whether one or both bones are broken. Caution has been already given against bandaging the forearm underneath the splints.
Step 1. Prepare two straight wooden splints; one to go in front of, and one behind the forearm. The posterior or outside reaches from the external condyle to the end of the metacarpus; the anterior or inside splint from a little below the internal condyle only as far as the wrist, keeping clear of the ball of the thumb.[Pg 44] The splints should be slightly broader than the forearm, and well padded; towards the lower end the padding should be thicker than above. The forearm is bent to a right angle and the thumb put upwards.
Step 2. Reduce the fracture by gentle slow extension at the wrist; this being effected, apply the splints to the forearm, and let an assistant hold them while the bandage is rolled on.
Step 3. When a little wool has been wrapped round the hand and wrist, fasten the dorsal splint by figures of 8 carried round those parts; then draw the two splints together by simple spirals continued to the elbow (see fig. 31).
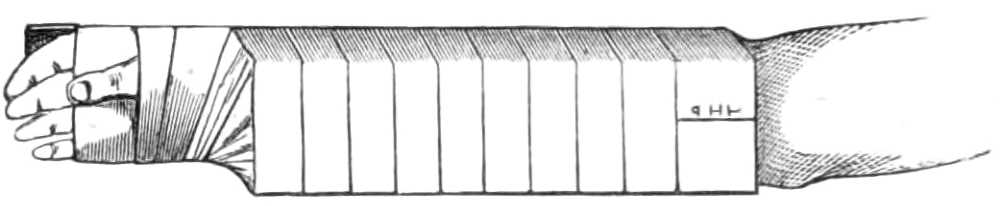
Fig. 31.—Fracture of both Bones of the Forearm.
Step 4. Support the forearm in a sling, to complete the apparatus.
The splints are worn three weeks; after this, passive motion may be practised daily, and the splints finally abandoned ten days later. But a sling is still required some ten days after the splints are laid aside.
When the ulna alone is broken, an anterior splint reaching from the inner condyle to the tips of the fingers often suffices without a second one.
When the shaft of the radius is broken high up (a rare accident) the displacement is sometimes very difficult of reduction unless the wrist be well supinated.[Pg 45] To preserve this position it may be necessary to use a wooden angular splint, and to fix the vertical part to the arm behind the elbow, while the horizontal part is carried along the back of the forearm.
Fracture of the Olecranon.—This fracture, if seen early before effusion takes place, may be put up at once, but if delay till the joint is swollen has occurred, the limb must be kept quiet on a pillow, or on a splint in an easy position with evaporating lotions, until the effusion is absorbed, before any means can be taken to restore the position of the olecranon. Though the straight position of the elbow is usually employed, it is not essential for even very close union of the fragments.
In treating this fracture the following plan is useful.
Apparatus.—1. Straight hollow splint.
2. 2-inch rollers and finger rollers.
3. Pad, wool, and lint.
4. Strapping plaster.
5. Pins.
Step 1. Bandage the fingers; wrap the hand in cotton wool and bandage it. When the wrist is passed, fasten the bandage for a time by a pin, and straighten the arm.
Step 2. Push the olecranon down as close as possible to the rest of the ulna, and put a dossil of lint over it. Place the middle of a strap of plaster an inch wide and 16 inches long, on the lint, and carry its ends round the forearm in a figure of 8; to some extent this alone fixes the fragment.
Step 3. Continue the bandage up the forearm by reverses, keeping the elbow straight; and pass the[Pg 46] joint by figures of 8 carried over the compress of lint and the forearm, to draw down the olecranon (see fig. 32). When this is secured, prolong the bandage to the deltoid, to confine the action of the triceps muscle.
Step 4. Pad lightly a hollow splint about 2 inches wide, reaching from the axilla nearly to the wrist, and apply it along the anterior aspect of the limb, then fix it by a second roller. This completes the apparatus.
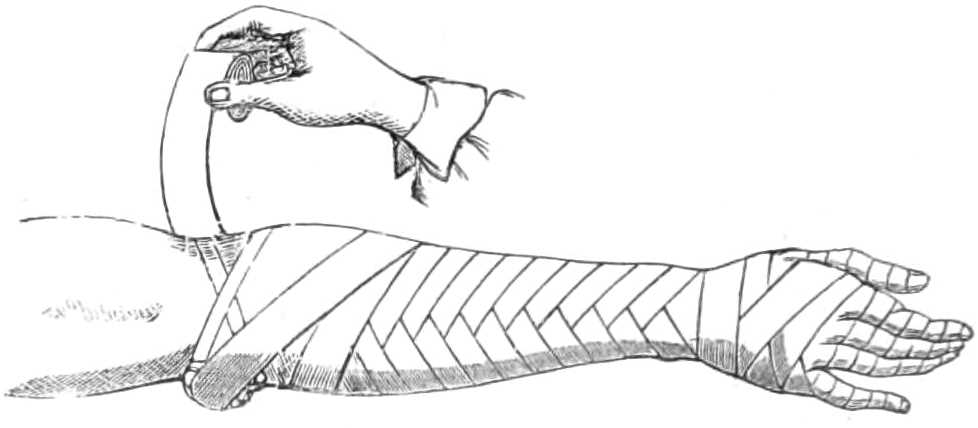
Fig. 32.—Bringing down the Olecranon with Figures of 8.
The splints and rollers should be removed on the fourth or fifth day, that the positions of the fragments may be examined and the roller again applied to draw them closer together. After ten or twelve days, passive motion of the wrist and fingers, with pronation and supination of the radius, should be adopted, but great care is to be taken that the patient does not inadvertently bend the elbow joint while free of the splint. The splint must be worn, with the frequent removals directed above, for five weeks, by which time gentle flexion of the elbow may be practised.
Hamilton notches his splint at each border about[Pg 47] its middle so that the notches shall be 3 inches below the tip of the olecranon (see fig. 33). He begins the bandaging by fastening his splint on to the hand and forearm, as high as the notches; here the roller is carried above the olecranon and again down to the notches; this is repeated again and again, each turn below the last, until the notches are all covered, he then continues the bandage upwards by circular turns until the top of the splint is reached.
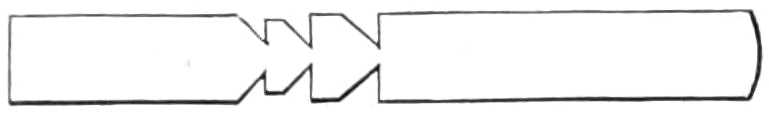
Fig. 33.—Hamilton’s Splint for fracture of Olecranon.
Fractures of the Humerus near the Elbow.—These resemble dislocations of the ulna and radius backwards, but are distinguished from them by the ease with which the bones slip into place and again slip back from it when left to themselves; by crepitus; and, when the fracture is above the condyles, the common accident, by those projections retaining their natural relation to the olecranon. In children and youths the articulating surface of the humerus may separate from the shaft without carrying the rest of the lower epiphysis with them. In this rare accident the main distinctions from the usual fracture are, the projection of the olecranon behind the condyles; from dislocation, the absence of the hollow of the sigmoid notch, and facility of reduction.
In ordinary cases, where the deformity is reduced without much difficulty, and the injury to the joint is not severe, lateral rectangular splints of leather, hollowed[Pg 48] wood, or wire gauze, answer very well. These are placed both inside and outside the limb, and reach from the axilla and shoulder to the wrist. They are applied in the following manner:—
Apparatus.—1. Lateral hollowed angular splints.
2. Pads and wool.
3. Rollers 2 inches wide for the arm, and 1 inch wide for the fingers.
4. Sling.
Step 1. The splints must be prepared.
Wooden and wire gauze splints are double. One, inside the arm, reaches from the axilla to the wrist, the forearm being bent to a right angle. The other extends, on the outside, from the deltoid to the wrist. They are better if provided with hinges opposite the elbow, so that their angle can be altered, if desired, in the later stage of the treatment. Splints of wood or wire gauze must be evenly and lightly padded before application.
Step 2. Bend the arm to a right angle with the thumb upwards. An assistant next reduces the fracture, and holds it in position. Then apply the splints. When adjusting the inside splint, care must be taken that the internal condyle is eased from pressure by sufficient padding above and below it. Next fasten on the splints by a roller begun at their lower end, leaving the hand free, and carried up to the elbow. Before turning round that joint a soft pad must be placed in the hollow of the elbow to push the lower end of the humerus back, and the length of the arm should be measured against the unbroken one to make sure that the shortening is reduced. Extension is kept[Pg 49] up the whole time the splint is being fixed to the arm, which is done by carrying the roller round the elbow with figures of 8 and simple spirals up to the axilla, where it is finished off.
Step 3. Lastly, the forearm is supported in a sling under the wrist, leaving the elbow free (as in fig. 35, page 52).
After three weeks of complete immobility, passive motion should be applied to the elbow daily, during a fortnight or three weeks more in which the splint is still worn.
If the displacement returns very easily, it is better to use an L-shaped splint passing behind the arm and below the forearm. This may be made of wood, or of leather, or of gutta-percha, in the mode about to be described.
The L-shaped splint of gutta-percha, or leather, is made as follows:—
Apparatus.—1. Sheet gutta-percha ¼ inch thick.
2. A tray or wide wash-hand basin.
3. A basin of cold water.
4. A kettle of boiling water.
5. A towel.
6. A knife.
7. A sheet of newspaper.
Cut a pattern of paper reaching, while the elbow is bent and the thumb upwards, from the arm-pit down the back of the arm and under the elbow and forearm to the wrist. The sides must be brought forward to the biceps and front of the forearm as seen in fig. 34. Next cut from the sheet of gutta-percha a piece to match the pattern. Prepare the tray with the hot[Pg 50] water, lay in it the towel, and then soften the gutta-percha by laying it in the tray and covering it with almost boiling water, adding more water as the first cools; this may be done by an assistant, while the surgeon directs another assistant to grasp the forearm and reduce the fracture. The assistant keep extension while the surgeon lifts the softened gutta-percha with the towel from the hot and plunges it a moment into cold water, then lays it on the limb, which the assistant keeps at a right angle, and the bone in place, while the splint is setting to the limb. This done, the splint is removed to be trimmed, perforated, and covered with wash-leather. It is then ready for use.

Fig. 34.—Gutta-percha Splint for fracture at the lower end of Humerus.
Leather takes so much time to set that it should not be used in recent fractures. When the bone is partly set, leather is a useful substitute for wood. It is prepared from a pattern in the same manner as the gutta-percha, but is trimmed before soaking, not after it is moulded, like gutta-percha. If possible it should have twenty-four hours soaking in water before being fitted to the limb; but when this cannot be done, immersion in hot water, into which a teacupful of vinegar has been thrown, will make the leather quite[Pg 51] supple in a quarter of an hour. The leather splint must be worn twenty-four hours while it sets, and then be removed for covering (see Leather Splints).
Fractured Shaft of the Humerus.
Apparatus.—1. Four straight hollow splints.
2. Rollers 2 inches wide, and 1 inch for the fingers, or straps and buckles.
3. Pads and wool.
4. Sling.
When broken below the attachment of the deltoid and coraco-brachialis muscles the displacement of the bone is commonly prevented with ease; neither shoulder nor elbow-joint need be fixed, and it is not necessary to apply the splints so tightly as to risk interference with the venous circulation. If the pectoral muscles or deltoid be connected with the lower fragment, the displacement is sometimes obstinate; in such cases it is necessary to buckle the splints lightly. For this to be done, the fingers, hand, and forearm must be previously bandaged to prevent œdema; with this addition, the method of treatment is the same in both varieties of fracture.
Step 1. Select the splints; they should be hollowed, of wood, perforated sheet zinc, or wire gauze, about 2 inches broad, lightly padded, and provided with straps and buckles.
The external one reaches from the acromion to the outer condyle; the inner one from the axilla to the inner condyle; a third shorter one is placed behind the arm, and if there is much projection forwards of the lower fragment, a fourth very short one is added[Pg 52] in front. The patient should sit on a chair while the apparatus is being put on.
Step 2. The fingers and thumb are bandaged; then, the hand and forearm, first padded with a little wool in the palm and over the wrist, are evenly bandaged to the elbow, round which the roller is carried while the joint is well flexed; this being covered in, the roller is made fast.
The first step of bandaging the hand and forearm before applying the splints is better omitted if the compression requisite to procure the natural position of the bone does not interfere with the circulation.
Step 3. An assistant grasping the elbow in one hand, pulls down the lower fragment, while he steadies the shoulder with the other. The displacement thus reduced, the surgeon applies the splints, taking care that the inside splint does not reach too high into the axilla, lest it compress the axillary vein.
In simple cases, the splints should be drawn close by straps and buckles; where the muscles are powerful, a roller should be wound round the splints instead of straps.
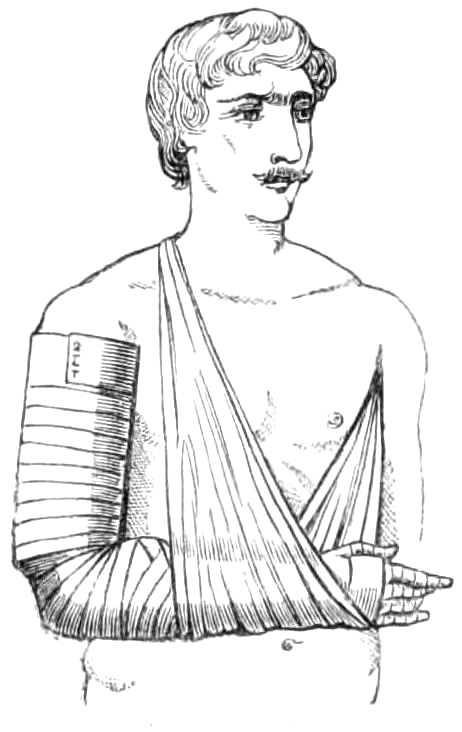
Fig. 35.—Fractured Shaft of the Humerus.
Step 4. A 2 inch wide roller is fastened to the arm above the elbow, and then carried round the trunk[Pg 53] to the arm again, to steady the limb against the body.
Step 5. The hand and wrist are supported by a sling over the shoulders, the elbow being allowed to hang (see fig. 35).
This apparatus is worn three weeks, when the bandages are removed from the forearm, and the splints replaced less tightly than before. They may be substituted by a sheath of gutta-percha moulded to the arm from the acromion to the elbow, and buckled on to the limb. The arm must be supported by splints for five weeks, but passive motion of the elbow and wrist should be adopted after the third week. The wrist especially should be set at liberty as soon as possible. In treating this fracture great care is necessary that the bone be kept in accurate and close position, as the humerus is specially prone to remain un-united for many months.
Fracture of the Anatomical or Surgical Neck of the Humerus, of the Great Tuberosity, and of the Neck of the Scapula. These fractures are similarly treated.
Apparatus.—1. Paper for pattern.
2. Gutta-percha, leather, or millboard.
3. Pads. A soft thin pad, 10 inches long, 5 inches wide (a double fold of thick flannel or blanket answers very well), is wanted to line the axilla. If the cap is of leather or gutta-percha, a lining of wash-leather should be added after the splint is made.
4. Rollers, 2 inches and 1 inch wide for the fingers.
5. Scissors.
6. A tray, and kettle of hot water.
[Pg 54]
7. A towel, and basin of cold water.
8. Sling.
9. Cotton wool.
Step 1. Cut out a paper pattern of the splint on the limb to be fitted. The pattern should reach along the clavicle to the root of the neck, and over the scapula to its posterior border, and be continued down the arm to the elbow, tapering as it goes, but having its anterior and posterior margins brought sufficiently to the inner side of the arm to give the splint a good grasp of the limb in descending. The end should be left long enough to turn a couple of inches round the point of the elbow (see fig. 36). A notch must be cut at the upper end of the paper pattern to make it fit on the shoulder between the clavicle and the spine of the scapula; this should not be repeated in the gutta-percha, as that can be moulded on without; and for that reason the cap is much more serviceable when made of gutta-percha than of leather, where a notch must be cut and stitched together when the leather is set. The gutta-percha, when cut to pattern, must be softened in the manner described in making the splint for the elbow at page 50, fig. 34; then accurately adjusted to the shoulder as high as the root of the neck, and turned under the point of the elbow a couple of inches (see fig. 36), while the forearm is well raised across the chest.
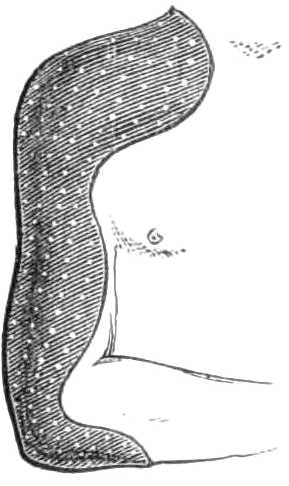
Fig. 36.—Cap for fracture near the Shoulder.
When set, the splint must be removed that it may[Pg 55] be trimmed and lined with wash-leather. If of gutta-percha, it must be perforated with small holes; if of leather, the notch at the shoulder must be stitched together. Next prepare a soft thin pad, 5 or 6 inches broad, and 8 or 10 inches long, to fill the axilla.
Step 2. Bandage the fingers and thumb separately, then, putting a little wool in the palm and round the wrist, bandage the hand and forearm to the elbow, where the bandage is fastened.
Step 3. Apply the splint. First get on the cap; then put the soft pad in the axilla, filling it out if the arm-pit is very hollow with cotton wool, and bend the elbow till the hand lies on the breast of the opposite side. Then, while an assistant holds the limb and apparatus in position, fasten them all in place by continuing the roller of the forearm in figures of 8 round the elbow until the splint is well fixed to it; and carry the roller up the arm by reverses to the axilla.
Step 4. A little wool or piece of flannel having been placed in the opposite arm-pit to prevent chafing, a spica for the shoulder is then applied (see page 16), beginning at the root of the neck and working downwards. Careful extension is continued by the assistant all the time this bandage is being put on, until the head of the bone is well drawn into the cap.
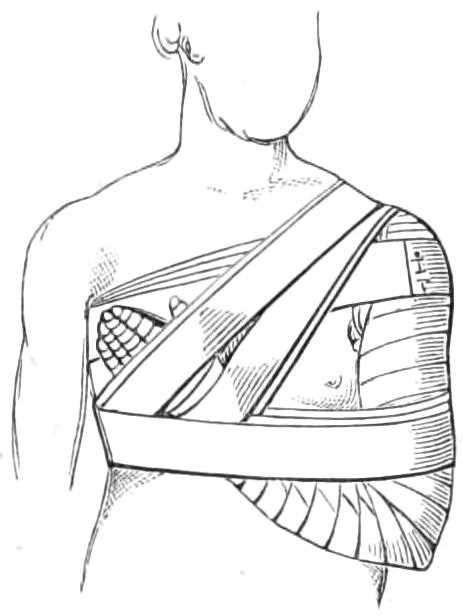
Fig. 37.—Fracture at the upper end of Humerus. The apparatus completed.
[Pg 56]
Step 5. The arm is drawn to the side, and the forearm fixed against the chest by a roller carried round the arm and trunk and over the shoulder (see fig. 37).
After three weeks the forearm may be released, but the cap and axillary pad must be continued to be worn two or three weeks longer while the arm is well drawn to the side, and the wrist carried in a sling.
Fracture of the Great Tuberosity of the humerus is difficult to treat, on account of the tuberosity being carried backwards by the muscles and the humerus being rotated forwards. Hence the parts must be braced together with a firm cap of gutta-percha moulded on to the shoulder while soft, and while the fractured parts are held in apposition, which may be done by the fingers, or by putting on a wet roller firmly over the shoulder as a spica before the splint is set. When the splint is hard the bandage may be taken off, and the splint removed and finished ready for application. In doing this, the steps are the same as for fracture of the surgical neck of the humerus, and the necessity for fixing the arm well to the side of the body as great as in that fracture.
Fracture of the Acromion is treated very much like fracture of the clavicle, that is, the arm is well raised by a sling under the elbow, and then fastened to the side. It is not necessary to fill the axilla with a pad, as in fracture of the clavicle, for in this case the shoulder is not drawn inwards.
Fracture of the Clavicle.
Apparatus.—1. Axillary pad.
2. Roller, 3 inches wide.
3. Sling.
[Pg 57]
4. Wool.
Fractures of the clavicle nearly always leave some deformity after union; this is best avoided by keeping the patient on his back on a flat couch with the head alone supported by a cushion, and the arm fixed to the side until union has taken place. As most persons will not submit to a fortnight or three weeks’ confinement in bed for this accident, the fragments must be kept in position as nearly as possible by apparatus while the patient goes about.
The displacement of the outer fragment is inwards, downwards, and forwards. Many varieties of apparatus are employed to prevent this displacement during union; the following mode is perhaps as effectual as any other in accomplishing this object.
Step 1. Fix in the arm-pit a firm wedge-shaped pad of bedtick filled with chaff; 5 inches broad, 6 inches long, and 1½ or 2 inches thick at the thick end, or just enough to fill the axilla and throw out the humerus without compressing the axillary vein, hence the thickness varies with the hollowness of the axilla (see fig. 38). A band and buckle are stitched to the thick end, which is uppermost. When in use, this band is passed over the opposite shoulder and keeps the pad in place. A little wool should be put under the band, where it crosses the root of the neck, to prevent chafing.
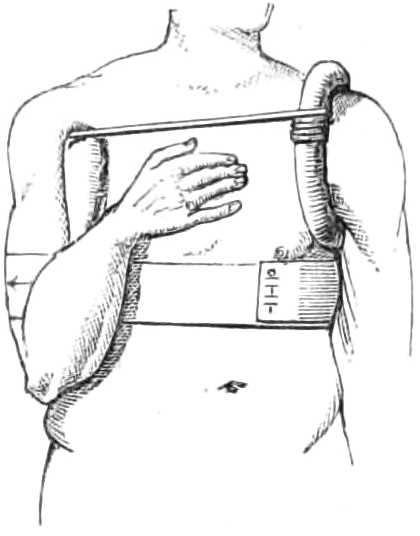
Fig. 38.—Wedge-shape pad for broken Collar-bone, attached to the American ring-pad.
[Pg 58]
Step 2. The elbow is elevated by an assistant, who keeps the arm vertical and lays the fingers on the breast bone. A roller attached to the arm by a couple of turns is carried behind the back round the trunk, and over the arm above the elbow, drawing that close to the side.
Step 3. To support the elbow, the longest border or base of a three-cornered handkerchief is carried under it, one end passes in front, the other behind the body; both are then drawn tightly and crossed over the opposite shoulder, where one end is taken under the axilla, and tied in front. In giving this direction the ring-pads shown in the figures are supposed not to be at hand. Lastly, the loose corner at the wrist is folded neatly and pinned up (see fig. 39).

Fig. 39.—Apparatus for broken Clavicle finished.
This apparatus must be watched from time to time, and re-adjusted if any part slips. The sling and pad are to be worn for four weeks.
Union sometimes takes place in three weeks or less, in which case the pad may be removed so much the earlier; but a sling should be worn for a fortnight after the bandage and pad are laid aside. In children the pad must be very much thinner and shorter than that described; the sling should be replaced by a bandage carried alternately round the body, and over the opposite shoulder. After it is put on the turns[Pg 59] should be well stitched together, and smeared over with stiff starch. In bandaging children, great care must be taken to protect with wool the parts likely to be chafed.
Figure-of-8 bandage.—Many surgeons still employ a figure-of-8 bandage carried under each axilla and crossed behind the back. Under any circumstances this is exceedingly irksome to the patient, but is least so if two silk handkerchiefs be substituted for the bandage, one being passed round each shoulder and the ends of both braced tightly together behind the back. The wedge-shaped pad may be dispensed with if the shoulders are braced back, but the elbow must still be raised and drawn to the side.
The American surgeons have a very good plan for attaching the sling to the sound shoulder. Instead of carrying the ends of the sling round the shoulder and under the axilla, they pass over the shoulder a loose but well-stuffed collar or ring-pad (see fig. 38), to which they fasten the ends of the sling in front and behind; this prevents all cutting or chafing under the armpit, and distributes the strain evenly.
Ruptured tendo Achillis is treated by extending the foot and flexing the knee; for this purpose the patient wears a high-heeled slipper. A band is sewn to the heel, drawn tight, and fastened to a buckle and strap round the thigh, just above the knee. The patient should not walk for a month unless he will[Pg 60] use a wooden leg on which he can kneel, with the knee bent.
Separation of the Epiphysis of the Calcaneum, which sometimes occurs instead of rupture of the tendo Achillis, is treated in the same way.
Fracture of the Fibula.—Dupuytren’s Splint.—When the fibula only is broken, it may be treated in several ways; this, however, is the common plan:—
Apparatus.—1. Straight wooden splint.
2. Pad and wool.
3. A roller.
Step 1. The splint should be about 3 inches broad, and long enough to reach from the head of the tibia to 4 inches beyond the sole of the foot. A notch 1½ or 2 inches deep is generally cut at the lower end of the splint to catch the bandage in. The splint is then padded, care being taken that the padding is sufficiently thick to prevent galling at the upper end against the inner condyle of the tibia, and that it becomes thicker as it descends along the leg, for that to rest easily against the splint; lastly, the pad should end in a thick boss or projection opposite the internal malleolus, beyond which it should not reach, lest it interfere with the rotation and adduction of the foot inwards.
Step 2. The splint, when thus prepared, is applied along the inner side of the leg, taking care in doing this that the internal malleolus is against the middle of the splint, and not allowed by the assistant to slip towards the anterior or posterior border.
Step 3. A roller is then carried round the limb and splint, beginning below the knee and continuing in[Pg 61] simple spirals for three or four turns, when it is fastened and cut off.
Step 4. A light layer of wool is wrapped round the outside of the ankle, heel, and dorsum of the foot. Then a roller, beginning at the splint, passes outwards in front of the ankle over the external malleolus, behind the heel and the splint; then over the dorsum to the outer margin of the foot, next under the sole through the notch of the splint to the front of the ankle joint again, where it repeats the same course three or four times. Each turn must be tightly applied and made to draw the foot well inwards to the splint, and in doing so to tilt outwards the broken part of the fibula (see fig. 40).
This splint is cumbersome, hence after two or three weeks, should be replaced by a light starch or gum casing for the foot and leg, leaving the knee free.
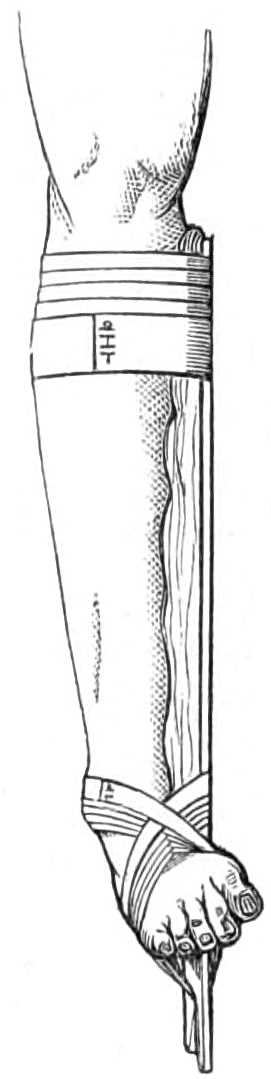
Fig. 40.—Dupuytren’s Splint for fracture of the Fibula.
Fractures of the Tibia with or without the fibula, and fractures at the ankle joint.
These fractures are often from their obliquity difficult to keep in good position; in such cases McIntyre’s Splint is very generally used in the early part of the treatment. For this splint the following apparatus is required:—
1. McIntyre’s splint.
[Pg 62]
2. Pads for the double incline plane and foot-piece.
3. Sock of flannel for the foot.
4. Rollers, 3 inches wide.
5. Wool, pins, needle and thread, strapping plaster.
6a. A sling-cradle, or
6b. Board, block, gimlet, screws and screw-driver.
The McIntyre’s Splint may be used either bent or straight, whichever position of the knee most relaxes the tension of the muscles on the fragments. As a general rule the straight position is best if the fracture is high up, and the bent one, when near the ankle joint.
Step 1. A splint of suitable length is selected, by measuring the sound leg. The joint of the splint should be put opposite the patella, and space be left below the foot for the foot-piece to slide along the slot when extension is made.
The splint is next padded, the hollow where the lower part of the calf and small of the leg will come being well filled, that the leg may be thoroughly supported; but the space behind the heel and tendo Achillis must be left quite clear. A small pad is then fastened by a strip of strapping or by needle and thread to the foot-piece.
Step 2. The limb having been first cleaned and dried, the dorsum of the foot and ankle are wrapped in an even layer of cotton wool. A sock or boot made of flannel is next put on the foot. This may be readily extemporised by cutting off the foot of an angola stocking, slitting it up along the back to the toes, and sewing on to the sole, one inch in front of the heel, the middle of a piece of tape ¼ inch wide and 18 inches[Pg 63] long. The foot is then wrapped in the sock, the edges drawn together by a needle and thread, care being taken that the sock fits closely round the ankle and dorsum of the foot. A little wool having been wrapped round the knee, the limb is next raised, while the splint is placed under it; the screw is turned until the inclined planes are at an angle suited for the maintenance of the fragments in position, and the foot-piece is pushed up to the foot with its screw-pin loose, that it may be adjusted to the amount of flexion or extension necessary for the foot; this being ascertained, the screw is tightened to keep it so while the foot is fastened to the foot-piece. For this the strings of the sock are brought over the top of the foot-piece, and drawn tight before tying them.
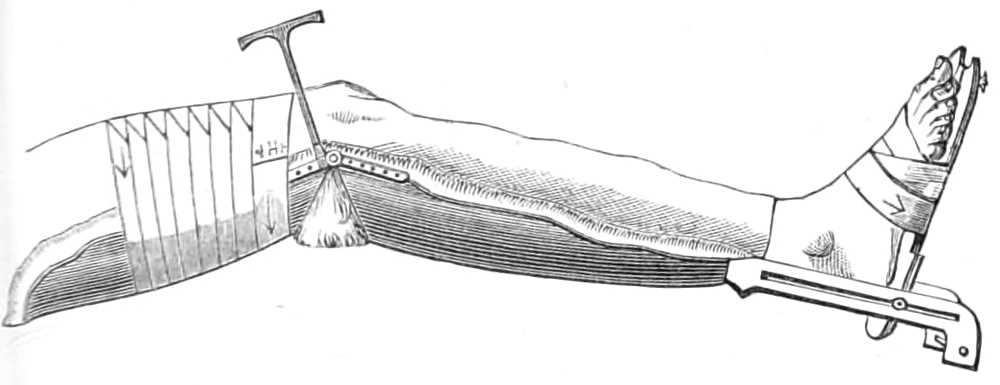
Fig. 41.—McIntyre’s Splint. The thigh fixed ready for extension of the leg.
The position of the heel is very important. It should not sink below the splint, or it will rest on the bandage; neither should it be drawn up too high, or the weight of the leg will hang on the sock, instead of resting on the pad; both frequent causes of pain at the heel. When the proper position is obtained, the strings are made fast to the pin behind the foot-piece,[Pg 64] and the foot is steadied by two or three turns of a roller carried round it and the foot-piece (fig. 41).
Step 3. The thigh is next fastened to the thigh-piece by a roller carried from the top of the splint downwards along the thigh to the knee, or below that joint if the fracture is near the ankle.
In doing this the roller is passed inside the screw, should that be placed underneath the splint, as in fig. 43 page 65, and not at the side as in fig. 41, for the screw will be wanted free for further adjustment.
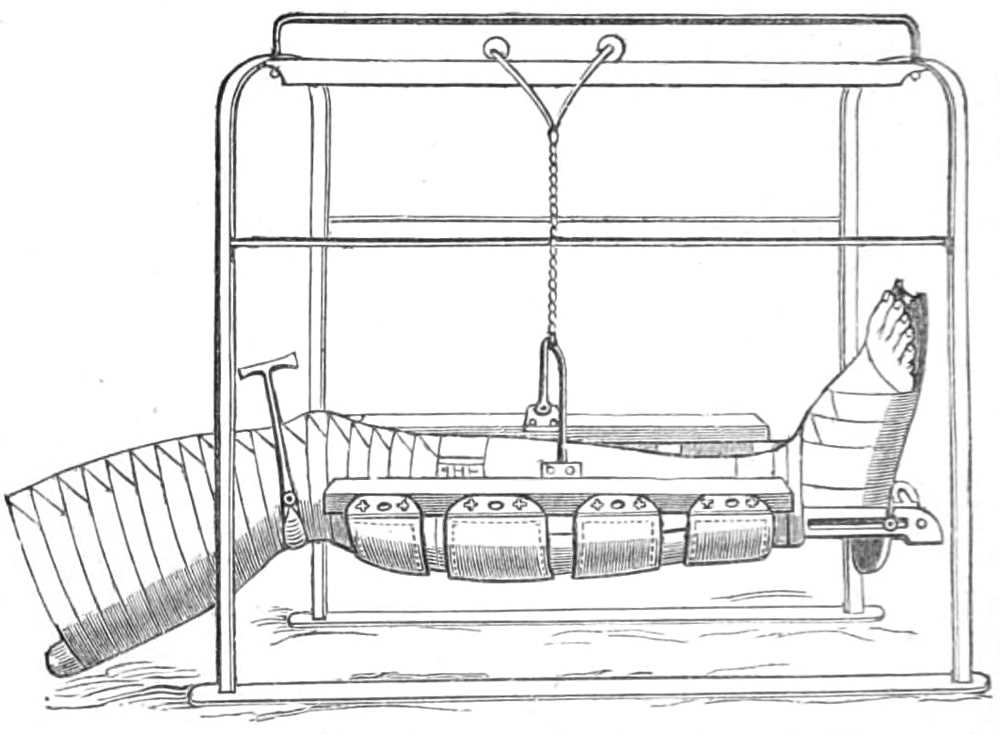
Fig. 42.—McIntyre’s Splint slung in Salter’s Cradle.
Step 4. An assistant grasps with both hands the foot and foot-piece, and pulls them downwards until the shortening is removed. While doing this, he tilts the foot up or down as the surgeon finds necessary for adjusting the fragments, who also bends the knee and raises or lowers the foot until a good position is attained. The general rule is to keep the great toe in a[Pg 65] line with the patella. This done, the surgeon tightens up the screw-pin of the foot-piece, and completes the attachment of the foot by continuing his roller with figures of 8 round the foot and ankle; these turns should not however pass above the fracture, and be no more than sufficient to secure the position of the foot and of the lower fragments (see fig. 42).
Step 5. The bandaging usually ceases with what has been already done; but if the limb swell, a separate roller may be carried along the leg to support the muscles and restrain œdema, otherwise the leg is best left bare, that the position of the fragments may be watched, and evaporating lotions applied.
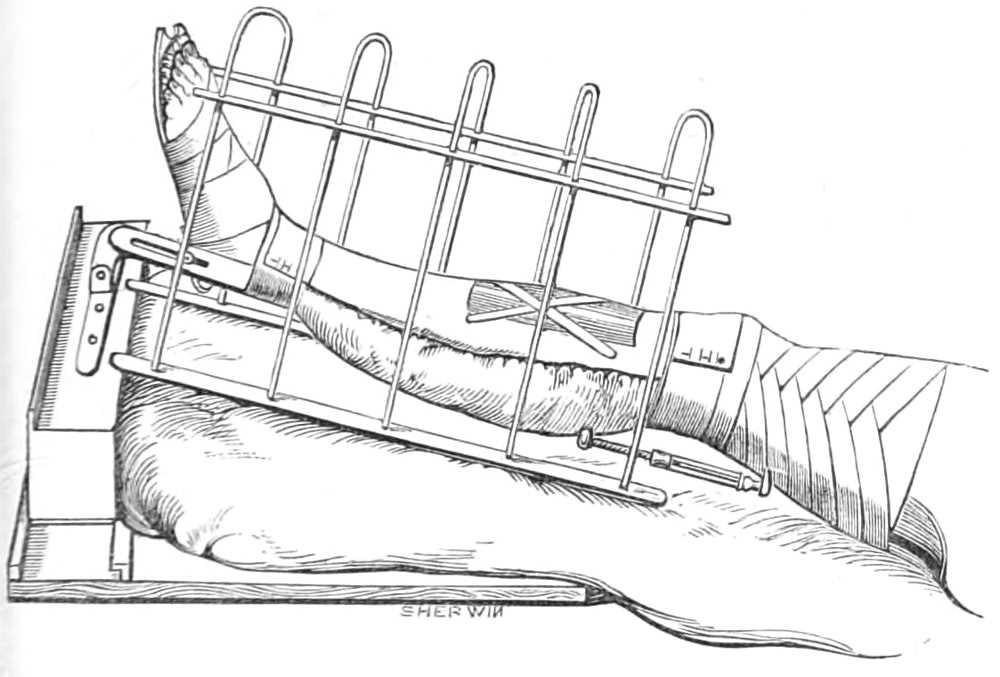
Fig. 43.—McIntyre’s Splint raised on a Block.
Step 6a. This consists in slinging the limb, for which Salter’s Cradle is very convenient (see fig. 42), or an ordinary bed cradle answers very well, from[Pg 66] which the limb can be slung on pieces of bandage carried underneath the splint at the knee and ankle.
b. Instead of elevating the limb by a sling, it is also customary to raise and fix the splint on a block (fig. 43), 6, 8, 10, or even 12 inches high, as may be necessary; this block slides in a groove on a board 3 feet square, put between the mattress and bedstead, to afford a firm support for the block.
In ordinary cases the limb is kept on the splint three weeks, until the irritation has subsided, and partial union is attained; the splint may then be replaced by a starch bandage, and the patient may leave his bed.
Transverse Fracture of the tibia alone, or even of both bones, when the displacement is small, is very well treated by a hollow splint on each side. Both splints are cut away opposite the malleoli, and the foot-piece of the inside one should not extend beyond the tarsus; that of the outside passes to the toes. The splints reach on each side to the head of the tibia, but ought not to extend above the knee-joint (see fig. 44).

Fig. 44.—Outside lateral Splint for the Tibia.
Step 1. They are padded lightly and evenly along their whole length, and applied to the limb on each side.
Step 2. They should then be fastened by figure of 8 round the foot and ankle until the foot is securely[Pg 67] fixed in them. The bandage should then be fastened off, and extension made by an assistant, who grasps the foot and ankle with both hands while the surgeon fixes the splints to the limb above the fracture, beginning his roller at the top just below the knee, and continuing it downwards with spiral turns until the fracture is reached, above which it should terminate (fig. 45). After the apparatus is applied, the limb may be either supported upright by sand-bags, or slung in a cradle, for three weeks, after which the splints are advantageously replaced by a starch bandage for three weeks longer.
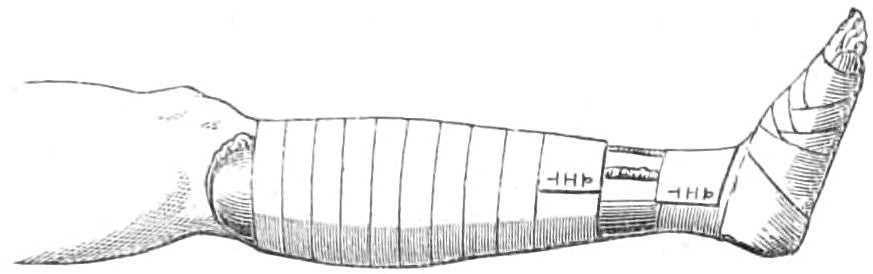
Fig. 45.—Lateral Splints for simple transverse fracture of the Tibia.
Flexing the Leg for Fracture of the Tibia.
Sometimes, when there is unusual difficulty in preventing displacement of the fragments while the limb is nearly straight, the bones can be readily kept in position if the patient lies on the same side as the injured limb and the knee is well flexed. For such cases these splints are very suitable; they should be applied after the limb has been bent and the fragments brought into apposition. When the splints have been put on, a roller may be carried round the leg and thigh to keep the limb in its bent position.
Fracture of the Patella.—When this bone is broken there is usually much swelling from effusion[Pg 68] into the knee-joint; while this is present, rest, with cold lotions, and elevation of the foot, are alone applicable. When the effusion has subsided, the upper fragment must be brought down to the lower one, by some means like the following.
Apparatus.—1. Straight wooden splint with a foot-piece.
2. Pads.
3. Diachylon plaster.
4. Roller.
5. Lint and wool.
6. Two hooks or screws, gimlet, and screw-driver.
Step 1. The splint is first fitted; it should reach from the buttock to the heel, at which point a foot-piece rises for the foot to rest against; at the back of the splint a line should be marked 3 inches above, and another 3 inches below the knee-cap, into which a stout screw or hook is inserted before the splint is put on. It is then well padded, to support the calf and leg, while the heel is left free, and a pad is put between the sole and the foot-piece. A firm crescent-shaped pad is prepared to sit like a saddle above the upper fragment.
Step 2. The limb is laid on the splint; an assistant draws the patella as nearly as possible into its place, and the surgeon lays the crescentic pad on the thigh above the patella, and takes a strap of plaster 2 inches broad and 20 long, warms it, and lays the middle across the compress, drawing each end tightly around the limb, and then downwards and forwards in a figure of 8; a similar strap is then fixed below the lower fragment. The knee, shin, ankle, and foot are then[Pg 69] protected by a layer of cotton wool, and the bandaging begins.
Step 3. The roller first fastens the foot against the foot-piece by figures of 8, then passes up the leg by reverses until opposite the lower hook, where it is fastened.
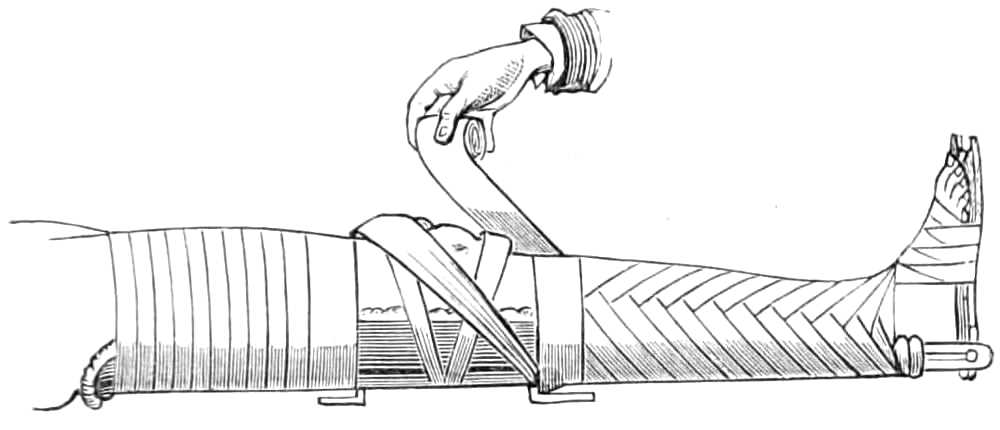
Fig. 46.—Fractured Patella, drawing down the upper fragment.
Step 4. A second roller is then begun at the top of the thigh and brought down the limb till it reaches the compress over the patella; from this point it passes below the lower screw at the back of the splint and makes one circular turn round the limb; the roller is then taken upwards across the compress (as shown in fig. 46) to the upper screw, where it also makes a circular turn; having done this it again descends to reach the lower screw, and is returned as before. Each of these turns should be drawn tightly to bring the upper fragment as near the lower one as possible; when this is done the bandage is completed over the knee by figures of 8. It suffices to fix the lower fragment, which cannot be drawn up to meet the upper one; the latter must descend to it.
Step 5. The limb is lastly put into position by[Pg 70] elevating the heel and by raising the body with pillows till it is in a half-sitting position.
The patient wears this splint four weeks, during the first fortnight of which the bandage should be perseveringly re-applied every three or four days until the upper fragment is brought into apposition with the lower one. After this the splint may be changed for a light starch or gutta-percha case, to be worn for six weeks more, and then replaced by a back splint of leather and knee-cap, that must not be laid aside for another period of three or four weeks. If the patient can be persuaded not to bend his knee for four months, the union of the fragments will be less likely to yield afterwards. He should be also warned that much stiffness will result from the long fixed position necessary to procure good union between the fragments; but the stiffness will all subside in time, notwithstanding the long-enforced rigidity.
Strap and Spiral Bandage.
E. K. Samborne’s Plan of drawing Patella Fragments together.—A strip of diachylon plaster 4 feet long and 2½ in. wide is applied to the front of the limb from 2 in. below the groin to the small of the leg, leaving a free loop or doubling opposite the patella. Beneath this loop a firm compress or horseshoe pad is placed above the upper fragment. A roller is then carried round the limb to keep the strap in place, but leaving the loop at the knee exposed. This done, the body is propped up in a half-sitting position, and the limb elevated on an incline. A stick, 6 inches long and ½ inch thick, is inserted into the loop of plaster, and then twisted[Pg 71] round and round till, by shortening the loop, the loose tissues of the thigh, and with them the upper fragment of the patella, are drawn down to the knee. The stick is prevented from untwisting by a roller lightly carried round the knee. As the plaster slackens, the stick may be tightened from time to time and the fragment brought in a few days into its proper place.
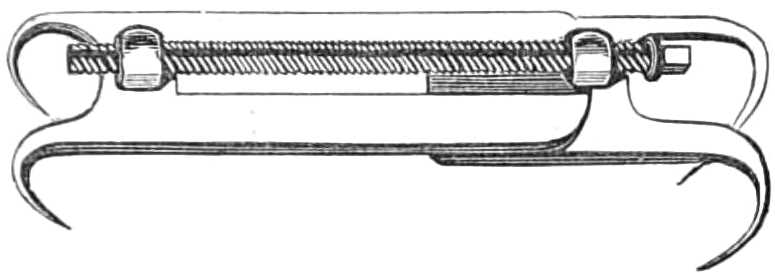
Fig. 47.—Malgaigne’s Hooks.
Malgaigne’s Hooks (fig. 47), for drawing closely and holding together the fragments in transverse fracture of the patella, or of the olecranon, often procure a closer union than any other method. They should not be inserted until effusion is absorbed and the soreness has subsided. To insert them, one pair of hooks should be bedded in the ligamentum patellæ, and catch against the lower edge of the bone; the skin is then drawn up the limb, while the upper pair of hooks is passed through it and behind the upper fragment; the two ends are then approximated by turning the screw. The fragments usually do not come quite close the first day, but the next they can be drawn so firmly together that if one is moved the other goes with it. In applying the hooks care should be taken that the upper pair go well through the skin and fascia behind the bone, or when they are screwed up the upper fragment is apt to ride unevenly over the other, and exact junction is lost. The pain of the insertion soon passes off, and the hooks[Pg 72] can commonly be worn without annoyance for five or six weeks, until union is secured.
Fracture of the Shaft of the Thigh-bone.—The long Splint.
Apparatus.—1. A wooden splint.
2. Rollers, 3 inches wide.
3. Perineal band.
4. Strapping, needle, and thread.
5. Pad and wool.
The splint for an adult should be 2½ or 3 inches wide, and long enough to reach from the nipple to 4 or 5 inches beyond the heel; two round holes ¾ inch diameter are cut at its upper end, and at the lower one two notches 2 inches deep.
Liston’s Mode of applying the Long Splint.
Step 1. The end of a roller is split for a few inches, and tied in the holes at the upper end. The roller itself is carried down the inside of the splint and attached temporarily to the notches at the other end; a pad is then fastened on, by drawing the margins together with needle and thread across the outside of the splint, or by tying strips of bandage round the pad and splint at short distances.
Step 2. The limb having been washed with soap and water, well dried, and afterwards dusted with starch powder, especially at the perinæum, the ankle and dorsum of the foot are wrapped in a layer of cotton wool, and the splint applied along the outside of the body. The bandage which was fastened to the splint is now released from the notch; and, taking with it the end of the pad, is carried under the sole, then over the ankle joint to the splint, and behind the ankle round[Pg 73] the internal malleolus to the dorsum of the foot, then through the lower notch of the splint to the inside of the foot again. This figure of 8 is carried four times over the dorsum of the foot, twice through each notch of the splint, and is made fast by a pin or a stitch. In doing this, care must be taken to keep the leg and splint parallel, and that the splint does not ride over the back of the foot; the external malleolus should be midway between the margins; moreover, the bandage must fit firmly round the ankle and splint, not spreading over the dorsum more than can be helped, to avoid straining the front of the ankle. Means for more effectually preventing this will be afterwards detailed.
Step 3. Next apply counter-extension; for this, the perineal band is used. The band consists of a silk handkerchief or napkin folded into a flat ribbon, 1 inch wide and covered for about 1 foot of its length with oiled silk. A piece of smooth brown paper, 1 foot long and 4 inches wide, folded into a ribbon one inch wide, makes an excellent foundation for the silk handkerchief to be folded upon. A band thus prepared is too stiff to become a cord after it has been worn a few days, which a simple handkerchief is apt to do. One end of the band is passed in front in the groin, and one behind the buttock, so that it bears on the tuber ischii in the perinæum; the ends are then drawn separately through the holes in the splint. All being ready for extension, an assistant, grasping the leg and splint above the ankle, pulls out the shortening till the broken bone is in a good position; the ends of the band are then tightened and made fast in a knot.
Step 4. First protecting the bony points with cotton[Pg 74] wool, the muscles about the hip are confined by a spica carried round the body and the splint, not merely a simple figure of 8 as depicted in the figure, but a series of overlapping turns which ascend and cover in the hips well. Afterwards the upper end of the splint is drawn close to the body by a few turns of a broad roller carried round the chest from above downwards (see fig. 48).
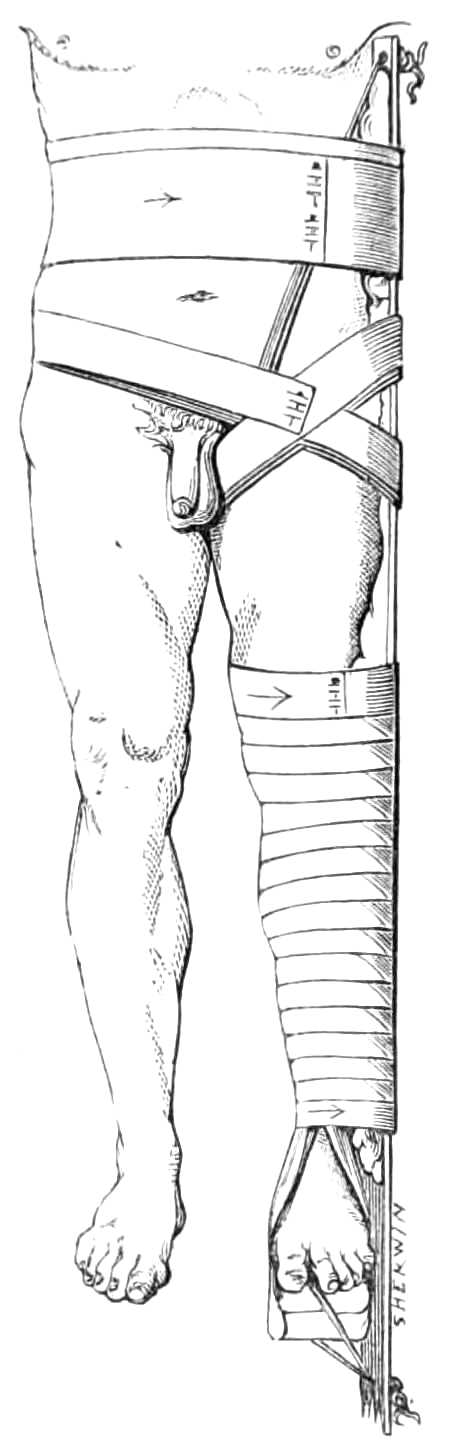
Fig. 48.—The long splint, with elastic stirrup extension at the foot. Bandage carried up to the seat of fracture.
Step 5. It is customary to carry the bandage further than the ankle, but this is not an essential part of the apparatus, which is simply to keep up the extension in the direction of the axis of the limb. This subsidiary bandage has the disadvantage of concealing the limb, and the position of the broken ends of the bone; but it steadies the limb on the splint, and confines the muscles, thereby preventing pain and perhaps hindering rotation outwards of the upper fragment. Before putting it on, some cotton wool is wrapped round the knee, and laid along the shin; the application of the roller is then begun at the[Pg 75] ankle where it first terminated, and is carried up the leg, over the knee, and along the thigh by reverses until the groin is reached, where it finishes.
The perineal band must be changed whenever it gets soiled, and the skin washed before a clean one is adjusted. After the first few days the band need not be very tight; it suffices if not slack or loose. Mr. Coxeter makes india-rubber tubes in the shape of a perineal band; these are filled with water when in use (see fig. 49).
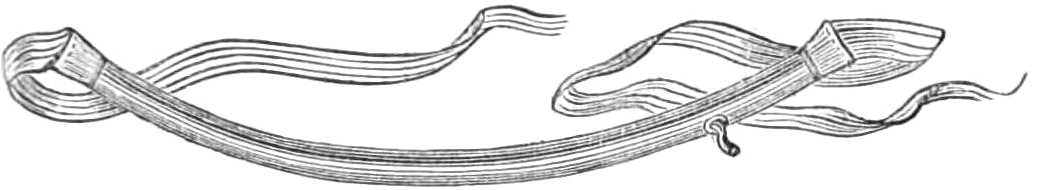
Fig. 49.—Coxeter’s elastic perineal band.
Stirrup extension is a mode of relieving the strain on the front of the ankle, caused by the lower end of the splint being attached to it. A 3-inch wide roller or bit of wood of the same breadth is laid against the sole of the foot, and a stout india-rubber ring 2 inches in diameter is slipped over it. A piece of strapping plaster, 2½ feet long and 2 inches wide, is passed half-way through the ring, and its ends carried up the leg inside and outside; the plaster is kept in place by a roller or second strip laid on in spirals up the limb as in fig. 50, and the india-rubber ring is hitched against a hook at the end of the splint. By this means the strain is transferred to the leg, and the ankle is quite free. It is perfectly successful, and very easy to the patient.
The long splint is to be worn continuously for six[Pg 76] weeks; or, what is better, after the first three weeks it may be replaced by a starch bandage, and the patient allowed to get about on crutches with his leg slung from his neck.
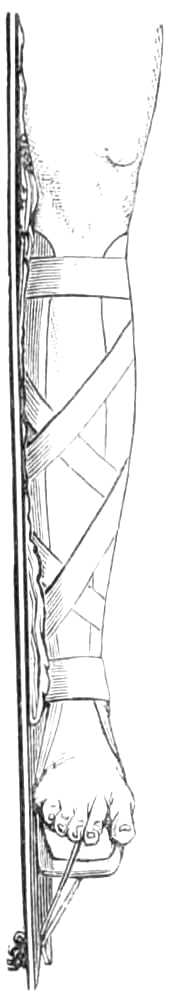
Fig. 50.—Mode of fastening the stirrup to the leg, to avoid straining the ankle.
Continuous Extension with the Limb flexed.—The muscles attached to the upper end of the femur sometimes cause so much flexion and rotation outwards of the upper fragment that union of the bones in this position produces a result approaching that in fig. 51, drawn from a preparation in the museum of University College.
This crooked union is prevented by bending the thigh and relaxing the muscles of the hip. This object is accomplished by using the double incline planes or the double incline planes, slung, shown in figs. 52 and 53.
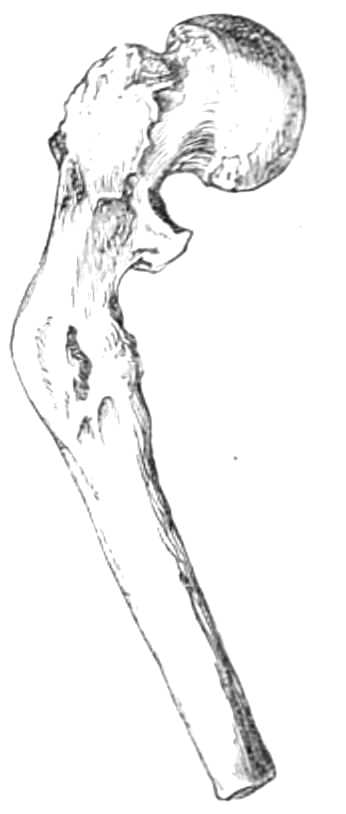
Fig. 51.—Fracture below the trochanters; bone in angular union.
Double incline planes are sometimes employed alone. The limb is raised over a wooden frame about 8 inches broad, with a double slope high enough at the apex for the leg and foot to hang unsupported down the further side (fig. 52). It is well padded before being applied, and the leg and thigh secured to it by a roller passed[Pg 77] round the limb and plane, or better, a trough of gutta-percha may be moulded to the limb while it is on the plane, and when set, screwed down to the wood at one or two points; in this the limb rests securely.
Fig. 52.—Double incline planes.
Slinging the double incline planes was practised many years ago by Mayor of Lausanne, and has been much used recently. It is an apparatus very easy for the patient, and particularly well suited for compound fractures of the thigh, for fractures near the trochanters that require a flexed position, or for fractures of the neck of the femur where the patient’s feebleness does not permit the constraint of the long splint.
Apparatus.—1. A bent wire frame (see fig. 53) with a separate foot-piece.
2. Two pulleys, a rope with tent stretchers passing up to hooks in the ceiling, or some suitable support.
3. One long and one short soft pad.
4. Strapping plaster, and some ends of bandage.
Step 1. The limb is washed and dried, and the short pad fitted to the foot-piece, which is furnished with some hooks at its lower surface, where ends of bandage or tape can be fastened, for fixing it to the wire frame. The frame is next prepared by passing strips of bandage[Pg 78] across it from side to side at short intervals, to make a support on which the limb is laid; if there is no wound, a soft pad may be put on the frame first, but if one be present, the limb should rest immediately on the strips of bandage, which can be changed whenever soiled, and replaced by clean ones without disturbing the limb. These strips should be tacked on with a needle and thread, that, when the limb is placed on the apparatus, they can be shortened or lengthened till the leg bears evenly on them (see fig. 53).
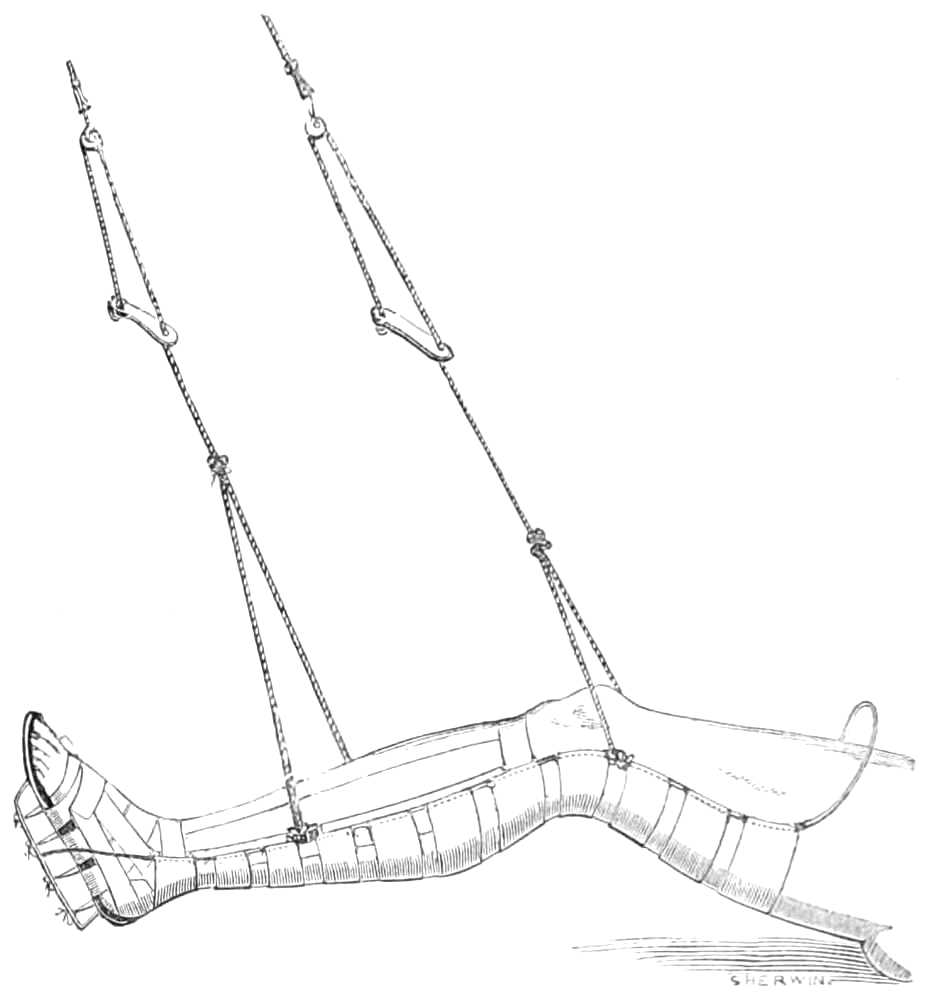
Fig. 53.—Double incline plane, slung.
[Pg 79]
Step 2. The foot-piece is adjusted and fastened to the foot by straps of plaster carried round it and up each side of the leg, as was done for the stirrup extension in the “long splint” (p. 76).
Step 3. The limb is next placed in the cradle formed for it, to the lower end of which the foot-piece is tied securely; the ropes are rove through the pulleys and tightened till the limb swings easily. The point of attachment of the ropes must not be just above the limb, but beyond it, that the leg may be drawn away from the body along its own axis. The weight of the body makes counter-extension sufficient to remove all shortening in a few days. The relief from the constraint attending the absolute immobility of the long splint, renders this apparatus a particularly easy one for the patient; and union is found to take place without any shortening of the limb. Where there is no wound, the limb and frame may be kept together by a roller bandage carried round them from the toes to the knee, after the limb has been adjusted in the splint.
Continuous Extension in the straight position is employed for fractures of the femur and in hip-disease. It is procured as follows. A stirrup is fastened to the leg in the way described at page 76; to this a cord and weight are attached below the sole of the foot, and passed over a pulley fixed to a tripod frame (fig. 54), or any convenient object below the bed, in a line with the axis of the limb. The weight should balance the contraction of the muscles, and usually varies between 2 and 6 lbs. A perineal band fastened behind the patient’s head keeps the body from following the limb. The weight may be a common scale weight, or a bag[Pg 80] with a hole at the bottom closed by a string, and filled with shot or sand, or a can with a tap at the bottom filled with water: these arrangements allow increase or lessening of the weight, without slackening the cord and moving the limb. This apparatus requires no bandages, which are so difficult to keep clean in children, and exerts a very even and continuous strain on the limb.
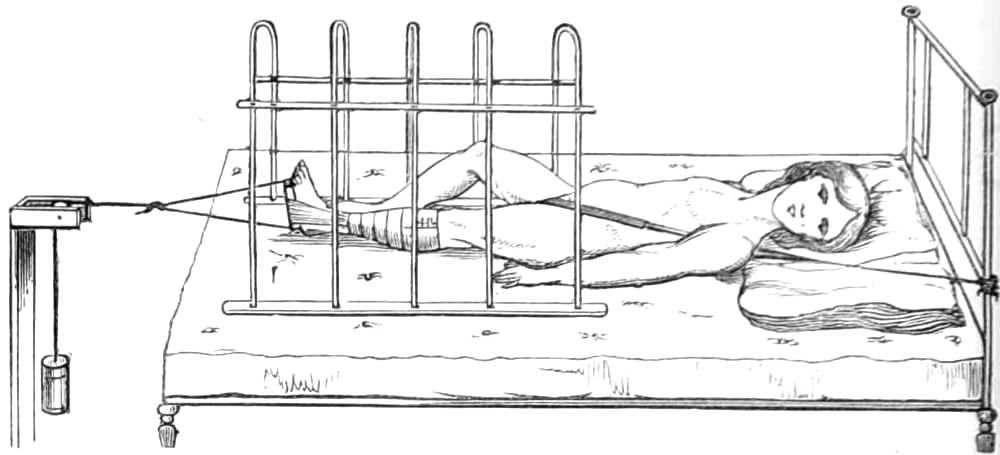
Fig. 54.—Fracture of the femur. Extension by weight and pulley.
The perineal band may be often dispensed with, by laying the patient on a flat mattress and raising the foot of the bedstead a few inches higher than the head; the body then sinks towards the head of the bed and resists the extension of the leg.
Starch Bandage.—The following mode of applying the starch bandage and pasteboard splints may be used in all varieties of fracture; the length of the splints and the number of joints that should be included depend on the bone that is broken.
Some surgeons apply the starch apparatus immediately after the fracture has happened, others wait until[Pg 81] partial union is procured and the irritability of the muscles has subsided.
Apparatus.—1. Sheets of bookbinder’s millboard.
2. Rollers suitable for the size of the limb.
3. Cotton wool.
4. A basin of freshly scalded starch.
5. A long strip of plaster, to reach as high as the bandage will extend up the limb.
6. If the fracture be recent, a wooden splint will generally be necessary to keep up extension while the starch is drying.
As a general rule, the joint at the lower end of the fractured bone should always be fixed, and that at the upper end also, if the fracture is near that point. For an example of the mode of fitting, let us suppose the femur is broken between the middle and lower thirds as in fig. 56.
Step 1. The limb is first measured for the splints. The length from the top of the sacrum to the heel, from the tuber ischii to the inside of the foot, and from the iliac crest to the outside of the foot, should be taken, and three strips of millboard prepared of corresponding lengths; the posterior one being 3 inches wide above and 2 inches, or, if the limb is small, 1½ inches wide at the heel. The inner and outer strips of similar width must be cut with side pieces for the foot, and these side-pieces stop short of the roots of the toes. For a child’s thigh, the foot need not be included, it suffices for the splints to reach the small of the leg, though to prevent shortening in an adult it is usually necessary to include the whole limb. The splints are readily cut, by first[Pg 82] marking on the sheet of millboard, the required width and length of the strips, then bending the sheet over the edge of a table along these lines. The two lateral splints may be first taken from the sheet in one wide strip, after allowing for the foot-piece; the two strips are separated through a diagonal line, so that the broad end of one splint is taken from the other (see fig. 55).
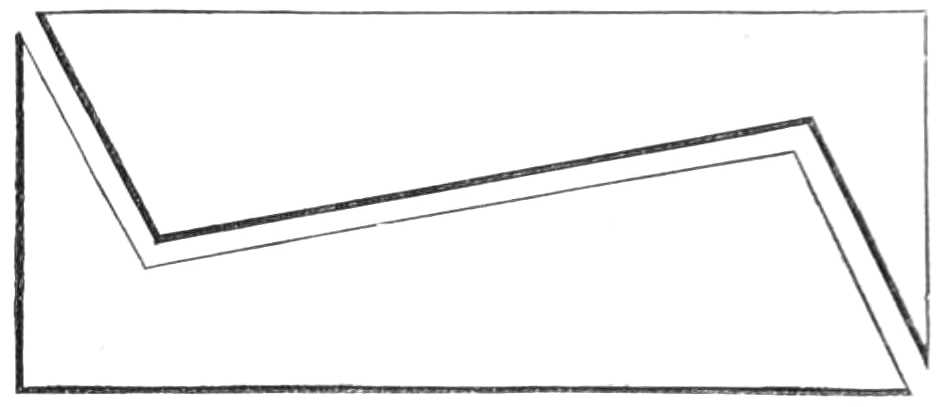
Fig. 55.—Diagram showing the mode of cutting out splints from a sheet of millboard.
When the strips are cut they should be laid on a large tea-tray, boiling water poured over them, and a minute or two later, some boiling hot thin starch; this soon soaks into and softens the millboard till it is thoroughly pliant. When somewhat softened, the edges should be thinned by peeling off little strips along them, after which some more boiling water may be poured on and allowed to soak in while the limb is prepared.
Two or three rollers should then be unwound, and passed as they are rolled up again through the basin of starch; these, thoroughly soaked in starch, are used for the first layer, dry rollers serve very well for the second layer.
Step 2. The limb is washed and dried; a strip of[Pg 83] diachylon plaster one inch wide is laid along the front to protect the skin when the case is being cut open after it is dry; the limb is next wrapped evenly in cotton wool, putting a scrap between each toe. This is best done by unrolling a sheet of wadding, splitting the sheet into a layer of suitable thickness, which is torn into strips about three inches broad, that are then wound evenly round the limb as high as the splints will reach.
Step 3. The splints are next adjusted and moulded to the limb, being temporarily secured by a few ends of bandage tied round them. One assistant grasps the splints and foot at the ankle and keeps up extension, while another holds the thigh. The surgeon then proceeds to roll the bandages, first round the foot and ankle, and then up the leg, rubbing in the warm starch as he proceeds. Each turn of the roller should be made as tightly as possible, for when the case dries it always grows loose by the evaporation of the water it holds. As reverses are always difficult to cut through afterwards, they should be avoided, and the bandage laid on in simple spiral or figure of 8 turns. When the perinæum is reached, the surgeon wraps round the pelvis a broad strip of cotton wool, while an assistant on each side of the patient supports his body on a folded sheet or jack-towel, and a third holds the broken limb. The bandaging is then continued in a well-fitting spica, and ended by a few circular turns round the body. If the splint touches the crest of the ilium it should be shortened till it clears that point, or it will gall the patient afterwards. A fold of soft lint in addition to the cotton wool should line[Pg 84] the splint at the perinæum, or the sharp edge of the bandage, when it is dry, will chafe there also. When the first bandage is complete, the limb should be smeared again with starch, and a dry bandage rolled over it from below upwards, which must be similarly saturated with starch as it is laid on the limb, and when finished the whole is well covered with starch.
If the fracture is recent, and no union has taken place, a long splint should be put on outside the case, fastened to the foot and extended by a perineal band, while the starch is drying, that the limb may not shorten. With children it is best to apply the wooden splint in all cases, as they are apt to wriggle about, or sit up in bed and disarrange the case while it is in a pliant condition. If the wood splint is not used, the limb should be supported in a good position by sand-bags laid along its sides.
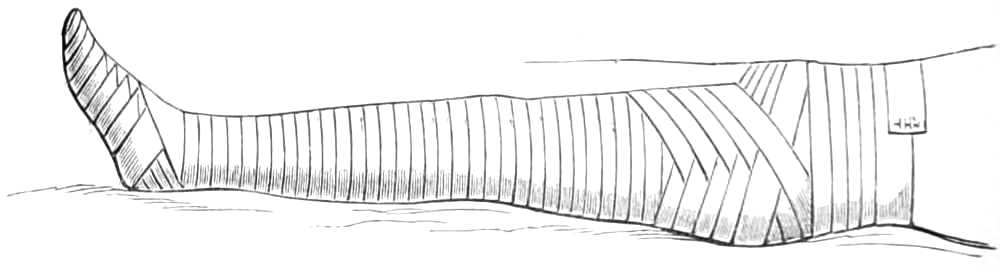
Fig. 56.—Starch Bandage.
In three days the starch is quite dry, but the drying may be hastened by hot-water bottles or hot sand-bags laid in the bed. It must then be cut up along the front from bottom to top; it will often be found loose, especially where swelling had existed before; this is best remedied by paring the overlapping edges with scissors. If any projecting part is chafed, an accident[Pg 85] that ought not to happen, the case may be lifted from the sore part by a little more wool laid around, not on the part pinched. The limb being in a satisfactory position, and the case fitting properly, a roller is carried up over the whole to keep it in place while it is worn (fig. 56).
The patient need not now be confined to bed; on the contrary, the limb should be supported by a sling round his neck, while he gets about with crutches, if his leg be the part injured.
The fracture should be examined from time to time, and at the end of three weeks some of the joints previously confined in the splint may be released by cutting off the part covering them; but if the part is a dependent one, such as the leg, it should be supported by a bandage after the splint has been removed. The limb may also be washed with soap and water, and then anointed with simple ointment, if the skin be roughened or irritated by long confinement.
In six weeks the starch splint may usually be discarded, and a roller alone worn for a few weeks longer.
Plaster of Paris Bandage.
Apparatus.—1. Freshly burned white plaster of Paris. If the plaster have become stale by keeping in improperly closed vessels, and it be impossible to obtain fresh plaster, the water the plaster has absorbed from the atmosphere can be driven off by heating the powder in a dry oven to about 200° F. to 260° F., but not higher, as greater heat destroys the power of “setting.”
2. Rollers, about 2¼ inches wide, of muslin with a coarse open texture.
[Pg 86]
3. A roller of Welsh flannel 3 inches wide and 6 yards long.
4. Basin of cold water, sponge, and a kitchen spoon.
5. Soft lard or spermaceti ointment.
Step 1. The muslin rollers are prepared by being loaded with dry powder just before they are used. To do this the roller should be gradually unrolled on a table while one person rubs in the powder, and a second rolls the loaded bandage up again. When three or four are loaded they should be plunged for a minute into cold water, and then are ready for use. While this is being done the limb should be thoroughly washed and dried, supported, if the fracture be recent, by sand-bags.
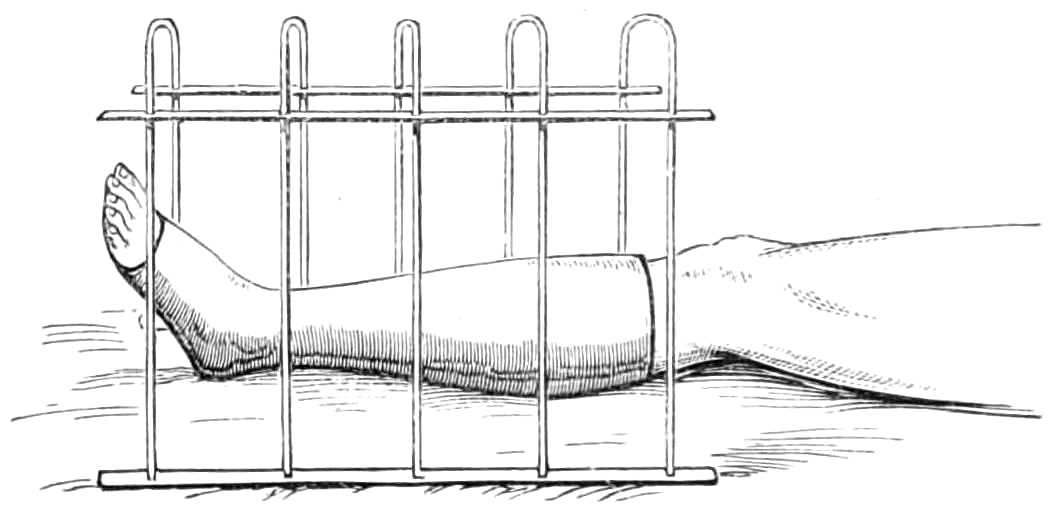
Fig. 57.—Plaster of Paris Bandage, for simple fracture of the tibia, and common bed cradle.
Step 2. The surgeon carefully greases the limb wherever the plaster will reach, and rolls a Welsh flannel roller round it for about 3 inches at the point where the plaster roller will cease. This protects the skin from the rough edge of the plaster splint when the apparatus is set and hard. Indeed, if the whole[Pg 87] of the surface to be covered with plaster be enveloped in a flannel roller, the apparatus is more comfortable to the patient, and in this case the grease may be dispensed with. When the limb is prepared the surgeon intrusts it to assistants, who will maintain reduction while he lays on the plaster rollers, wetting them freely as they are laid on, with a sponge at hand in a basin of cold water. Usually two layers of roller give sufficient rigidity to the apparatus; but if the limb is heavy, the case should be strengthened, by smearing over it a coating of plaster, prepared by shaking the powder into a basin of water kept constantly stirred, till it has the consistence of cream. The surgeon must watch that the fractured bones are kept in position till the plaster is set, a process sufficiently advanced in five minutes, when the bandage, supported by sand-bags, may be left to dry.
When the plaster is quite set the bone is immoveable and may be carried about without risk of displacement. In deciding what joints should be included in the bandage, the same rules obtain in this as for the starch bandage; no more joints should be rendered immoveable than are necessary to obtain command of the broken bone; when the fracture is near a joint, that must be confined to prevent the bones being moved with the movements of the joint; when the fracture is far away from it, sufficient control can be exercised over the bone to prevent the broken ends moving, and the joint may remain free.
If the plaster apparatus is applied over a wound, the latter should be covered with greased lint, and its position noted before the rollers are applied; when the[Pg 88] apparatus is set, the plaster must be dissolved around the wound by touching it with strong nitro-hydrochloric acid; when this is carried completely round, the isolated fragment of plaster may be removed, and the wound exposed.
For removal, the roller can be unwound again readily, or it can be softened by acid along a line, and slit up with scissors, when the apparatus comes off in a piece.
Should bandages of loose texture not be at hand, common rollers can be made to answer the purpose tolerably well in the following way.
Having washed and dried the limb, and reduced the fracture; the bones are held in position by assistants, while the limb is greased and enveloped in a dry roller by simple turns and figures of 8. A basin of plaster is prepared by shaking the powder into water till a thin cream is formed, which is laid on the bandage with a spoon, or the hands. Then a second but wetted roller is put on in the same way quickly before the plaster has set, and covered in its turn, until a case of sufficient thickness is procured.
This bandage is much improved if the first roller be of flannel instead of calico. The flannel roller may be unrolled and loaded with dry plaster, like the muslin, and wetted before using; in this way it contains nearly as much plaster as the loose webbing rollers of muslin.
In the Army Medical Reports for 1865 (1867), Mr. Moffitt describes a very ready method of employing the plaster splints for recent fractures. Instead of bandaging the limb, an envelope of Welsh flannel is fitted to the part to be supported.
The flannel should envelope the limb, except for a[Pg 89] longitudinal space about ½ inch in width between the edges of the flannel. The dotted lines in the accompanying figure show the shape of the flannel when fitted to the leg. The limb being thoroughly greased, the flannel is well soaked in thin plaster cream, and laid on a table while the creases are smoothed out of it.
When ready it is applied accurately to the limb, so as to fit everywhere, but leaving a narrow open space along the whole length of the limb. The flannel must be held steadily till the plaster is set, which takes place in about five minutes, and the splint is complete. If one layer is not stiff enough, a second may be laid over the first in the same way. When the splints are fitted, they are kept in place by a roller applied lightly over them. If instead of soaking the second layer of flannel in plaster, it be thickly spread with strong solution of British gum (dextrine), and the gummed side laid next the first flannel, the splint is tough enough to stand any ordinary strain without breaking.
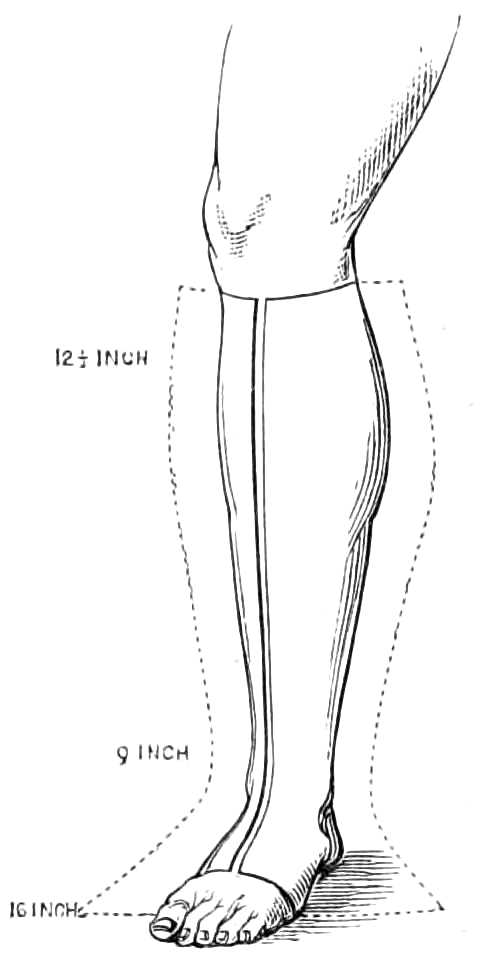
Fig. 58.—Moffitt’s method of applying plaster of Paris splints. Copied from Army Medical Reports for 1865.
Gum thickened with powdered chalk, glue, silicate of soda, Hides’ leather felt and stiffening solution, paraffine, &c., are also employed for stiffening bandages[Pg 90] and flexible splints, after they are moulded to a limb, but none of them are as readily procured or have much advantage over starch and plaster of Paris. A detailed description of the mode of using them is unnecessary.
Sand-bags are very useful, when laid along an injured limb, to prop it up on either side. For this purpose they are better than pillows, as their weight prevents their slipping from under the part they support. They should be made of macintosh cloth about 4 or 6 inches diameter, and in lengths varying from 1 to 4 feet, well closed that the sand may not escape through the seams; the macintosh should be covered with flannel, renewed from time to time. The sand should be washed and well dried before the bags are filled, that it may not rot the cloth containing it. Moreover, the bags should be only three quarters full, or they will be too hard to adapt themselves to the limb when in use.
Cradles are light arched frames of wire or cane to support the bedclothes over an injured limb. On emergency an efficient cradle can be constructed from a band-box, by knocking out the bottom and putting the leg through it. If used to protect a foot, a notch may be cut with strong scissors, not a knife, for that splits the wood.
If the cradle is stout enough, it is useful to sling a broken limb in its splint, and often great relief is thus given to the patient. Dr. Salter’s Swing Cradle is specially contrived for the purpose, and is shown, fig. 42, page 64.
Leather Splints.—For these sole leather, to be[Pg 91] purchased at any leather dealer’s, is used. In preparing them, the required length should be first noted down, then a series of transverse measurements taken at the widest and narrowest parts of the limb and over the projections of joints, &c., or a pattern may be first cut in paper and laid on the sheet of leather from which a corresponding piece is cut. The splint should always be so arranged that its edges do not bear on any bony point, the shin, or malleoli, for example, but either fall short of or pass beyond them. The hair side of the leather should go next the skin, as it is the smoothest and least irritating. The edges of the splint must be thinned by bevelling off the outside for about an inch all round, and no sharp corners should be left. When the leather is prepared it should be soaked, if the time can be spared, for twenty-four hours in cold water, but when wanted quickly it can be softened in a few minutes by soaking it in warm water to which a little vinegar is added—this, however, renders the leather brittle when dry, and apt to curl at the edges. When the leather is softened, a very thin even layer of cotton wadding or of lint is laid on next the skin; the splint is then moulded to the limb with the hands, and bandaged firmly; in twelve hours it will be dry and rigid. The roller is then unwound, and any parts of the splint pressing on bony projections are marked before removal. It is then trimmed, and laid between two layers of wash-leather stitched together round the edges. The splint is now finished, and can be either fastened on by a roller or by two or more straps and buckles stitched to it.
[Pg 92]
When support is required for a joint, the splint should be fitted on the sides, where the leather may have the rigidity of its width rather than only that of its thickness to prevent bending.
Leather Splint for the Hip.—This joint is by far the most difficult to fit. The hip splint should obtain a good grasp of its fixed point, the pelvis, and a stiff bearing on the front of the thigh where its pressure is to be exerted. There are many plans of procuring a satisfactory fit; the following is one of the best.
First cut a pattern on a sheet of paper from which to shape the leather. If possible the patient should stand while the pattern is fitting. Take a sheet of paper large enough to reach round the body, and long enough to extend from the waist to the leg below the knee. Lay it against the diseased hip, carry its vertical margin a little beyond the middle line in front towards the sound side, and the other part round the body behind, till the front is reached on the sound side. Feel for the anterior iliac spine, and mark with a pencil the point midway between it and the pubis; from this draw one horizontal line inwards to the border of the paper, and a second obliquely to the perinæum. Then seek for the junction of the sacrum and iliac bone behind, which corresponds pretty nearly to the point first found in front; from this mark the gluteal fold. Next carry a line vertically from the upper border of the sheet of paper to the great trochanter; and lastly, mark the level of the pelvis. Lay the sheet on a table and slit it with scissors along the lines marked, apply it a second time to the body and bend the thigh part round the thigh, making its[Pg 93] anterior margin reach well to the inside of the limb, while the posterior part should almost meet it from behind. The splint should also reach downwards to the back of the knee. The paper is then trimmed down to these dimensions. The hip part is next trimmed so that it clears the buttock on the sound side and passes round to the anterior iliac spine of that side. The pattern being complete, cut a piece of sole-leather to correspond, arranging that the hair or short side of the leather will lie next the skin; bevel off the outer edge all round, and soak the leather till thoroughly soft in water, wipe it dry, and bandage it carefully first to the trunk and next to the thigh. When it is set, superfluous and overlapping edges must be marked before removal; lastly, the sides of the vertical notch, between the hip and trochanter, are stitched together, and the splint is covered with wash-leather.
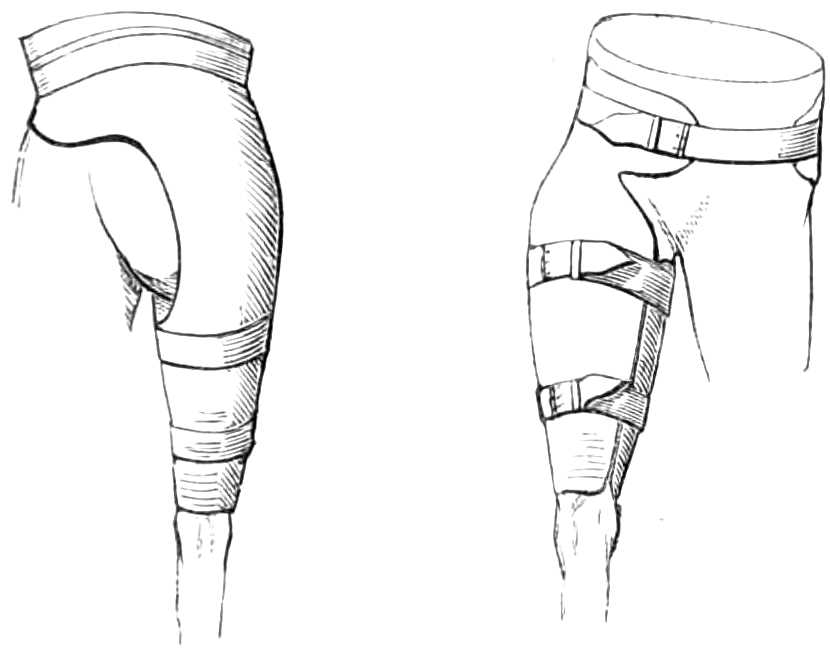
Fig. 59.—Leather splint for the hip.
[Pg 94]
When extension of the hip is required (see page 80), it can be applied to the leg below the splint without lessening the support that affords.
The accompanying figure, 59, is drawn from a splint fitted by Mr. Heather Bigg on the plan just described.
Gutta-Percha may always be substituted for leather in these splints, and the same plan of fitting is used, except that the notching requisite in leather is not necessary in using gutta-percha; for the directions to use this material see page 50.
[Pg 95]
The main obstacles in reducing dislocations are entanglement together of the displaced bones and contraction of the muscles; the entanglement of the bones determines the direction in which extension must be made, and also of the counter extension, or point at which the body is fixed to resist the traction practised on the limb; this should be exactly opposite the direction in which the limb will be drawn. The muscles can always be relaxed by chloroform, hence it is better when they are powerful, not to use the limb as a lever to prize the head of the bone into its place. Steady extension instead is better, to disengage the bone from the parts against which it is caught, and to bring it opposite its socket, into which the hands of the surgeon guide it with less risk of laceration of the soft parts than attends forcible leverage.
Lower Jaw.—This bone is dislocated on one or both sides; when the condyle has slipped forward from the glenoid fossa, the contracted temporal muscle keeps the bone from regaining its proper position, and causes the coronoid process to hitch against the malar bone.
[Pg 96]
Treatment.—Apparatus.—1. A towel.
2. A four-tail bandage.
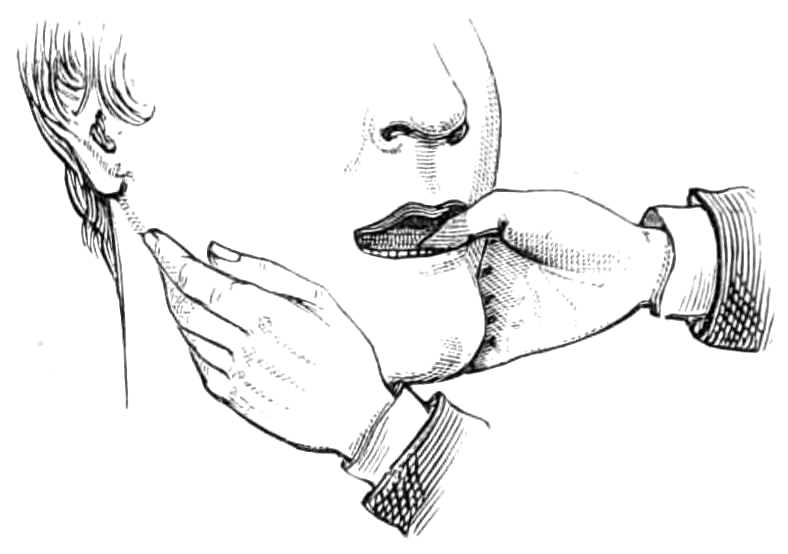
Fig. 60.—Dislocation of the jaw.
The patient should be seated in a high-backed chair, resting his head against the back. The surgeon winds the towel round both thumbs, and standing immediately in front of his patient, places a thumb on the second molar of both sides, if the dislocation be double, or on one side only, if that be alone displaced (see fig. 60). He then presses steadily downwards until the condyle is released, when it slips back to its place. The return of the bone may be aided by pushing up the chin with the fingers after the ramus of the jaw has been lowered.
When the jaw is replaced, a four-tail bandage or split handkerchief should be tied over the nucha and vertex of the head, to keep the jaw closed (see fig. 23, page 32). Biting or chewing should not be attempted for ten days or a fortnight. The patient should be warned also that when the jaw has been once dislocated it very readily slips out of place again; he must thenceforth avoid gaping or opening the jaw very widely.
The Clavicle is rarely dislocated, nevertheless both the inner and the outer end may be displaced. The[Pg 97] signs are obvious—the end of the bone is felt in its new position. The treatment for all is the same.
Apparatus.—1. Roller, 2¼ inches wide.
2. A piece of old blanket.
The blanket should be torn into strips about a foot square, and folded thrice, thus making a long soft pad to line the axilla, one for each armpit. The patient is next seated on a stool; an assistant standing behind, draws back the shoulder while he presses on the spine with his knee; the dislocation being reduced, the surgeon fixes the bone by a figure of 8 carried round the shoulders and across the back. The forearm is then bent and fastened to the body by a few turns of the roller round it and the chest. This prevents the pectorals from acting on the bone. The apparatus may be laid aside at the end of a week, but the arm must be fixed to the trunk for a fortnight longer.
This bone is often difficult to keep in place after dislocation, and even the most accurately fitted apparatus sometimes fails to effect its object, hence many varieties of collar and yoke have been devised by different surgeons to accomplish this purpose.
The Shoulder is dislocated in three directions, downwards, inwards, and backwards. These have subordinate varieties, but the signs depend chiefly on the direction of the greatest displacement.
Signs of dislocation into the axilla. When the bone is displaced below the glenoid fossa the acromion is prominent; underneath it, the surgeon feels a hollow instead of the head of the humerus, which the finger detects in the axilla. Movement of the shoulder is very limited and painful If the elbow is rotated[Pg 98] while the finger is in the armpit, the head will be found to move with the rest of the bone.
If the head of the bone is carried more inwards on to the ribs, it can be seen and felt near the clavicle; the hollow is again readily detected below the acromion, while the axis of the arm is altered, being directed inside its proper position.
When the bone is carried backwards the head is plainly felt on the scapula below the spine.
For the reduction of these dislocations several plans are employed. When recent the two first displacements can generally be restored without chloroform, but if the patient is muscular it often saves time and pain to produce anesthesia before attempting to replace the bone.
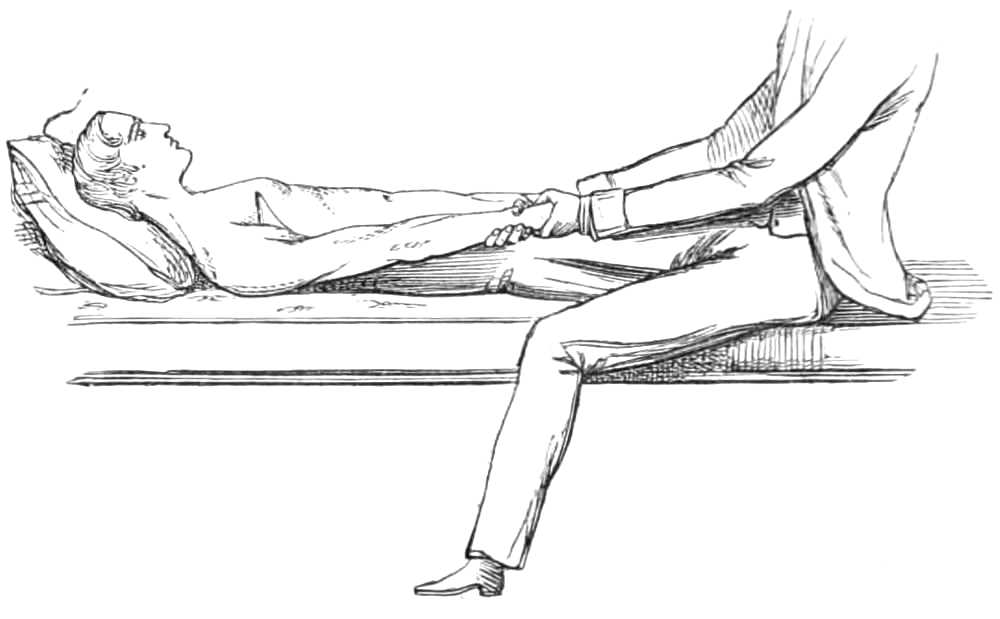
Fig. 61.—Reducing a dislocated shoulder by the heel in the armpit.
By the heel in the axilla (fig. 61).—The patient lies flat on a couch; the surgeon pulling off his boot from the left foot if he has to reduce a left dislocation, and[Pg 99] vice versâ the right boot, seats himself on the couch facing the patient. Putting his unbooted foot into the armpit, he grasps the forearm with both hands and pulls steadily downwards. When the head of the bone is disengaged the muscles draw it into the socket, and the movements of the limb become at once easy and natural. The arm must then be fixed to the side by a roller for a fortnight, and the shoulder is wetted with an evaporating lotion to allay the pain and inflammation resulting from the laceration of the soft parts. Should the surgeon’s strength be insufficient for the requisite extension, a jack towel may be attached in a clove hitch round the wrist and held by an assistant, who standing behind the surgeon draws steadily in the same direction.
To make a clove hitch.—Grasp the towel in the left hand, the little finger being downwards, then pronating the right hand till the little finger is upmost, seize the towel below the left hand; if the wrists are then rotated in opposite directions the towel will be drawn into two loops, of which the ends cross above the connecting part between the loops (see fig. 62); if one hand holds the loops and the other pulls the ends, the loops will be found not to slip, however tight the ends are pulled.
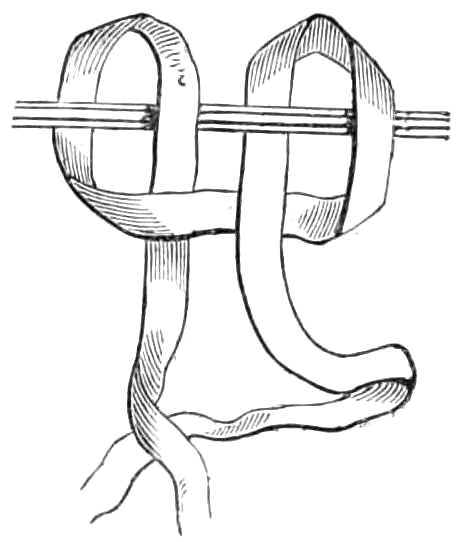
Fig. 62.—The Clove-hitch knot.
Reduction by simple extension.—The patient again lies flat on his back, a jack towel is passed round his[Pg 100] body and fastened behind the opposite shoulder for counter-extension, while a second towel is attached to the wrist by a clove hitch and intrusted to two or three assistants, who are desired to pull quietly and steadily directly away from the patient’s body. The surgeon meanwhile watches the progress of the extension, altering its direction as he finds the head more or less engaged against the scapula, and finally with his hands thrusts the head into its socket. Sometimes there is much difficulty in getting the head back to the glenoid fossa, even when the humerus is completely disengaged from the scapula; this difficulty is often overcome if an assistant rotates the humerus backwards and forwards, while the extension at the wrist and the pressure on the head of the humerus is[Pg 101] steadily maintained. When the limb is replaced it is fixed to the side as before directed.
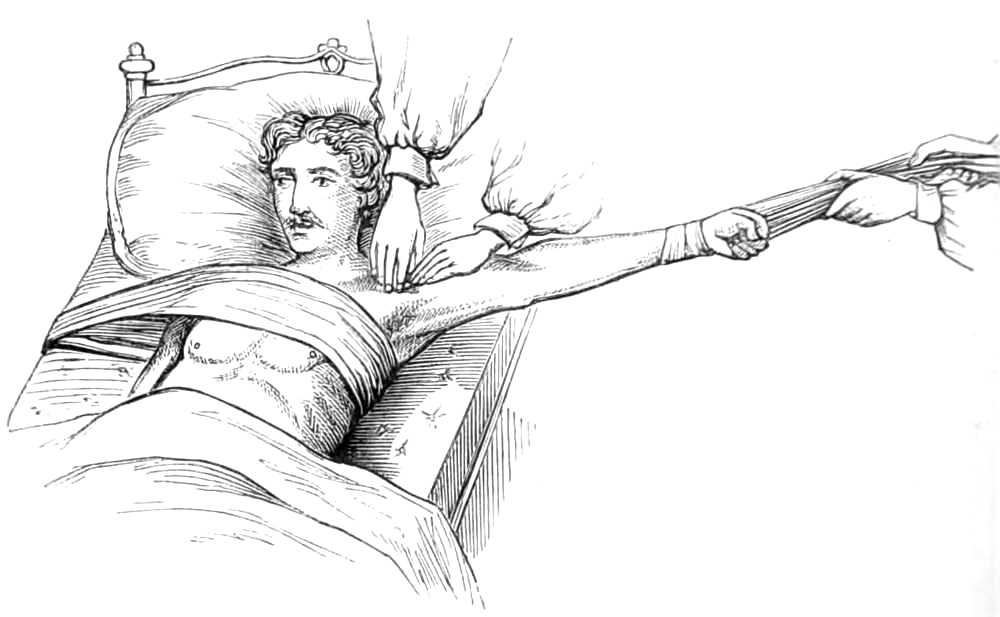
Fig. 63.—Dislocation of the shoulder reduced by simple extension.
If the dislocation has existed more than a few hours, relaxation of the muscles by chloroform and extension of the limb carried directly away from the body are more sure of success than the heel in the axilla, because they allow greater power to be exerted in a steadier manner than is possible by the other mode.
The Elbow.—The signs of dislocation at this joint are tolerably evident, but there is often coexistent fracture of the coronoid or olecranon processes. Separation of the articulating surfaces of the humerus from the shaft is sometimes mistaken for dislocation of the forearm backwards.
In dislocation of both bones backwards the olecranon is very plainly felt behind the lower end of the humerus; the sigmoid notch is generally to be made out, and the forearm is fixed at a right angle. The altered relation of the olecranon to the condyles suffices to distinguish dislocation from fracture of the humerus at its lower end, where the olecranon also goes backwards, but the condyles go with it. The immobility of the joint distinguishes it from separation of the lower articular surfaces of the humerus from the shaft, an accident, moreover, only met with in children.
Other subordinate distinctions between dislocation and fracture are, the limited movement, the difficulty of restoring the bones to their natural position, and the absence of crepitus; lastly, the peculiar form of the articular surfaces can sometimes be made out.
In reducing the backward dislocations the patient[Pg 102] sits on a chair on which the surgeon rests his foot, pressing his knee against the forearm at the elbow for a fulcrum; then, grasping the wrist with one hand, and steadying the arm with the other, he flexes the elbow to dislodge the coronoid process from the fossa at the back of the humerus; when this is done, the articulating surfaces slip into place. This plan is commonly adopted when the olecranon is displaced, but if it fails to reduce the dislocation, direct extension at the wrist must be employed, as for the following dislocation.
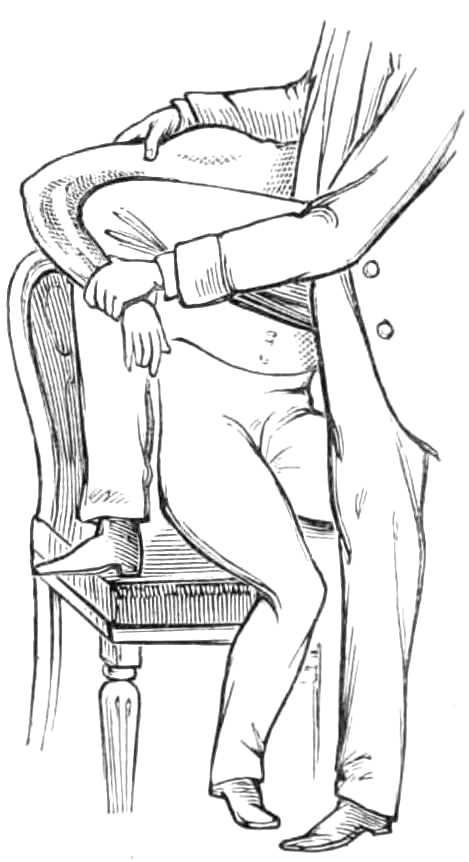
Fig. 64.—Reducing dislocation of the elbow round the knee.
When the radius only is displaced, the body should be fixed by a jack towel carried under the armpit of the injured side, and over the shoulder of the sound side. A wetted bandage is rolled round the forearm, and a second towel is attached by a clove-hitch (see fig. 62, page 99) to the wrist for extension, which is made in the axis of the limb until the radius can be slipped into its place on the outer condyle.
In all dislocations of the elbow, when the bones are returned the limb should be bent to a right angle and put on a lateral angular splint for a week or ten days, after which time it should be worn in a sling a fortnight longer.
[Pg 103]
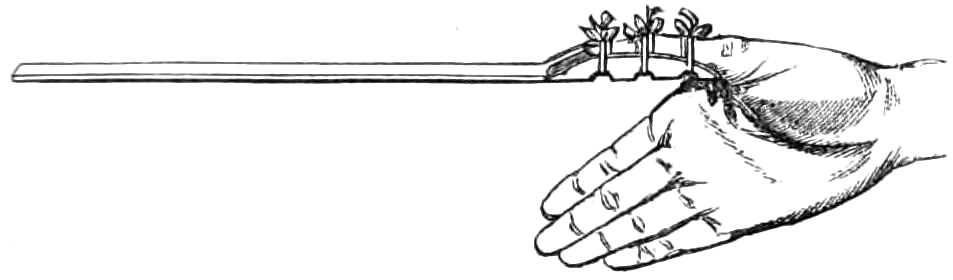
Fig. 65.—Handle for obtaining grasp of the thumb in dislocation.
The Thumb and Fingers.—When the first phalanx is dislocated from the head of the metacarpal bone it is sometimes very difficult of reduction. The most effectual mode is steady extension, which is procured by fastening the thumb to a piece of wood, which serves as a handle to give command of the phalanx, and is contrived as follows: the thumb is first bandaged with a narrow wetted roller over the two phalanges, and a thick layer of cotton wool is rolled round it; a piece of stiff wood, 1 inch wide, ½ inch thick, and 12 long, is perforated at one end with three pairs of holes ½ inch distant from each other and from the end; through these, three stout tapes, ½ inch wide and 2 feet long, are threaded, leaving three loops on one side of the piece of wood (fig. 65). The wood is then applied to the palmar aspect of the phalanges, the loops passed over the thumb, their ends drawn tight, and tied, not in a bow as the figure represents, but wound round the end of the stick. The stick thus attached becomes a good handle for extending the digit, and also a long lever for altering the direction of the phalanx if desired. Langenbeck of Berlin employs a pair of forceps to seize the thumb, instead of the wooden handle just described. But with the greatest[Pg 104] care and perseverance it is sometimes impossible to replace the bone unless the constricting bands be divided with a tenotome.
Hip-joint.—There are three chief directions in which the hip is dislocated. First backwards on the dorsum ilii, or further on to the sciatic notch. In this dislocation the limb is shortened, moved with difficulty, drawn inwards over the other, and its great toe touches some part of the back of the other foot. The hip itself is altered, the great trochanter being nearer to the crista ilii, and more prominent than on the uninjured side, and the head is often plainly felt in its new position. Resistance to extension of the limb, limited movement of the hip, with rotation inwards, are the distinguishing points between this dislocation and fracture at the neck of the femur.
Treatment.—Apparatus.—A complete apparatus for this purpose is contrived and sold by instrument makers, but a sufficiently serviceable one can be extemporised when the former is not at hand; it consists of:—
1. A rope running in two pulley blocks.
2. Three jack towels.
3. Two stout hooks to screw into the wall, or some firm object, to obtain fixed attachment.
4. A wetted roller 3 inches wide.
The complete apparatus is as follows:—
Apparatus.—1. A set of multiplying pulleys.
2. A leathern padded girth, 2 inches wide and 3 feet long, having at each end an iron ring.
3. A stout leathern belt about 6 inches broad, furnished with buckles, straps, and rings to fasten[Pg 105] on to the thigh above the knee; a rope is run through the rings to connect the hook of the pulleys with the thigh.
4. Two strong iron hooks to screw into the wall, for fixing the apparatus.
5. Half-a-dozen yards of stout cord.
6. A hook, fitted with a buckle and strap, and hinged so that, by turning a pin, it at once disengages itself. If this is interposed between the pulleys and the hook fixed in the wall, the limb may be instantaneously released if desired.
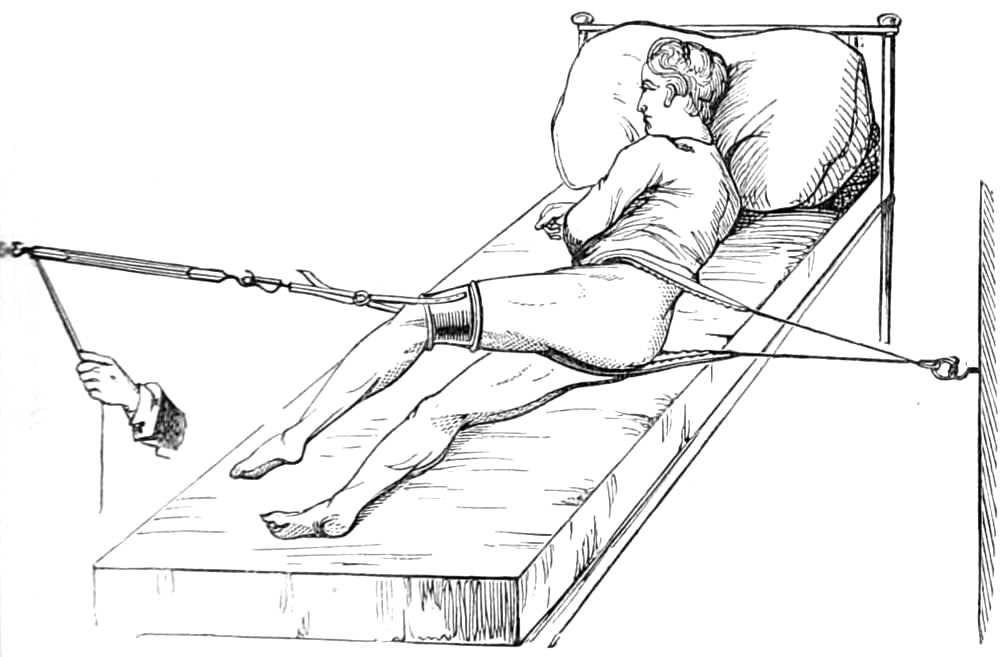
Fig. 66.—Dislocation of the dorsum ilii.
Treatment.—Step 1. The patient is laid on a flat couch, and put under the influence of chloroform. When he is narcotised, a jack towel, or if it be at hand the pelvic girdle, is carried across the perinæum,[Pg 106] arranging it to bear on the tuber ischii behind and the pubes in front, its ends being attached to one of the hooks screwed into the wall behind, and about six inches below the level of the patient. This towel should be put slightly on the stretch, that the pelvis may be kept in the position first assigned to it when the pulleys begin to draw. A wet roller is put on the lower third of the thigh, the jack towel slipped up the leg to the bandage, and fastened in a clove hitch. Another jack towel is then doubled and passed up the limb to the perinæum. The patient is next turned on to his sound side, and the belt of the thigh connected by the disengaging hook to the pulleys, which are drawn out from each other as far as their cord will allow, and attached to a hook fixed a little above the level of the patient, on a line carried from the hip across the junction of the middle and lower thirds of the uninjured thigh (see fig. 66).
Step 2. The surgeon being ready, an assistant draws on the pulley cord, getting gradual extension of the limb as required by the surgeon, who, keeping his hands on the hip and great trochanter, watches the progress of the head of the bone towards the acetabulum.
Step 3. When the bone has reached the edge of the acetabulum, a second assistant slips the doubled jack-towel over his shoulders, and by raising his body, lifts the femur away from the brim of the acetabulum, while the surgeon, grasping the foot and knee, makes a few movements of rotation backwards and forwards to ease the head into its socket.
When a reduction is effected, the limb should be put[Pg 107] in a long splint or starch bandage for three weeks, and the patient not allowed to exercise the limb freely or violently for a month afterwards.
Reduction by Manipulation.—When the patient is not very muscular, and the dislocation recent, the bone can often be speedily returned by movements of flexion and rotation.
The patient is put fully under chloroform and brought to the foot of the bed; the surgeon grasps the ankle in one hand, and the knee in the other, bending that joint till the heel reaches the thigh; he next flexes the thigh on the abdomen, in doing this he carries the knee outwards away from the body, and then rotates the limb by pushing the foot outwards, on which the head often slips into the acetabulum. If this plan do not quickly succeed it is better to have recourse to extension, by assistants if pulleys are not at hand, but the irregularity of the force when assistants are employed renders the traction of pulleys much preferable to manual strength.
Dislocation downwards into the ischiatic foramen. The limb is lengthened, capable of little motion; the knee is bent; the toe points forwards, and away from the other foot. Here the reduction is best managed by extension; the apparatus required being the same as that employed in dislocation backwards, but it is differently arranged.
Step 1. The patient lies on his back, the pelvic girth, or towel, is carried round the pelvis and fastened to the wall on a level with his body, opposite the uninjured side. A jack towel is put round the upper part of the dislocated thigh, and attached to the pulleys[Pg 108] outside, which are fastened to the wall opposite (see fig. 67).
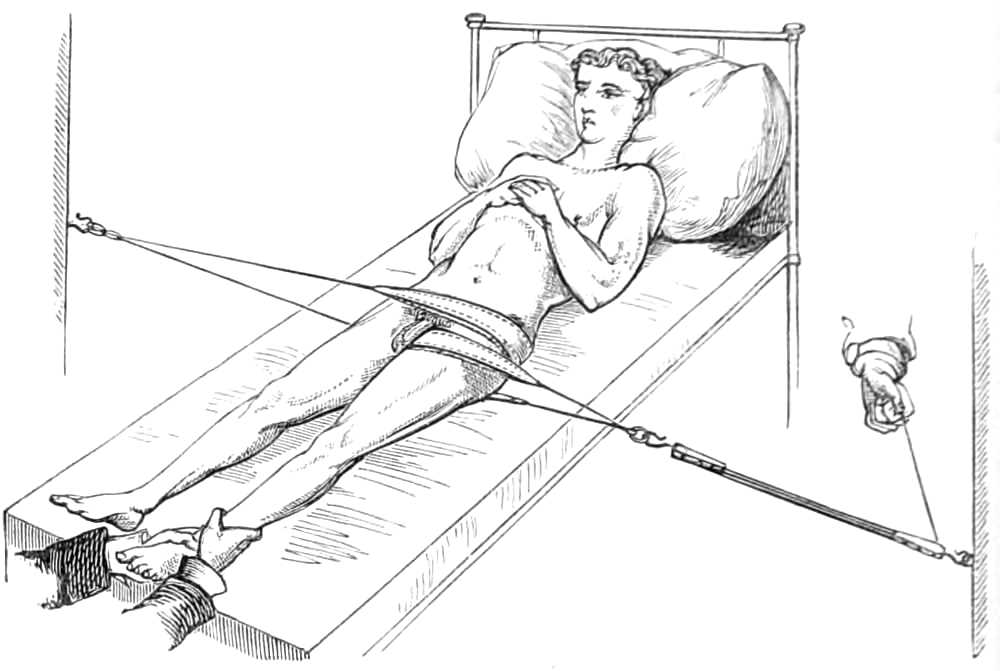
Fig. 67.—Dislocation into the foramen ovale.
Step 2. Extension is then made by an assistant, the surgeon grasps the leg above the ankle, and rotating the limb inwards and outwards, but without lifting it from the bed, guides the head into the acetabulum.
Here, as after dislocation backwards, a long splint should be worn on the limb for three weeks before the patient is allowed to move about at all.
Dislocation on to the Pubes.—The limb is easily moved at the hip, shortened, rotated outwards, and the head of the bone is felt in the groin.
The same apparatus is used in this as in the dislocation on the dorsum ilii. It is applied as follows:—
Step 1. The patient lies on his back (fig. 68), with[Pg 109] his legs separated. The pelvic band is passed over the perinæum and pubes, and attached above the patient, in a line passing from the pelvis a little to his sound side. A double jack towel is slipped up the limb to the perinæum; the pulleys are fastened to the thigh above the knee and fixed, in the manner directed on page 106, to the wall below and external to the injured side of the body.
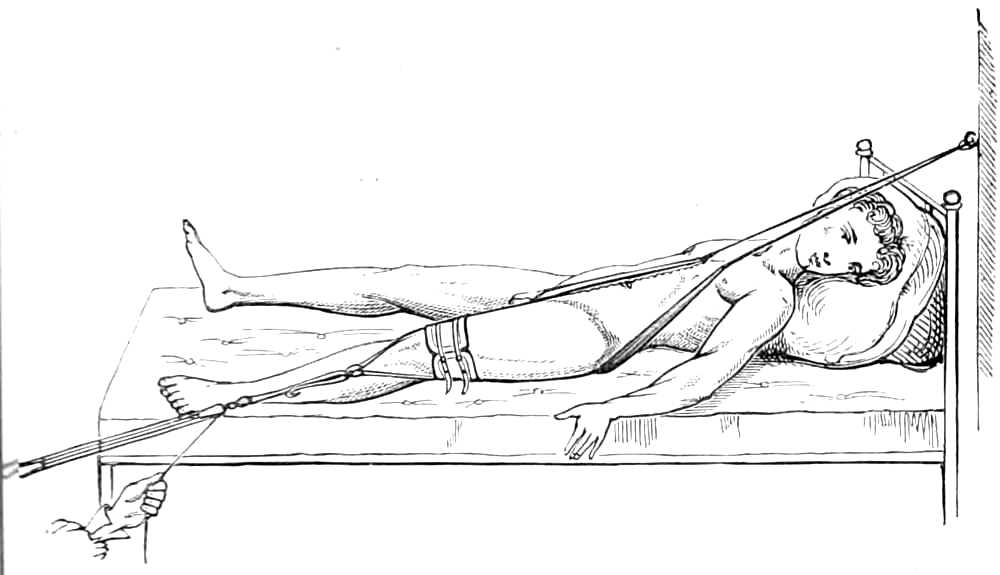
Fig. 68.—Dislocation on to the pubes.
Step 2. Extension is then steadily made, while the surgeon watches the head getting free from the pubes, over the edge of which a second assistant slipping his neck through the doubled towel, raises the bone a little outwards. The surgeon in the meantime encourages the bone by rotation to enter the socket.
A splint is necessary here also after reduction.
The Knee.—These dislocations are rarely complete, and are easily reduced; the lateral ones by flexing the[Pg 110] thigh on the belly, straightening the leg, and rotating it a little from side to side.
Another Plan.—Apparatus.—Two jack towels. This is more useful when the tibia is carried backwards. Lay the patient on his back, and slip a jack towel in a clove hitch up the leg to the ham, and another round the small of the leg; the thigh is bent and retained in a semiflexed position by an assistant holding the jack towel at the ham, while a second pulls on the one at the ankle and so disengages the bones from each other, when the surgeon readily slips them into place.
After reduction is accomplished, the limb should be fixed in a leathern back splint until the inflammation subsides.
Dislocation of the Patella.—The displacement of this bone on to the outer or inner condyle is generally easily reduced if the knee is straightened and the vasti relaxed by bending the thigh on the belly. When the patella is turned on its own axis, the side, not the under surface, is locked against the condyle, and reduction is sometimes extremely difficult or impossible. The same movements must be adopted as for simple lateral displacement, and the surgeon must endeavour to release the bone by pressing its upper edge downwards with his thumbs.
After their reduction, all dislocations about the knee-joint must be treated by rest, straight splints, and evaporating lotions.
The Foot is very rarely dislocated from the leg without fracture of the malleoli. Its reduction requires simple extension of the foot on the leg, with the[Pg 111] knee bent; the surgeon grasps the heel in one hand, the foot in the other, while an assistant fixes the thigh in the half-bent position. The foot is first drawn downwards to disengage it from the tibia, and then directed into its place.
After reduction the limb should be put in a McIntyre’s splint, in the way described for fracture of the tibia near the ankle-joint.
Scarpa’s Shoes are instruments for restoring deformed feet to their natural shape. The shoe (fig. 69) consists of a flat metal sole broader and longer than the foot, furnished with a rest for the heel. A rod, attached to the side of the sole beneath the ankle, reaches up the limb, to which it is secured by one broad band and buckle below, and by a second above the knee, opposite which joint the iron stem moves on a free joint backwards and forwards. Opposite the malleoli are set the centres of movement required for the restoration of the deformity; they are moved by a key. The foot is fastened to the sole by straps across the instep and ankle; the toes are restrained by a strap passing round them and fixed to a horizontal toe-bar by the side of the foot. In fitting one of these shoes, which of course must always be made specially for the limb it is to control, the points to be attended to are—1st, the centres of the joints must be so arranged that, when traction is made, the foot shall revolve back again round the same centres it has passed in reaching its distortion. For example, if the heel is raised, as in talipes equinus, the fore part of the sole of the shoe must be capable of elevation, by moving a joint that rotates in a plane parallel to[Pg 112] the rotation of the astragalus on the tibia. In most cases of talipes, the bones of the foot have been displaced round several centres; hence, the apparatus must be furnished with power of traction along all of these, or along the lines resulting from these different directions acting simultaneously. 2nd. The heel must be got thoroughly into its place at the back of the sole to ensure that the foot will follow the shoe in all its movements.
The treatment of talipes frequently requires division of tendons before extension is attempted, if they are too firmly contracted to permit the bones to regain their proper position until they are lengthened by division. Thus, in varus, the tibiales and tendo achillis; in valgus, the peronci; in equinus, the tendo achillis; are often divided.
The limb must not be very tightly braced into the shoe, slight tension, if continuous, suffices to overcome the resistance; and in children if the straps are drawn tight the skin almost invariably inflames, and even sloughs where it is compressed. Before the instrument is applied, the limb should be bandaged with a soft cotton, or Domett’s flannel roller. The foot is first fixed to the sole or shoe, and then the leg to the rod. Traction is increased gradually with frequent small alterations, as the foot yields to the tension and regains its natural position. The accompanying figure (No. 69) represents an instrument made by Mr. Heather Bigg. It shows the shoe restoring a much elevated heel to its proper position after division of the tendo achillis.
There are three common varieties of talipes—equinus,[Pg 113] or horse-heel, where the heel is drawn up and the toes only touch the ground; varus, club-foot proper, where the foot is twisted inwards; and valgus, splay-foot, in which the foot is drawn outwards. Equinus is often associated with varus, and sometimes also with valgus, and consequently for such cases the instrument must provide the mechanism proper to each direction of displacement.
In Equinus the heel is raised by the extreme extension of the ankle, and the sole of the foot is shortened by the metatarsus being drawn backwards. In this kind of deformity the shoe must have a joint to bring the astragalus forwards on the tibia, and the sole of the shoe must be well padded beneath the scaphoid and metatarsal bones, that, as the foot is released from its position of extreme extension at the ankle-joint, the anterior parts of the foot may be thrust upwards into their proper relation to the astragalus and os calcis.
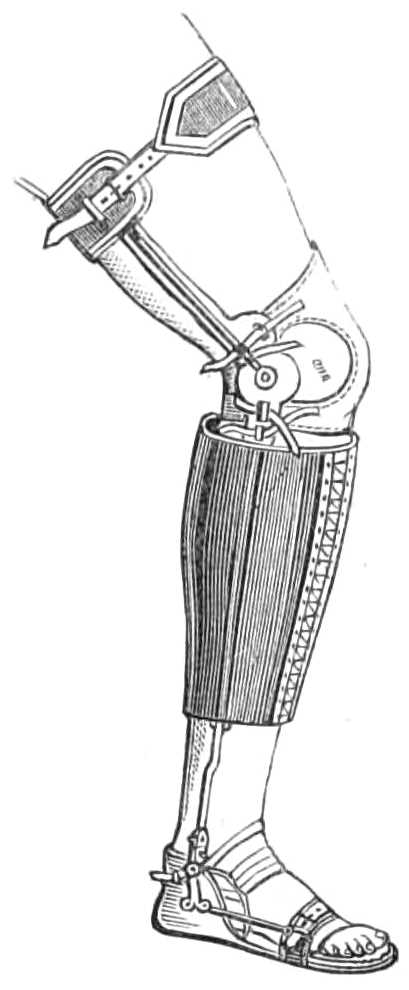
Fig. 69—Shoe for reducing talipes equinus.
In Varus, or rather Equino-varus, for varus without elevation of the heel is rare, the displacement is compound, the ankle is extended, the heel raised, the scaphoid and metatarsus are drawn inwards and downwards,[Pg 114] so that the scaphoid lies immediately beneath, sometimes even in contact with the internal malleolus. The astragalus and cuboid are drawn forwards so as to lie in front of their natural position against the tibia and os calcis. To bring down the heel the upright stem passes outside the limb, the toe of the shoe can be raised by a circular joint on the stem opposite the malleolus, which by its revolution raises the toes and depresses the heel. A second joint working outwards and upwards elevates the outer border of the foot, and restores the scaphoid to the front of the head of the astragalus. Lastly, the metatarsus is drawn outwards by a horizontal spring toe-bar along the outer border of the foot, to which the toes are fastened.
In Valgus, the plantar arch is flattened or even rendered convex downwards by the sinking of the scaphoid, and in extreme cases, by rotation outwards and upwards of the tarsus. The shoe here has the vertical rod inside the limb, and if necessary, an axis for rotation below the inner malleolus, and an elastic arched pad under the scaphoid to lift it into its natural position.
Casting in Plaster of Paris.—It is often convenient, when ordering an apparatus for deformity, to send the instrument-maker a cast of the deformed part. This is readily made in the following way:—
Apparatus.—1. Two packets of freshly burned plaster of Paris.
2. Some pasteboard, an old bandbox, or several newspapers.
3. Olive oil.
4. A basin of cold water.
[Pg 115]
Step 1. The part to be modelled should be laid in an easy position, thoroughly oiled, and a shell or trough of pasteboard roughly built round it to contain the plaster till it sets.
Step 2. The plaster is then prepared by shaking the powder into cold water, till a thick cream without lumps is formed; this is secured by constantly stirring the water as the plaster is shaken in. The cream is then poured into the trough, little by little, that it may make its way into the inequalities and recesses under the limb, until the limb is half immersed, leaving the projecting parts, such as joints, half exposed, so that the halves of the mould may separate opposite them. This first instalment is then allowed to set, and a fresh supply of plaster is prepared.
Step 3. The surface of the hardened mould is oiled, that the fresh cream may not stick to it, and the whole of the limb is then covered by pouring the cream on a second time. Plenty of plaster should be laid over the projecting parts that the mould may be strong enough for use. It should be ¾ inch thick everywhere, and 1 inch thick along the sides. When the second half is set, the trough or shell is cleared away, and the two halves of the mould removed from the limb separately.
For casting, the mould is well oiled inside and filled with cream, which sets into the cast required. While the plaster is liquid, the mould should be well shaken, that the air-bubbles may be all driven from the surface of the cast.
[Pg 116]
Hair Suture.—This is useful to bring the margins of small scalp wounds together, where plasters are not employed. It consists in taking a lock of hair ½ or ¾ of an inch on each side of the wound, and tying them together over a double thickness of lint; by this means the margins of the wound are kept together, and the dressing in place. The slits left after the removal of small sebaceous tumours are very conveniently treated in this way.
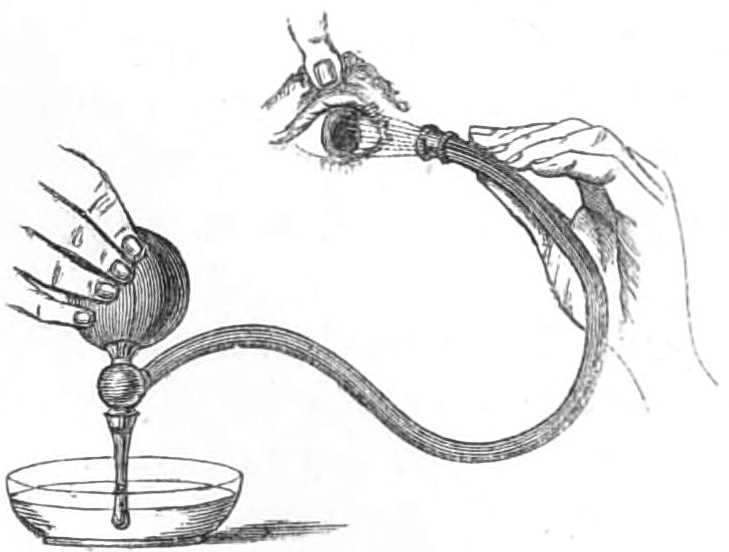
Fig 70.—Eye Douche.
The Eye Douche is a small elastic bottle fitted with a nozzle and flexible tube, ending in a rose, through which, by means of a valve, the water is drawn from a vessel and driven in a fine spray over the eye held[Pg 117] open to receive it (see fig. 70). The syringe in fig. 70 is very useful for a variety of purposes.
Eye-Drops.—Little bottles are sold by chemists for this purpose, with a tubular stopper; at one end of the stopper is a fine jet, the other is closed by a piece of indian rubber stretched over it; on pressing this a drop escapes from the jet. In dropping astringents into the eye the patient should put his head well back; while the surgeon raises one lid from the eye, drops in the lotion, and then raises the other and drops it in again, and tells the patient to move his eyelids about a little to force the lotion over the whole conjunctiva.

Fig. 71.—Syringe for sending a continuous current into the nose or ear, &c.
Syringing the Ears is best performed by a syringe having a long nozzle to direct the current of soap and water down the meatus on to the wax.[Pg 118] Figure 71 consists of a syringe with double opening and air chamber; when in action it supplies a continuous gentle current, which breaks up the concretions more speedily and with less discomfort to the patient than the intermitting jet of a common syringe; but an important part of the apparatus is the long slender nozzle to direct the stream well into the meatus. The instrument-makers supply a little spout or shoot to hang under the ear, to turn off the water into a basin clear of the neck. If time permit, the patient should keep the ear charged with olive oil for a few days before syringing, that the wax may be softened. After the wax is removed, the irritation of the canal is best allayed by a little glycerine or olive oil put into the meatus, and covered by a pledget of cotton wool, large enough to fill the concha and too large to enter the passage, where it may be lost sight of.
Ice-Cold Injection.—In obstinate epistaxis the nares are sometimes plugged, but, before proceeding to this painful mode of treatment, a simpler plan should first be tried; namely, the injection of ice-cold water into the nostril along which the blood flows. The stream should be directed upwards that the water may first dislodge the clots entangled in the meatuses, and then flow over the bleeding surface. This is best done by employing a clyster or douche bottle (see fig. 71), one tube of which lies in a vessel of ice-cold water (containing solution of gallic acid or other styptic if desired, though cold water alone usually suffices), the other tube, having a long narrow nozzle, is passed up the nostril and directed upwards among the spongy bones. With this apparatus the water is injected[Pg 119] steadily for half an hour, before being abandoned as unsuccessful. The patient is kept still, sitting upright in a cool room. If these means fail to check the flow of blood, the nares may then be plugged.
Plugging the Nares.
Apparatus.—1. A flexible catheter, No. 7, or Belloc’s sound.
2. Whipcord.
3. Lint.
4. Scissors.
Step 1. Roll up a strip of lint tightly into a mass, 1 inch broad and ½ an inch thick, trim the ends away with scissors till the mass is of a size to enter a posterior naris, then tie the wedge in the middle of a yard of doubled whipcord. If blood trickle down both nostrils both must be plugged, and two such plugs must be prepared; next, make two similar rolls of lint, and tie these up with a short piece of silk or twine to prevent their unrolling.
Step 2. Pass along the interior of the catheter a yard of twine, and draw its end through the eye of the catheter a few inches, then introduce the catheter through the naris directly backwards, not upwards nor downwards, because, when the patient is upright, the floor of the nose is nearly horizontal. When the catheter has reached the pharynx, the finger, or a forceps, must be passed through the mouth to catch the string hanging from the end of the catheter and bring it out of the mouth, where it is held while the instrument is withdrawn from the nose. The step is repeated in the other nostril if required.
Step 3. Next wash out the nostrils with a few[Pg 120] syringefuls of ice-cold water, in which some tannin is suspended.
Step 4. Fasten the double string of the plug to the end of twine hanging out of the mouth (see fig. 72), and then draw out the other end through the nose; this will carry the plug to the pharynx, where the finger guides it over the soft palate and thrusts one of its ends into the naris, where the strings draw it tight. The plug for the anterior nostril is then put in place, and the strings tied tightly over it (see fig. 73). Thus the plug in front keeps the plug behind in place and vice versâ. The end of string from the posterior nares, left hanging out of the mouth, must next be tied to the string of the anterior plug to keep it out of the patient’s way, till wanted to withdraw the posterior plug, when that is to be removed. If blood run from both sides, the other nares are stopped by a repetition of this operation.

Fig. 72.—Plugging the nares. Belloc’s sound passed through the nares, and projecting at the mouth.
This apparatus is very painful, and, if borne so long as a couple of days, should always be taken out then.[Pg 121] If bleeding recur, which is very unlikely, fresh plugs must be introduced. Sometimes the posterior plugs are soaked in styptic solutions; this is bad, because the bleeding part is not at the posterior nares, and the styptics increase the soreness the plugs themselves produce.

Fig. 73.—Plugging the nares; the strings from the posterior plug tied over the anterior plug.
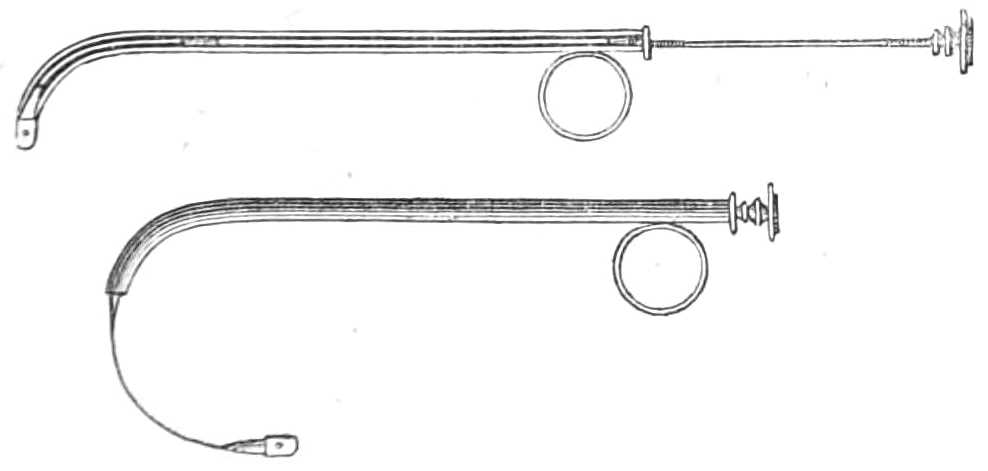
Fig. 74.—Belloc’s Sound, for drawing a thread from the mouth along the nares.
Belloc’s Sound.—Fig. 74 is a curved silver cannula like a female catheter, furnished with a long spring stylet, that arches round in a circle when thrust out of the cannula, and has a hole at the end to carry a thread. The long stylet can be unscrewed into two parts, when not in use. The figure represents the instrument with the stylet[Pg 122] ready for protrusion, and the same arching forwards after it is protruded.
The cannula is passed along the nares till the end reaches the pharynx, then the stylet is protruded and arches forward till it reaches the teeth, when a thread is passed through the hole, and the stylet being withdrawn, the thread is carried with it into the pharynx and through the nostril, where it can be used to draw the plug into its place at the posterior nares.
Tooth Drawing.—A surgeon is frequently required to draw a tooth on emergency, and should be provided with instruments (see fig. 75). Seven pairs of forceps and an elevator are sufficient for all he is likely to deal with. They are differently shaped for the different teeth, which vary much at the neck, the part grasped in the forceps.
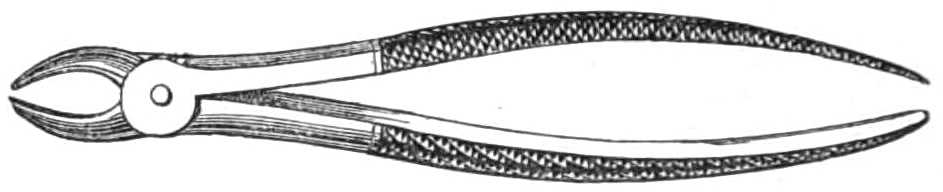
Fig. 75.—Tooth Forceps.
For the operation the patient should be seated in a high-backed chair; the surgeon stands at his right side, holds the jaw with his left hand, while with the right he thrusts the beaks of the forceps between the gum and the tooth on its lingual and buccal aspects; having reached the neck, he holds the tooth firmly, pushing it inwards and outwards with a rotary motion of the wrist (except for the molar teeth). Sudden tugs break the tooth and leave the[Pg 123] fang behind; when loosened by rotation and lateral motion, the forceps readily lift the tooth out of its socket.
For the upper incisors the beaks of the forceps are straight, slightly hollowed inside, to give them hold of the teeth, and have crescentic edges (see fig. 76).
The upper incisors and canines can be drawn by the same pair, as the shape of these teeth at the neck varies to a small extent.
For the lower incisors a very narrow forceps is necessary. The beaks (fig. 77) should be curved at the joint sufficiently to form an angle of 25° with the handles, that the latter may clear the upper jaw. The edge of the beaks is crescentic, similar to that of the upper incisors. These forceps are also very useful for removing roots, as their fineness enables them to sink between the stump and the alveolus with ease.

Fig. 76.—Upper incisor tooth and forceps.
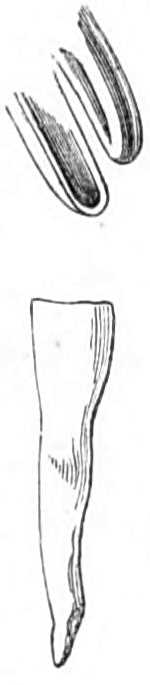
Fig. 77.—Lower central incisor and forceps.
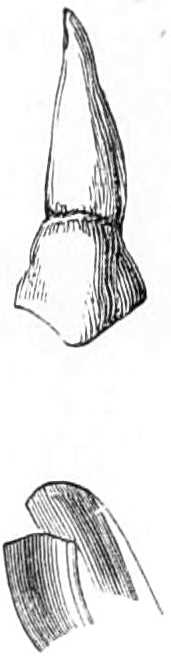
Fig. 78.—External aspect of upper bicuspid tooth, and bicuspid forceps.
[Pg 124]
For the bicuspids, beaks with crescentic edges also are used, but the inside of the beak is more hollowed to fit the round neck of these teeth (see fig. 78). All the bicuspids can be drawn with the same pair, but it is convenient to have forceps bent at the joint to clear the upper jaw when extracting a lower bicuspid (see fig. 79).
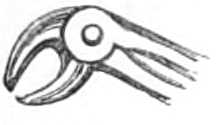
Fig. 79.—Lower bicuspid forceps.
For the upper molars two forceps are required, one for each side of the jaw; the beaks of these are well hollowed to admit the crown of the tooth. The inner beak terminates in a crescentic border to fit the large internal fang (see figs. 80 & 81); the outer beak has two smaller grooves separated by a point, that passes between the two external fangs.
In drawing these teeth the forceps should be thrust as high as possible and held firmly, while the fangs are loosened by moving the tooth from side to side, but from the multiplicity of fangs, rotary motion is not available.

Fig. 80.—Left upper molar tooth and forceps.

Fig. 81.—Right upper molar forceps.
The wisdom molars are often difficult to seize from being almost buried in the jaw; as they resemble a bicuspid in shape, bicuspid forceps (fig. 78) should be employed; if this fails to[Pg 125] penetrate between the tooth and the alveolus, the narrow incisor forceps (fig. 77) can be driven up till it grasps the tooth. Not unfrequently the fang of this tooth in the lower jaw is curved backwards and prevents extraction when the tooth has been loosened; this difficulty may be overcome by pushing the crown of the tooth a little backwards so as to tilt the fang forwards out of place.
When the molars are closely set, or the tooth to be extracted is overhung by its neighbour, it is often difficult to avoid tearing the gum extensively and even carrying away more than one tooth; tearing the gum is easily avoided by lancing it before applying the forceps, and slow and steady movements of the wrist usually prevent the latter accident, or the overhanging tooth may be filed away before the forceps are applied.
The inferior molars (fig. 82) have forceps, whose beaks are doubly grooved and pointed, to enable them to seize the neck on each side between the two fangs.

Fig. 82.—Inferior molar tooth and forceps.

Fig. 83.—Elevator.
In raising stumps, so much decayed that the forceps will not hold them, the elevator must be employed; this instrument (fig. 83), straight, pointed, and a little grooved at the point, is thrust down between the alveolus and the tooth; the jaw being then the fulcrum, the elevator[Pg 126] is the lever to push forwards the fang; when thus loosened it is easily lifted out. In working with an elevator there is some risk of thrusting the point through the alveolus, and wounding the tongue or floor of the mouth, hence it should always be guided and covered by the left forefinger. In removing the fangs of incisors the narrow forceps are most useful, and should it not be possible to penetrate between the fang and the alveolus, the alveolar border may be included in the grasp of the forceps and brought away with the tooth. The injury thus inflicted is very unimportant and much pain is saved.
After the tooth is extracted the mouth should be well washed with warm water a few times, the attending bleeding being of no importance, except in individuals of hæmorrhagic diathesis, in whom measures should be at once taken to arrest the flow.
To stop a bleeding socket the alveolus must be well cleared of clots, and fragments of sponge, soaked in a solution of perchloride of iron, one part of the salt to three of water, packed into the cavity. A plug of cork is placed between the jaws, and a four-tailed bandage (see page 32) carried round the head to keep them firmly closed. Should this plan fail, the socket must be cleared again, and the wire of the galvanic cautery pushed well down to the bottom and then heated till it has cauterised the cavity (see page 168).
Nipple Shields and Artificial Nipples made of flexible ivory, vulcanized india-rubber, &c., are required when the nipple is chafed and excoriated by the child’s sucking, especially if his mouth be attacked by thrush, as is usually the case. When the nipple is sore[Pg 127] it should be well washed and dried after suckling, covered with glycerine of starch or plastic collodion and protected by a shield. If much inflamed it may be wrapped in lint dipped in alum water or solution of sulphate of zinc (one grain to the ounce), and deep chinks should be freely rubbed with lunar caustic. The breast should be regularly emptied by the breast-pump if the child’s sucking gives much pain, lest the accumulation of milk in the ducts cause milk abscess.
Plugging the Vagina is employed in cases of rapid hæmorrhage from the womb, &c.
Apparatus.—1. A silk pocket-handkerchief.
2. A dry new fine sponge or pellets of cotton wool.
3. Silk thread.
4. A body roller or folded sheet.
The sponge should be cut into pieces the size of nuts; if the sponge is compressed it answers better. When prepared, the vagina should be cleared of coagula by a syringeful of ice-cold water; the handkerchief, unfolded and thrown over the right hand, is passed up the vagina till its centre reaches the os uteri, the borders and ends then project from the vagina. The interior of the handkerchief is next filled by firmly packing the sponge in bit by bit until the vagina is distended by the mass; the ends of the handkerchief are then tied together. The sponge swells as it absorbs the blood, and compresses the bleeding vessels by its distention.
The abdomen and uterus are then supported by a body roller, or folded sheet, wrapped tightly round the hips and waist, while the patient, lightly clad, is kept quiet in a cool chamber.
[Pg 128]
When the plug has answered its purpose it is removed, by withdrawing the sponge bit by bit, and the vagina is washed with tepid water.
The kite’s-tail plug.—Masses of cotton wool the size of a hen’s egg are tied at two inches distance from each other along a long string. When about a dozen are tied on, a speculum is introduced, and the first ball of wool is passed to the bleeding point and pushed firmly against it, and then another, and so on, until the vagina is firmly packed. An end of string is left hanging out of the vulva, whereby the plug may be removed when necessary. Each mass comes away successively with ease as the string is pulled out of the vagina.
Injecting the Urethra often fails from the inefficient mode in which it is done. The syringe employed should be short enough to be worked easily with one hand, and need not contain more than one or two tea-spoonfuls, as the capacity of the urethra does not exceed that amount. One of such a size is just 2 inches in length, and easily worked by one hand. The opening through the nozzle should also be wide, that a forcible stream may be injected into the urethra.
The patient should fill the syringe, then place on a chair or stool before him a chamber pot, and, having just made water to clear out the discharge collected in the urethra, he inserts the slightly bulbous nozzle into the meatus urinarius. He then grasps the sides of the glans with the left forefinger and thumb to close the mouth of the passage. The right forefinger next presses down the piston slowly, so that the whole of the injection passes[Pg 129] into the canal and distends it; keeping the meatus shut with his left finger and thumb, the patient lays down the syringe and rubs the under part of the penis backwards and forwards, that the injection may be forced into any folds or follicles of the mucous membrane. Having thus occupied about thirty seconds, he releases the mouth of the passage, when the fluid is ejected sharply into the vessel placed ready to receive it. This rapid ejection is a test of the proper performance of the operation.
In counselling the use of astringent solutions, the surgeon should always caution the patient not to employ one that produces severe smarting, which lasts more than a few minutes after injection. If it causes much pain, the solution is too strong.
Catheters and Bougies.—Silver catheters are made in sizes, increasing from No. ¼ to No. 12, the first having a diameter of 0·64 inch, the latter 0·25 inch. Larger ones than these are seldom employed.

Fig. 84.—Silver catheter.

Fig. 85.—English Flexible catheter.
The curve preferred by different surgeons varies much; that depicted in fig. 84 is the one used by Sir Henry Thompson; it begins at 3¼ inches from the[Pg 130] point, and ends when the point is at right angles with the stem. Each catheter is fitted with a wire stylet.
The flexible catheters are of many kinds; the English gum-elastic (fig. 85), the French black flexible (fig. 86), and the vulcanised india-rubber (fig. 87), catheters, being the three varieties most generally employed. English flexible catheters should be kept on stylets well curved at the last 3 inches, that, when the stylet is withdrawn, for the catheter to be passed, the latter may retain sufficient curve to pass over the neck of the bladder easily.

Fig. 86.—French bulbous-ended catheter.

Fig. 87.—Vulcanised india-rubber catheter.
Sounds are solid, being of steel, plated or gilt. Their curve varies, and is generally 20 or 30 degrees more obtuse than that of the catheters.
Bougies are made of the same materials as the flexible catheters; they are kept straight, and the more supple they are the better, the black bulbous-ended bougies being the most useful variety for dilating the urethra.

Fig. 88.—The Olive-headed bougie.
Olive-headed Bougies (Bougies olivaires) are used for exploring the urethra in cases of gleet, where the discharge is often kept up by a stricture or a tender patch of chronic inflammation of the mucous membrane. They are made of metal, or of black gum[Pg 131] mounted on a very flexible leaden wire; the latter kind are far preferable. The stem of the instrument is slender, no bigger than a No. 3 or No. 4 bougie; the end terminates in a conical point about ¼ or ⅜ of an inch long, expanding at its base to any required size. These bougies are most useful from No. 4 to No. 16 of the English scale, or from No. 10 to No. 24 of the millimetrical scale. The stem should be marked with white rings an inch apart, so that when the instrument is passing over a tender part, or is arrested by a stricture, the distance of the impediment down the urethra can be at once estimated. In withdrawing the instrument, the wide base of the olive shows the exact position and length of those strictures which are not too narrow for the olive-head to slip by, for it is nipped by the stricture and released as soon as the narrowing is passed. By using instruments large enough to fill the normal urethra, an induration beneath the mucous membrane can be detected in its earliest stage before it has produced symptoms diagnostic of stricture.
Rigid instruments have one advantage over flexible ones, in that their points can be guided by the surgeon; the points of flexible instruments cannot be directed, hence the introduction of the latter into a stricture is less easily managed, consequently bougies with various kinds of points should be kept. But flexible instruments cause far less irritation than rigid ones, and should always be employed instead of the latter when possible: with patience and practice much of the difficulty attending their introduction is overcome. The French bougies, with tapering ends and bulbous[Pg 132] points, slip more easily through a stricture than instruments having the same diameter throughout, and bougies with fine tapering points can sometimes be introduced where others fail.
Passing Catheters.—In passing instruments along the urethra the conformation of its interior should be borne in mind. From the meatus to the triangular ligament, the normal urethra, when gently stretched, becomes a straight tube; having, nevertheless, just within the meatus, a pouch in the roof, the lacuna magna, where the point of the instrument may catch if not turned downwards. At the bulbous part the urethra enlarges in capacity by having a slight downward curve in its floor, just before the triangular ligament is reached. In this depression, the beak of the catheter is apt to sink below the level of the passage through the ligament, which is always a fixed point. Beyond the triangular ligament the urethra curves gently upwards, has a floor beset with irregularities, in which the point of the instrument easily catches, if not raised as it passes along the curve.
A Silver Catheter is passed most easily while the patient is in a horizontal position, with the shoulders low and the thighs separated. The surgeon stands on the left side of the patient, and holds the catheter, previously warmed and lubricated with oil or lard, lightly between the thumb and two first fingers of the right hand, the beak downwards and the stem across the patient’s left groin. Then taking the penis between the middle and ring fingers of the left hand, the palm being upwards, he pushes back the foreskin with the thumb and forefinger, and steadies the meatus[Pg 133] while introducing the beak of the catheter. This done, he draws the penis gently along the catheter as the point is lowered to the perinæum, but without raising his right wrist until the instrument has travelled 5 or 6 inches along the passage and reached the triangular ligament. The surgeon then carries his right wrist to the middle line of the patient’s body, and while pushing the point onwards, raises the hand round a curve till it again sinks between the patient’s thighs. When the bladder is reached he withdraws the stylet that the urine may escape. Three points of difficulty are usual in passing catheters; the lacuna magna just within the meatus, the triangular ligament, and the prostatic part of the urethra just before the bladder is reached. The first is escaped by keeping the beak along the floor of the urethra for the first two inches; the second is best avoided by raising the wrist as the instrument passes the triangular ligament, and directing the beak against the upper surface of the urethra, lest, being in the enlarged bulbous part, it sink below the opening in the ligament; the third difficulty is overcome by depressing the hand well as the point approaches the bladder.
To pass the catheter in the upright position, the patient is placed against a wall or firm object, with his heels eight or ten inches apart and five from the wall, that he may rest easily during the operation. The surgeon sets himself opposite the patient and grasps the penis with the two middle fingers of the left hand, the palm upwards; he next exposes the meatus with the thumb and forefinger, and his right hand holding the catheter by its middle obliquely across the left side of[Pg 134] the patient, he draws the penis on to the instrument till the triangular ligament is gained. He then carries the shaft of the catheter to the middle line and, holding it by its end, brings the right hand downwards and forwards, to carry the point upwards over the obstruction at the neck of the bladder.
The operation should be done slowly and with great gentleness, giving the urethra time “to swallow the instrument,” as the French surgeons express it. Hasty or forcible movements tend to thrust the point against the wall of the urethra, where it hitches, if it does not penetrate and make a false passage. However easy the introduction may have been, the withdrawal of the catheter should be always done slowly to avoid giving pain to the patient.
When the canal suddenly contracts, as from a stricture, the point of the sound often stops at the obstruction; by withdrawing the instrument a little, and diverting its point to another side or along the upper part of the urethra, a part where the obstruction is less abrupt will often be found to let the catheter glide into the stricture. The floor of the urethra should always be avoided, as false passages nearly always branch off from the floor close to the stricture.
Difficult narrow strictures are most easily overcome by injecting a drachm of warm olive oil into the urethra, and then passing fine black gum or whalebone bougies (bougies filiformes) along the urethra. These, from their fineness (their diameter is only ⅓ or ⅔ of a millimetre, about 1/100 inch), are very apt to catch in false passages; if so, the bougie should be left engaged in the false passage, and held in the left hand[Pg 135] while another bougie is passed along the urethra; if, in its turn, this one gets into a false passage, it also should be left, and a third passed; and so on till all the false routes are occupied, or a bougie enters the stricture and reaches the bladder, which is known by the readiness with which it will pass backwards and forwards. The other bougies should then be withdrawn, and the bougie which has passed the stricture be tied in for twenty-four hours, until the passage is sufficiently dilated to allow a small catheter to replace it. If the patient is not suffering from retention of urine, there need be no anxiety about evacuating his bladder, as urine will find its way alongside the bougie when he attempts to make water. In passing to relieve retention, No. ½ English flexible catheter should be used instead of bougies; but when the stricture is too narrow for these, a bougie may still be tried, as the urine will generally dribble alongside the bougie with sufficient rapidity to relieve the patient.
English flexible Catheters should be kept on stylets curved as represented in fig. 85, that the first 3 inches of the instrument, when the stylet is withdrawn, may retain sufficient curve to ride over the impediment at the neck of the bladder. In warm weather, after being oiled, they should be dipped in cold water just before using, to render them a little stiffer, and less likely to lose their curve while traversing the urethra.
They may also be passed while the patient lies or stands, and the movements are the same as for the silver catheter.
Bulbous-ended or probe-ended Catheters and Bougies (Bougies à boule) are always straight; their suppleness,[Pg 136] their tapering ends, and their smooth rounded point enable them to glide along the urethra, and to accommodate themselves readily to the windings of the passage; for which reason they are the easiest to pass both for the patient and the surgeon. In passing them they are slightly warmed, if the weather is cold, to restore their flexibility, and gently pushed along the canal till the bladder is reached.
Vulcanised India-Rubber Catheters (fig. 87) are used when the bladder is to be kept empty; their suppleness renders them very unirritating, and as phosphates crust on them very slowly, they may be worn for a week without being changed.
They are easily passed by threading them on a stylet with the appropriate curve, and lubricating them with white of egg or water, not with grease, which injures them. The stylet is withdrawn after they are passed.
To pass a Catheter in the Female.—The patient may lie on one side or on her back; if on her side the knees should be well drawn up; if on her back, the thighs must be somewhat separated. Before introducing the catheter, a wine bottle or narrow-necked bed urinal should be placed in the bed ready to receive the urine. If the ordinary slightly curved female catheter be not at hand, a No. 7 or 8 flexible one does just as well.
Having oiled the instrument, go to the patient’s back, and take the catheter in the right hand if the patient lies on her right side, and in the left hand if she lies on her left side; if she lies on her back, go to either side and take the catheter in the hand nearest her feet. Hold the stem of the catheter in the palm,[Pg 137] so that the beak lies against the tip of the forefinger, while the thumb and second and third fingers grasp the stem. Then passing the hand under the bed-clothes, seek the buttock; from that pass the forefinger to the perinæum, and let it enter the vulva, keeping the back of the finger against the posterior part, then pass it between the nymphæ to the entry of the vagina. This is known by the tip of the forefinger being lightly grasped, unless the vagina is very wide. Keeping the finger just within the entry, feel for the arch of the pubes in front; having found this, withdraw the tip of the finger slightly from the vagina: in doing this, it will strike a small projection of mucous membrane hanging just at the anterior margin of the entry. Keep the finger steady against this, while the other hand pushes the catheter gently onwards, which then rarely fails to enter the urethral opening close above the projection of mucous membrane. Having penetrated the urethra, arrange the catheter in the receptacle for the urine, and push the instrument into the bladder.
To Wash out the Bladder.
Apparatus.—1. A flexible catheter; Nos. 8 or 9 are convenient sizes; but a smaller one can be employed.
2. A caoutchouc bottle, holding six ounces, and fitted with a tapering nozzle and stop-cock. (Fig. 89.)
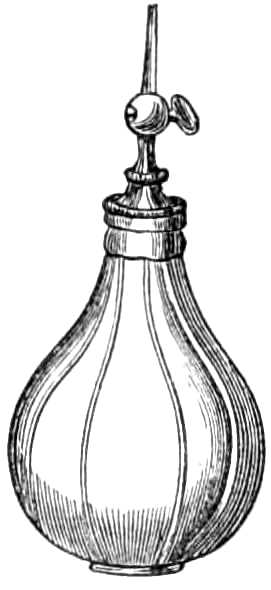
Fig. 89.—Elastic india-rubber bottle for injecting.
During the operation the patient should stand, if possible, as the mucus is thus more easily cleared from the bladder. The surgeon first[Pg 138] fills his bottle completely with tepid water, that no air may remain; then directing his patient to stand against a wall or some firm object, passes the catheter and draws off the urine. He next inserts the nozzle into the catheter, and, turning the cock, compresses the bottle slowly until two or three ounces of water have run into the bladder; this he lets escape by removing the bottle for a minute, and then repeats his operation till the water returns clear, without exhausting the patient’s strength. Three or four small injections wash the sediment and mucus from the bladder as quickly, and with far less fatigue or risk of spasm than a prolonged flow of water through a stiff double current catheter. In this way the bladder may be washed twice or thrice daily to the great comfort of the patient.
Injections of solutions of nitrate of silver, carbolic acid, alum, &c., in the proportion of 1 part to 100, or to 50 of water, can be used instead of water for this purpose.
To Tie in a Silver Catheter.
Apparatus.—1. A few yards of tape ¼ inch wide.
2. A roller.
3. A spigot of wood; or,
4. A yard and a half of fine india-rubber tubing.
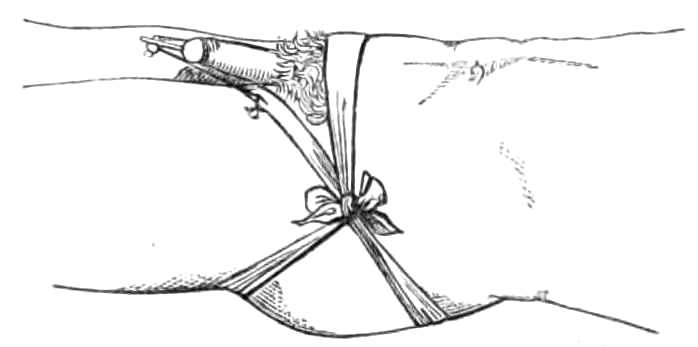
Fig. 90.—A silver catheter tied in the urethra.
A narrow roller is tied round the hips; from this, on each side, a tape is passed round the thigh at the[Pg 139] groin, and fastened before and behind to the roller round the hips (see fig. 90); a narrow tape run through the rings of the catheter connects them with the loops in the groins. The tapes are tied short enough to prevent the catheter slipping out; a yard or two of narrow india-rubber tubing, fixed on to the end of the catheter, conveys the urine to a pan under the bed, and keeps the bed dry, or a spigot of wood fitted to the catheter may be inserted, for the patient to draw out when he desires to void his urine.
To Tie in a Flexible Catheter. (Fig. 91.)
Apparatus.—1. A piece of soft twine, or Berlin wool, about 15 inches long.

Fig. 91.—A flexible catheter tied in the urethra; the string fastened behind the corona glandis, and concealed by the foreskin.
A catheter is first passed into the bladder, and the urine runs off. The catheter is then gently withdrawn, till the stream ceases, that the end of the instrument may remain just without the neck of the bladder. The string should be tied round the catheter ½ an inch from the meatus, its ends gathered together and tied in a knot about 1 inch farther on. The foreskin is then drawn back, the ends passed beneath the glans and tied round the penis behind the corona; the superfluous string is snipped off, and the foreskin brought forward. The catheter is cut off obliquely ½ an inch beyond the string and then stopped with a spigot, direction being given to the patient to withdraw the spigot, and[Pg 140] push the catheter a little further in when he wants to make water.
To Tie a Patient in Position for Lithotomy.
Apparatus.
Two bandages, each 3 yards long and 2 inches wide, of calico or saddle-girth, with tapes sewed on the ends.

Fig. 92.—Tying for lithotomy.
The patient is laid on his back, a slip-knot made in the middle of the bandage and passed over the wrist; the hand is then made to grasp the foot, the thumb above, the fingers under the sole (fig. 92); one end of the bandage is carried behind and inside the ankle to the dorsum of the foot, where it meets the other end passing in front of the ankle. The ends are then carried under the sole, brought up and tied in a double bow over the back of the hand.
Bedsores are best treated by great cleanliness, and by washing the skin exposed to the discharges with spirit of wine every day. Brown-Sequard recommends cold and heat to be applied daily, by means of an ice bag for ten minutes, followed by a warm poultice for an hour. The pressure of the skin over the sacrum or trochanters is prevented by a ring of soft thick felt,[Pg 141] covered on one side with adhesive plaster, and applied like a corn plaster around the prominent bone.
In addition to these local applications, the pressure of the body should be evenly distributed over its under surface by placing the patient on a water cushion, or, better, on Arnott’s water-bed.
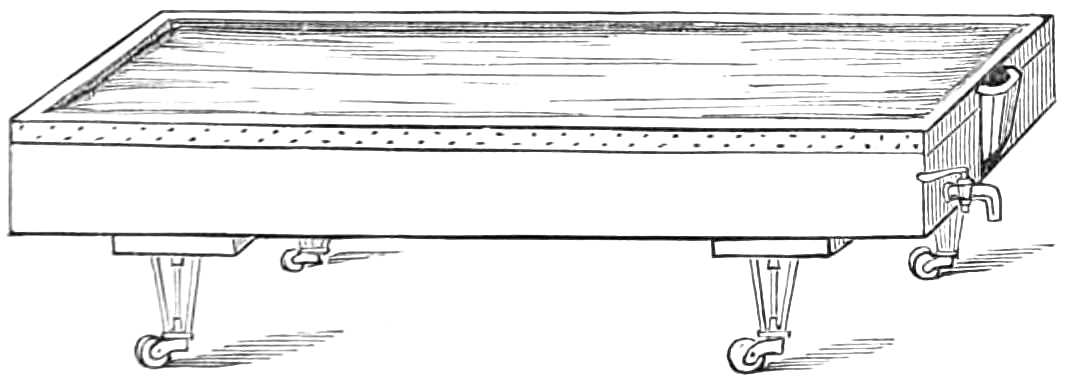
Fig. 93.—Water-bed.
Arnott’s Floating Bed.—In the hydrostatic or floating bed of Dr. Arnott, the patient floats on the surface of a trough of water, into which he sinks until he has displaced his own weight of water; his floating apparatus, or raft, so to speak, being a sheet of waterproofing, and a thin mattress or folded blanket, on which he lies. The bed consists of a trough running on large castors, about 8 feet long, 2 feet 8 inches wide, and 1 deep, with a tap at the bottom for letting out the water, and a spout in one corner to fill it by. Over the top a macintosh cloth is spread, its edges being firmly nailed to the margin of the trough, but the cloth is left slack enough to float easily on the surface of the water when the trough is partly filled. This slackness is requisite to allow the water displaced by the weight of the patient’s body to rise up around him without tightening the cloth, or the floating principle[Pg 142] of the bed is not carried out, and the pressure of the patient’s weight not evenly distributed over his body (see fig. 93). Three or four blankets are laid evenly over the macintosh, and these again protected from the moisture of the patient by a macintosh under-sheet. If a mattress is used, it must be very thin, and supple enough to let the surface of the water adjust itself to the patient’s body and receive the pressure evenly. The water employed to fill the bath should be about 50°.
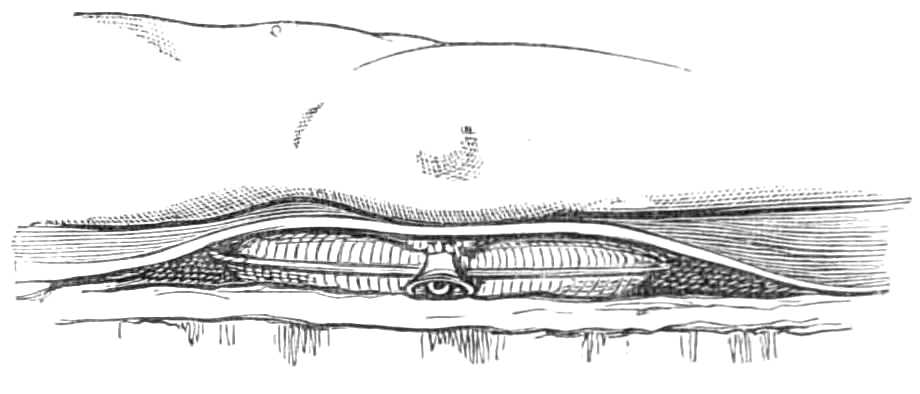
Fig. 94.—Water-cushion.
Water Cushions are flat cushions of stout macintosh cloth, half or two-thirds full of water, and laid on the mattress beneath the blanket and sheet (see fig. 94). They are more portable than the water-bed, but they are simply soft pillows, and do not counter-balance the weight of the patient in the manner of the floating bed.
The Stomach-Pump is used for emptying the stomach, or for injecting fluid food when patients refuse to swallow.
It consists of a brass syringe holding 4 ounces, of which the nozzle is connected with two tubes, one at the end, the other at the side. The passage through[Pg 143] these is directed by a valve which is governed by a lever lying on the barrel (see fig. 95). When the lever is at rest, the current passes in and out of the syringe by the lateral tube; when depressed, by the direct tube. The elastic tubes with smooth nozzles, about 2 feet long, are fitted to the syringe. There is also a gag of hard wood, having a hole in the middle, through which the tube passes on its way to the stomach, to protect it from the patient’s teeth.
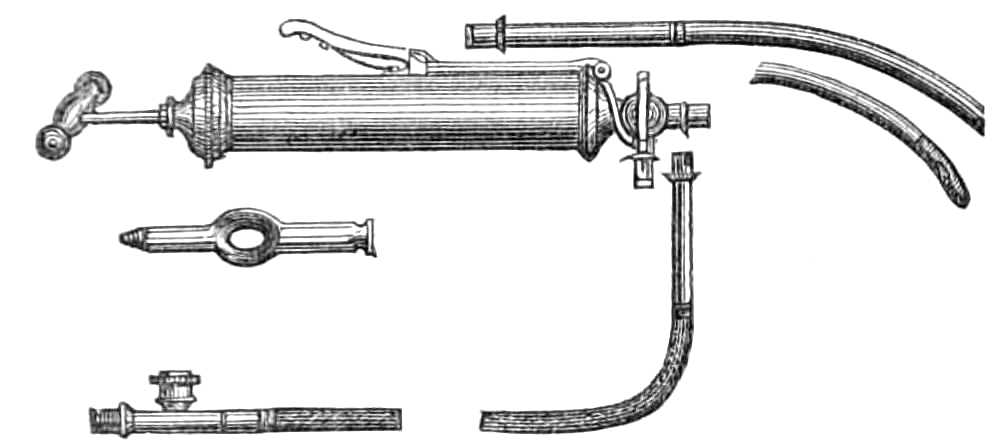
Fig. 95.—The stomach-pump.
When the pump is employed to remove the contents of the stomach, two washhand-basins are placed at hand, one empty, one full of tepid water. The patient is seated in a high-backed chair to steady his head; one assistant holds his hands, while a second screws the small end of the gag between the teeth and forces open the mouth, across which it is then easily fixed. The flexible tube, being well oiled, is next passed across the pharynx and down the gullet slowly and cautiously, without staying for any effort of vomiting it may induce; when about 20 inches are passed through the gag the nozzle has reached the stomach. First, two or three syringefuls of water are injected into the stomach;[Pg 144] then, removing the second tube from the basin of water to the empty basin, the action of the syringe is reversed, by pressing on the lever as the piston is raised, and letting it fly up when the piston is depressed. Thus two syringefuls may be withdrawn, then fresh water is again injected and withdrawn, until the contents of the stomach are removed and the water returns clear. Precaution must be always taken not to exhaust from the stomach before water is injected, lest the coats of that organ be injured by being sucked against the nozzle of the tube.
If desirable, antidotes may be dissolved or suspended in the water injected. When the pump is used for feeding patients, one or two pints of beef tea, eggs beaten with milk or wine, Liebig’s soup, &c., are the kinds of food suited for the purpose. Each time the pump is used, it should be thoroughly cleaned by syringing through it plenty of warm water, and the tubes must be unscrewed to wipe the joints carefully.
Transfusion of Blood.—The points of greatest importance in performing this operation are:—
1. That the supply of blood come from a vigorous adult.
2. That the transfer be made within two minutes of the blood’s escape from the vein of the supplier.
3. That, to prevent coagulation, the blood should pass over as small a surface, and suffer as little exposure as possible in transit.
4. Care must be taken to prevent air entering the vein with the blood.
The apparatus described below is that devised by Dr. Graily Hewitt, and depicted in the Obstetrical[Pg 145] Society’s Transactions for 1864, page 137. It consists of a glass syringe holding two ounces (fig. 96), with a piston easily attached and removed; its nozzle is curved and fits the mouth of a cannula of silver. The nozzle of the syringe is provided with a little stopper attached by a chain; a stylet likewise fills the cannula, to be withdrawn when the blood is injected through the latter.
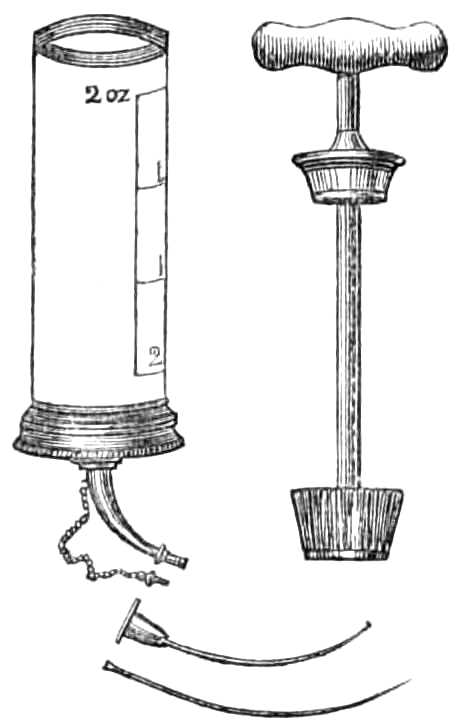
Fig. 96.—Graily Hewitt’s syringe for transfusion of blood.
The success of the operation depends in great measure on the rapidity with which it is performed, and requires the aid of two assistants that the various steps may follow each other as quickly as possible.
Apparatus.—1. Syringe, cannula and stylet.
2. Lancet.
3. Scalpel.
4. Forceps.
5. Three yards of tape, one inch wide, and lint.
6. A silver wire suture.
7. A basin of cold water.
8. Brandy and Sal Volatile.
Step 1. See that the piston-rod works properly in the syringe, and that the instrument is fit for use; then place it in the basin of cold water with the cannula to lie till wanted.
Step 2. Place the person supplying the blood on a[Pg 146] couch or easy chair in the same chamber, but so that he cannot see the recipient, lest he faint and his blood consequently flow feebly. Tie up the arm as for venesection; lay ready the lancet, and direct the assistant, in charge of the supplier of blood, to keep his thumb on the vein when it is opened, that the flow may be checked when blood is not required.
Step 3. Place a tape round the arm of the recipient, above the point for injection, and another below it at a convenient distance, and lay bare a vein (usually the median basilic) for an inch and a half of its course; holding the vein by the forceps, make a slit with the scalpel and introduce the cannula, which is then intrusted to the second assistant. The stylet is withdrawn, and a minute drop of blood escapes through the cannula, showing that the point has been properly introduced into the vein. The assistant replaces the stylet and slackens the ligature, while the surgeon proceeds to fill his syringe.
Step 4. The surgeon, going to the supplier of blood, makes a large opening in the vein with a lancet, or if the first assistant be a surgeon also, he may do this while the chief operator is preparing the vein of the recipient. When the vein is open and the blood flowing freely, the barrel of the syringe is inverted over it and filled with blood; when full, the nozzle is stopped by the plug and the piston attached while the syringe is carried to the recipient.
Step 5. This being reached, the plug is pulled out, the nozzle inserted into the cannula, and the blood slowly injected by depressing the piston gently, but without quite emptying the syringe. A minute should[Pg 147] be spent in injecting one ounce and a half, and a pause of five minutes ensue before a second supply is introduced. This interval may be employed in cleaning the syringe, &c., and procuring a fresh supply of blood; 3-4 ounces of blood are usually sufficient, but 10 ounces have been injected on some occasions. The perturbation of the supplier (generally a near friend of the recipient), renders it necessary he should drink freely of brandy and water, that the blood flow forcibly when required.
Step 6. When sufficient blood has been introduced, both patients’ wounds are dressed, as after venesection (see page 20), the long incision of the recipient being closed by a point of suture under the pad.
Tourniquets.—Tourniquets are of several kinds.
The Ring Tourniquet (fig. 97) is used when pressure is desired on the main artery of such a limb as the arm. It is less easily displaced than the Signoroni, but, like that, soon becomes irksome by its continual pressure.
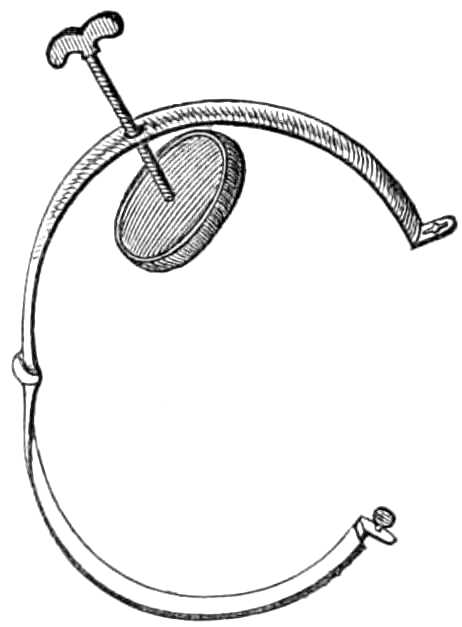
Fig. 97.—Ring tourniquet.
When hæmorrhage has to be temporarily arrested, that of Petit (fig. 98) is generally used. It consists of a strap of stout webbing and buckle, that can be rapidly tightened by a few turns of a screw. To use this tourniquet, lay a roller over the artery and carry the end once or twice round the limb to steady the roller, then pass the strap over the roller,[Pg 148] keeping the buckle about two inches away from the screw and the screw on the anterior or outer aspect of the limb, not over the pad, lest that be displaced when the screw is tightened. The tourniquet should be screwed up as quickly as possible, that the limb be not charged with blood by obstructing the venous, before the arterial flow is checked.
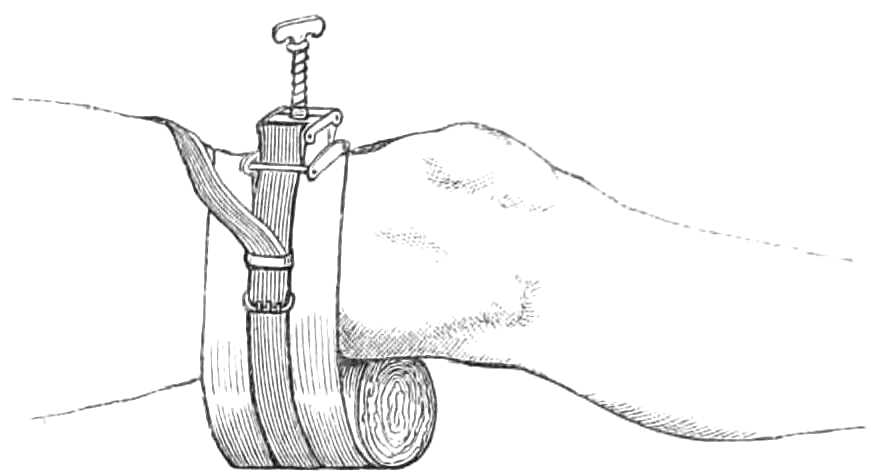
Fig. 98.—Petit’s tourniquet applied to the popliteal artery.
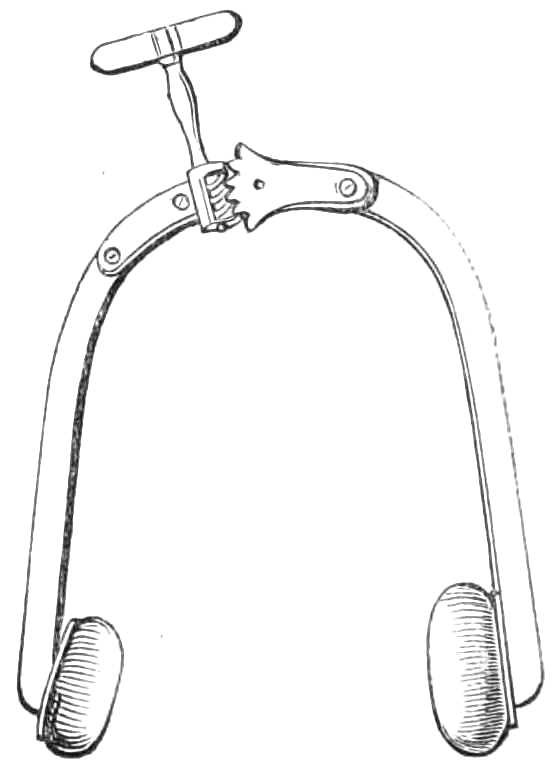
Fig. 99.—The horse-shoe tourniquet.
In Signoroni’s Horse-shoe tourniquet (fig. 99) the extremities of the shoe can be approximated to each other by a rack screw working a hinge. The ends are furnished with pads, one broad and flat to bear on the limb away from the artery, the other rounded to compress the vessel itself. This tourniquet does[Pg 149] not arrest the whole circulation in the limb. It can therefore be applied for a longer time than Petit’s. However, it easily slips out of place, and soon becomes very irksome and painful.
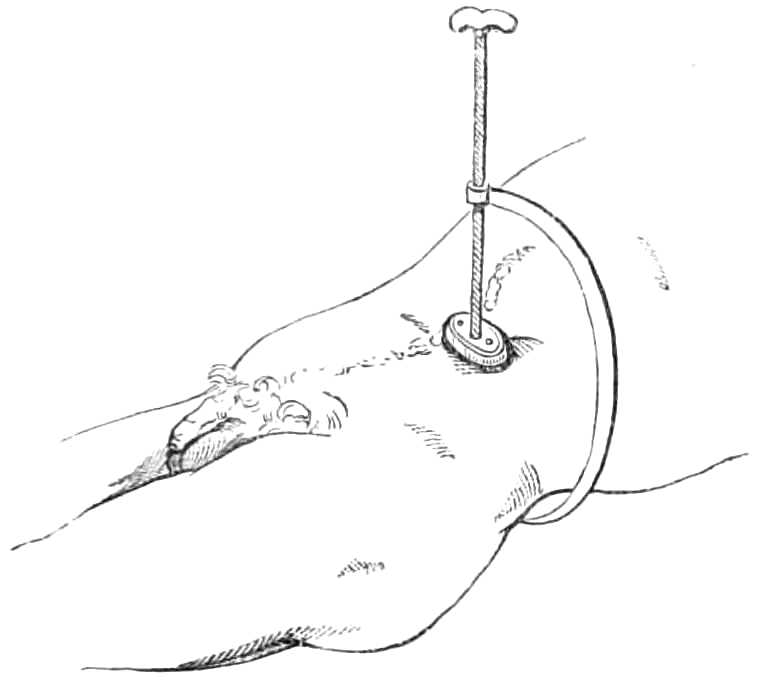
Fig. 100.—Lister’s tourniquet for compressing the aorta.
The Abdominal Tourniquet of Professor Lister is a very effectual contrivance for compressing the aorta during amputation through the hip joint, and operations where a tourniquet cannot be placed on the limb. It consists (see fig. 100) of a semicircular bar, with a broad pad to fit on the lumbar vertebræ behind, while in front it holds a long screw-pin carrying a pad. This instrument passes round the left side, and its pad is forced down into the abdomen, one inch to the left of the umbilicus, until the aorta is compressed against the spine.
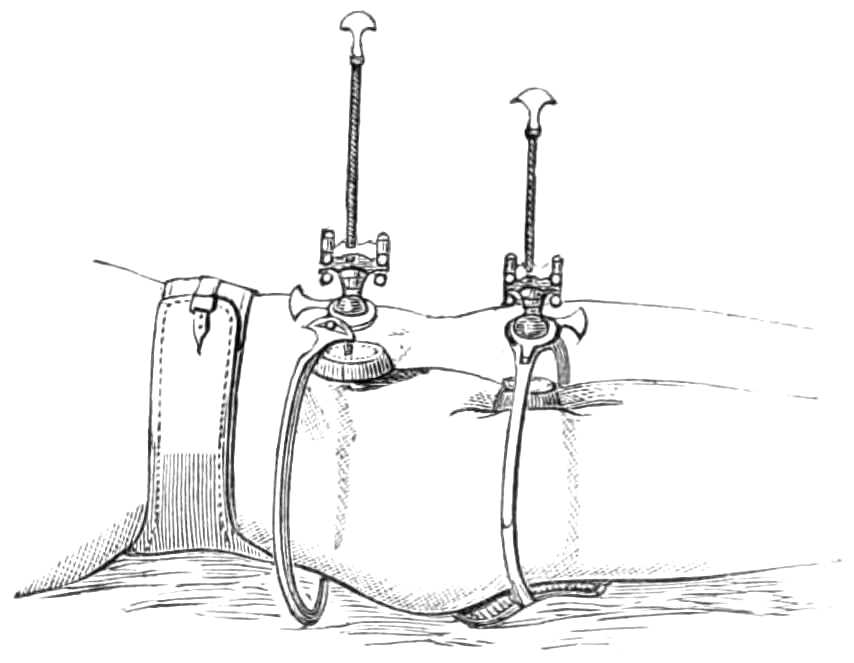
Fig. 101.—Carte’s tourniquets for femoral aneurism.
Carte’s Tourniquets (fig. 101) are employed to control and diminish the flow of blood through an aneurism. They are intended to be worn for several days, and are[Pg 150] fitted with many contrivances for obtaining a continuous pressure on the artery without completely arresting the flow of blood. They are always used in pairs; in the figure, one presses the external iliac on the pubes, the other the femoral artery. The first is fastened to the body round the hips, the second round the thigh. They are constructed as follows: an arm attached to a pad reaches round the limb to the artery, over which it supports a ball and socket joint turning in any direction, but fixed by a screw clamp. This joint has a long screw carrying the compress down to the artery. There is a little play of the screw in the ball of the joint, controlled by india-rubber bands, that the compress may yield slightly before the arterial pulse. In the solidification of an aneurism by this means, the flow of the blood is intended to continue; hence the current through the vessel need not be completely obstructed by the pressure of the tourniquet,[Pg 151] and the elastic bands prevent that pressure from becoming insupportable.
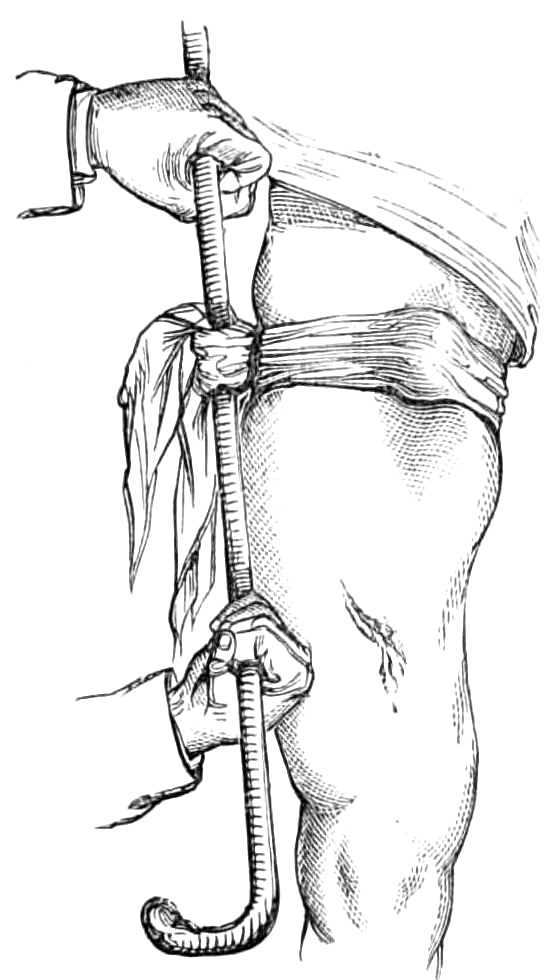
Fig. 102.—An improvised tourniquet.
When the tourniquets are applied, the patient must lie on a flat hair mattress, have his limb well washed and dried, lightly but evenly bandaged, and somewhat raised. If the thigh is hairy it should be shaved where the pads will press, and dusted with powdered French chalk. The tourniquets are next adjusted, as seen in fig. 101; the patient is taught to change the pressure when it grows irksome, by screwing down the second pad, and then releasing the first.
To improvise a Tourniquet.—A tourniquet may readily be formed on emergency from a handkerchief, a stone, and a stick. Fold a stone the size of an egg in the middle of a handkerchief, lay it over the main artery, tie the ends of the handkerchief round the limb, slip the stick underneath and twist it round, till the tightened handkerchief draws the stone on to the artery and arrests the flow of blood (see fig. 102).
Fumigation.—Mercurial vapour baths are contrived in various ways. The following plan succeeds[Pg 152] perfectly well when the whole surface of the body is to be exposed to the vapour (fig. 103).
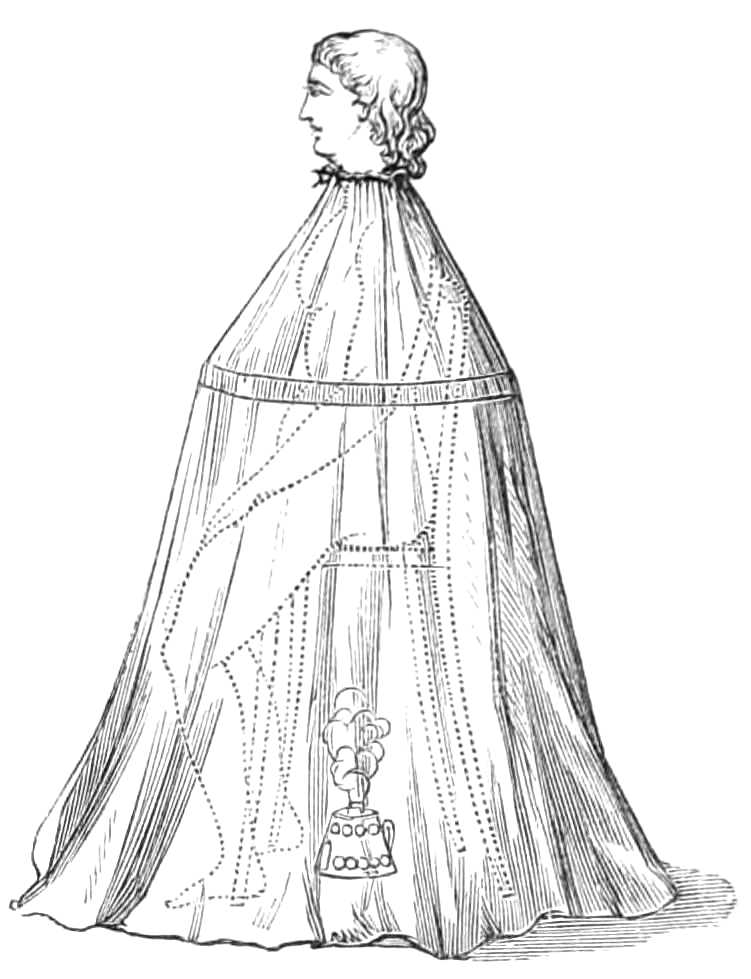
Fig. 103.—Mercurial fumigation.

Fig. 104.—Lamp for fumigating.
Apparatus.—A Langston Parker’s lamp made by Savigny and other instrument makers. In this a spirit lamp, holding the required amount of spirit is protected in a cage, on the top of which is a receptacle for the calomel, and a small saucer for water (fig. 104). The flame beneath[Pg 153] boils the water and volatilises the calomel. Water is added, because the calomel vapour, when associated with steam, acts more efficiently than with dry air.
The lamp is placed under a high wicker chair, on which the patient sits undressed, and round his neck, a frame is tied, made of cane hoops, with a calico cover sewn over them; this falls to the ground and encloses his body in a chamber, where the vapour is confined while absorbed into the skin. A blanket thrown over the frame completes the preparation. If a hoop frame be not at hand a lady’s wire-hooped petticoat answers the purpose quite as well.
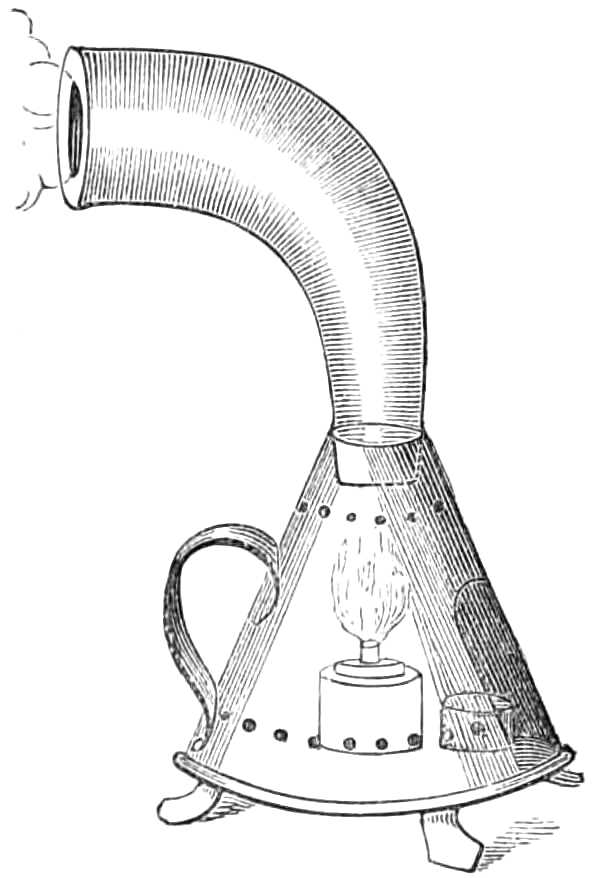
Fig. 105.—Lamp for local fumigation.
The patient, in four or five minutes, usually breaks into a violent perspiration, his pulse quickens much, sometimes even syncope occurs; hence, he should not be left alone until the bath is over. This, if the flame is strong and the quantity of calomel not very great—one or two scruples being a common dose—occupies a quarter of an hour. When the bath is over the patient should at once get into bed, and lie there a few hours; then he may rise and be well sponged with tepid water. Moderate but tolerably speedy mercurialisation of the system is thus induced.
[Pg 154]
Local Fumigation is employed when the disease is confined to a few obstinate patches of eruption. For this purpose an earthenware alembic (fig. 105) is fitted to the lamp used for general fumigation; the calomel is thrown into the bottom of the alembic. The flame plays over the outside, and heating it, sublimes the calomel; which reaches the mouth of the alembic and condenses on any part to which it is applied.
The throat may be fumigated by inhaling the vapour as it escapes from this alembic, or by sucking air through the spout of an earthenware teapot in which the calomel has been placed, and heated by a spirit lamp underneath.
The Hot Air-Bath is easily obtained by undressing the patient, putting him to bed on a mattress, and fastening across the bed two or three lengths of cane or stout wire, over which a blanket is next thrown. The patient’s body is thus enclosed in a small chamber, the air of which is then heated by putting inside, on an earthenware plate, a spirit lamp, surrounded by a kitchen lemon-grater to protect the bed clothes from its flame. Sheets should be dispensed with while the lamp is alight, lest they catch fire. The temperature of the air should be watched, lest it grow hot enough to scorch, but it must be kept up till the patient breaks into a sharp perspiration, when the lamp may be removed and the patient allowed to cool slowly down.
The action of the bath is greatly accelerated by sponging the patient all over as he lies in bed with tepid water, when the air grows warm.
[Pg 155]
Lamps protected with wire gauze, and furnished with a cradle to keep the bed clothes up, are sold at the instrument-makers, but the above arrangement answers just as well as more elaborate apparatus.
The Vapour Bath.—The patient is put to bed as in the hot-air bath, and a few feet of vulcanised india-rubber tubing, fastened to the spout of a tea-kettle on the fire, bring a supply of vapour into the bed.
The vapour bath may precede the hot-air bath, and will quicken the action of the latter very greatly.
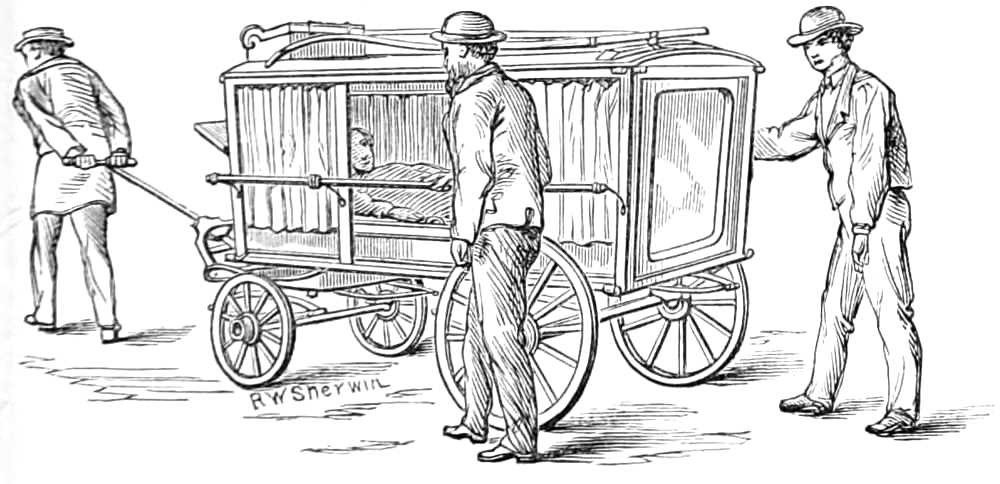
Fig. 106.—Dr. Horace Swete’s village ambulance or sick carriage.
Carriage for transporting the Sick.
The army ambulance and the carriage of the Invalid Carriage Society are excellent means for transporting sick from their homes, or wounded persons from the scene of injury to the hospital. As their cost is somewhat considerable, a cheap carriage (see fig. 106) has been devised by Dr. Horace Swete, of Weston-super-Mare, for the use of the district in which he is residing, and which may be kept for use at workhouses, hospitals,[Pg 156] and in remote districts. It is constructed of varnished wood and iron, and in the following manner.
The dimensions of the carriage are—length, 7 feet 6 inches; breadth, 3 feet 9 inches; height, 4 feet 9 inches. Its weight is under 3 cwt., and its total cost 21l.
The body is like a skeleton hearse, without fixed floor or sides. The sides are closed by vulcanised india-rubber curtains, or by glass sliding panels. The back, a wooden panel, opens like a door. A wooden tray slides on three rollers at the bottom, and on this a mattress covered with vulcanised india-rubber is placed to receive the patient. For infectious cases straw should be used instead of the mattress, as it may be burnt when the patient is removed. The tray is narrow, and fitted with handles, that it may be carried up a narrow staircase. The vehicle runs on four wheels, is fitted with lamp, handle, shafts, and driving box, and is well hung on good springs. The material of the carriage admits of being washed, and thus readily purified, after conveying an infectious case.
Cupping—Dry, and Bleeding Cupping.
Apparatus.—1. A series or nest of exhausting glasses.
2. Different sized boxes of lancets for incising the skin, called scarificators.
3. A spirit lamp (fig. 107).
The glasses are 6 oz., 4 oz., 2 oz., and 1 oz. in size, of rounded shape, with thick smooth edges.
In dry cupping the object is to relieve internal congestion by drawing the blood into the subcutaneous[Pg 157] cellular tissue. The back and loins, where the skin is tolerably loose, are most suitable places for this proceeding.
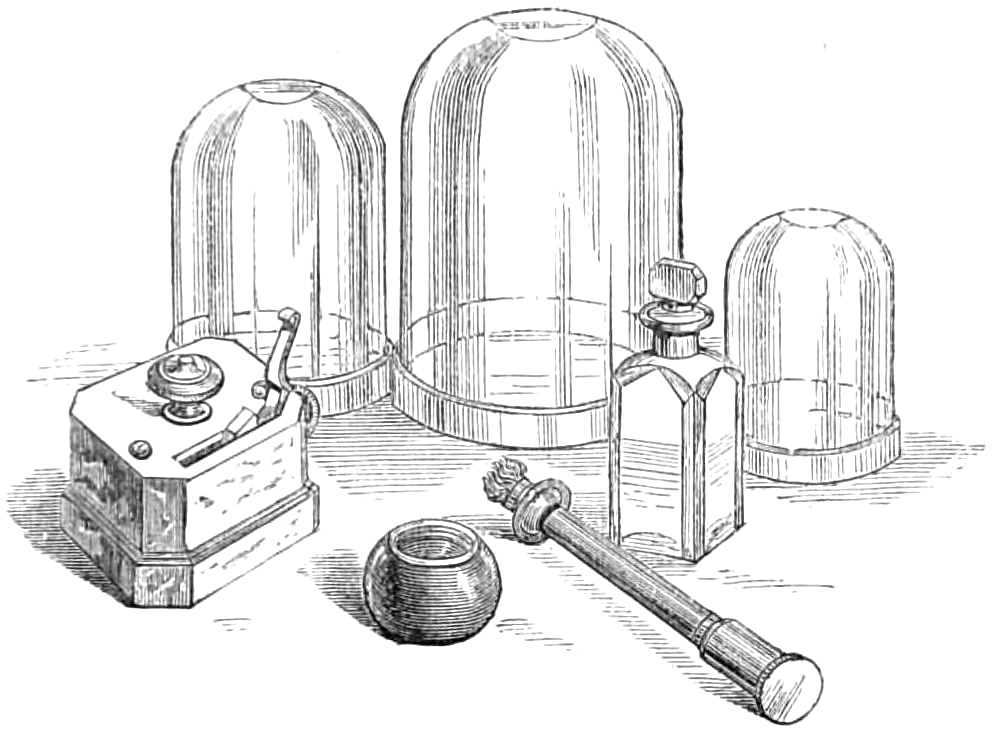
Fig. 107.—Cupping glasses, lamp, scarificator, and spirit bottle.
The Operation.
Step 1. Light the spirit lamp, direct the patient to sit forwards, and lay bare the back ready for the glasses, which should be placed on the bed within reach of the operator’s right hand.
Step 2. Rarify the air in a glass by plunging the flame into it a few moments, and then quickly clap the mouth of the glass on the skin; leave it there while a second and third glass are heated and applied, when the first should be removed and its vacuum restored before it is replaced. In putting the glasses on again, their rims should not lie exactly in the rings marked on the skin by previous applications, or the bruises may inflame and slough afterwards at these parts.[Pg 158] The application and removal of the glasses should be done as lightly as possible to prevent all unnecessary pain.
A few repetitions of this incomplete vacuum causes the skin to puff up readily into the glasses, and much blood is thereby attracted into the cellular tissue.
Bleeding or Bloody Cupping.—When it is desired to take blood from the body the skin is punctured or scarified by the scarificators, half a dozen incisions being made at a blow by as many lancets protruding from a box, when a spring it holds is touched; the glasses are then laid over these incisions, and the necessary amount of blood removed by their exhausting power.
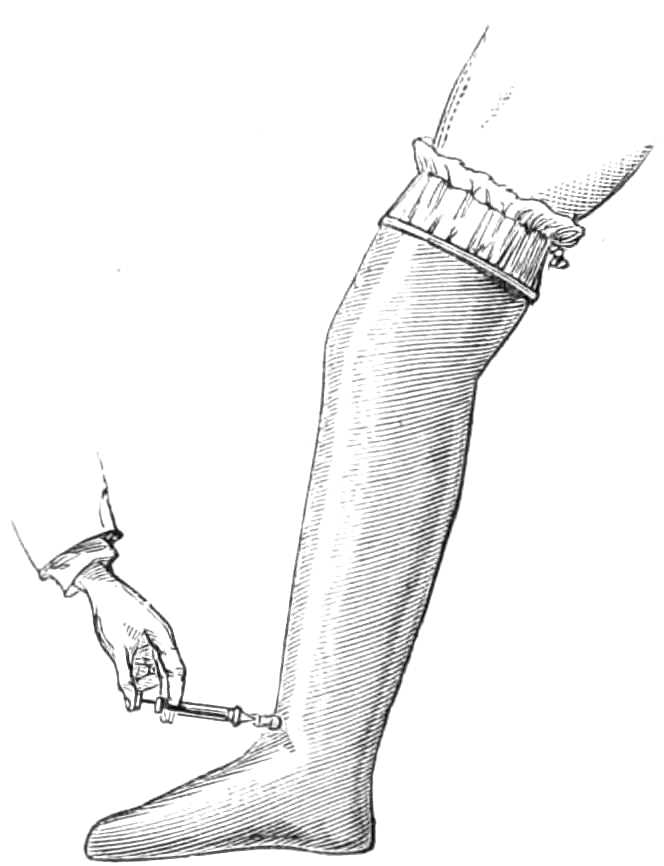
Fig. 108.—Junod’s vacuum boot for attracting the blood to the lower extremities.
Junod’s Boot is a tin case, shaped like a boot (see fig. 108), but capacious enough to allow a limb when placed within it to swell freely. It is sometimes employed to draw blood and serum into the lower extremities during congestion of internal organs. When used, the leg is passed into the boot, and the mouth of the boot closed round the limb by a packing of india-rubber tied firmly round the boot and limb,[Pg 159] and well smeared with simple ointment. The air is then exhausted from the inside of the boot by a small brass syringe, which screws into a hole in the leg of the boot, as depicted in the figure. The patient should wear the boot some two or three hours, while the vacuum is kept up by an occasional exhaustion of the syringe. Both limbs may be subjected to exhaustion, but the patient must remain in bed for twenty-four hours after the operation; this is generally necessary for other reasons, and he must wear a bandage for a few days when he gets about.
Leeches.—Each leech should draw about 2 drachms of blood, and if the bite is well fomented, another drachm will escape from the wound afterwards.
Before the leeches are applied, the skin should be well washed with soap and warm water, and carefully dried. The leeches should not be taken from their box, but the box inverted over the part, when they will quickly fasten themselves. If the leeches are applied in a dependent position, a soft napkin may be pinned round the box to support them as they grow heavy, and to enable them to suck as long as possible. They should be allowed to drop off; if pulled off they are apt to tear the wound, or leave part of their suckers in it, which causes much irritation afterwards.
The leech is put in a little glass when applied to the gums or the cervix uteri, and held against the part he is to suck.
If the leeches do not bite readily the part should be smeared with blood or warm milk, and the leeches put into lukewarm water a few minutes; immersion[Pg 160] in small beer is also said to stimulate them to bite.
If the bites bleed longer than is desired, they may be stopped by pinching the skin between the finger and thumb, wiping the bite thoroughly dry, and filling it with a little bit of amadou or fine sponge, soaked in solution of perchloride of iron; a larger piece of amadou is placed over the first, and the whole compressed with a turn of a bandage or long strip of plaster. If this fails, a sewing needle may be passed through the skin beneath the floor of the bite, and the bleeding surface constricted by twisting a thread round it under the needle.
Leech-bites should never be left bleeding, especially in children, for a dangerous amount of blood may be lost from them in a few hours.
Tents are instruments made of some substance that enlarges as it absorbs liquid; they are employed to dilate apertures of sinuses or natural passages, as the cervix uteri, &c., and are generally short rods 2 to 3 inches long, and 1/10 to ¼ inch in thickness, made of a whalebone stem, wound round with compressed sponge, which is smeared with wax to keep it in shape. Slips of gentian root, or of laminaria digitata, which rapidly enlarge as they imbibe moisture, are also employed for this purpose.
Setons are strips of varnished calico, 6 or 8 inches long and ⅓ broad; a thread is fastened to each end, which are tied together while the seton is worn. It is employed to excite irritation either along the course of a sinus, or in some superficial situation, as the nape of the neck, to relieve congestion of internal parts. In[Pg 161] sinuses, a few threads of silk usually produce the required amount of irritation.
Chassaignac’s Drainage-tubes are a form of seton; they are india-rubber tubes of the calibre of a wheat straw, of any requisite length, and perforated with holes at frequent intervals; they are carried into the cavity to be drained, by hitching the prong of a forked probe, made for the purpose, through one end of the tube and thrusting it along the sinus, or across the abscess. The skin is then incised over the further end of the sinus to bring the probe out, and the ends of the tube are tied together.
The advantages of these tubes are, the small amount of irritation they provoke, and the ready exit furnished for the matter along their interior.
Issues are a contrivance for keeping up irritation of the surface. A piece of diachylon plaster the size of a half-crown, with a hole in the centre as large as a pea, is laid over the skin where the issue is to be formed. A bit of potassa fusa is laid in the hole and kept in sitû by a second plaster, for an hour or till the skin is destroyed under the hole. The plasters are then removed, the wound washed, and a fresh piece of the same size put on, having at its centre a slit ¼ inch long, under which a pea is slipped into the sore and covered over by another smaller piece of plaster. The discharge that soon sets up must be washed away twice daily, and the plaster and pea renewed from time to time as they become soiled.
Trusses for ruptures. These are various, in shape, strength of spring, &c.
Whatever variety of truss is employed, care should[Pg 162] be taken that the pressure is made in the right direction, and that it is sufficient, but not too great for the strain it has to support.
In reducible hernia the pressure for inguinal rupture should be exerted on the inguinal canal and directly backwards (see fig. 109). For umbilical rupture, the pressure should be also backwards, and confined as much as possible to the aperture in the wall of the belly. In femoral rupture the pressure should be directed upwards as well as backwards into the femoral ring (see fig. 110). The pad in all should be large enough to well cover the passage through which the rupture passes. The ease and comfort of a truss much depend on the completeness with which it fulfils these conditions.
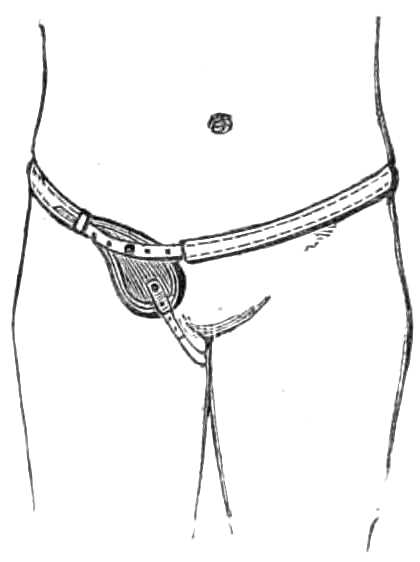
Fig. 109.—Inguinal truss.

Fig. 110.—Femoral truss.
The adequacy of a truss should always be tested by directing the patient to separate his legs, lean forward over the back of a chair, and cough or strain deeply. If the truss support the rupture during this exertion it fits satisfactorily.
[Pg 163]
For irreducible hernia large air-, or spring-padded trusses are made, which prevent further descent of the viscera, but they are exceedingly difficult to fit and often unsatisfactory in use.
In inguinal hernia the truss consists of a pad, a spring, and a neck, with guide straps.
The pad is made of various materials, fine carded wool is among the best when well stuffed into a proper shaped leather pad, and in most cases a fixed pad is better than a moveable one.
The pad should compress the canal and be convex if the patient is stout. Its size ought to be sufficient to compress the canal and the margins for a short distance on each side, but the pad should be as small as will ensure fair compression. A very flaccid bellywall, and a large gap or protrusion require a large surface on the pad. The spring should be supple and padded behind to rest on the two sacro-iliac synchondroses, without bearing on the spine. The spring, narrowing as it comes forward, embraces the pelvis; and opposite the anterior iliac spine inclines downwards, because the hernia is a little lower than the resting-place of the spring behind. When the rupture is almost reached, the spring takes a slight elbow or bend (the neck), that its pressure may be directed against the hernia more fully. Understraps, generally not necessary, should be omitted if possible.
In trusses for children when the testis is not descended, the pad should have a notch at its lower border in which the testis may rest uncompressed.
In the truss for femoral hernia, the spring bears behind the body and encircles the hips in the same[Pg 164] manner as in the inguinal truss, but when opposite the femoral artery it turns abruptly downwards to reach the saphenous opening. The pad should fit the hollow where the rupture issues and be not oval, but rounded. The under-strap should be attached to the stud at the lower end of the pad, and pass round the perinæum and fold of the buttock, and be attached to the neck of the spring close to the pad. It should be made of knitted bandage that it may be changed and washed frequently.
When measuring a patient for an inguinal truss, the circumference of the body round the hips (between the crista ilii and the great trochanter) should be first taken, and then that between the symphysis pubis and the anterior iliac spine, half of which distance denotes the position of the internal abdominal ring, which with the inguinal canal has to be supported by the pad of the truss. For a femoral hernia the same measurement should be taken round the body, and also the distance of the saphenous opening from the symphysis pubis and from the anterior superior iliac spine. This will enable the maker to put the pad at the proper angle with the spring, so that it compresses the saphenous opening, and clears the crest of the pubes.
Every patient should, while he wears a truss, show himself from time to time to the surgeon to see that any defect in his apparatus may be quickly remedied. It is a useful precaution also to keep two trusses at hand, so that if one breaks, the patient may at once apply the other.
Salmon and Ody’s truss consists of a spring passing round the hip from a circular pad b, which bears on[Pg 165] the sacrum to a second oval pad a. Both pads are attached to the spring by a ball and socket joint. There is also a slide for shortening or lengthening the spring if desired (fig. 111). This truss is worn round the sound side of the body and reaches beyond the middle line to the hernial opening, with the object of directing the pressure of the spring outwards and backwards, or exactly counter to the course of the hernia inwards.

Fig. 111.—Salmon & Ody’s truss.
Umbilical hernia.—Spring trusses are not adapted for restraining umbilical hernia. The support consists of a broad belt fitted to the belly, made in front of elastic webbing, and on each flank, of white jean. Behind, the belt is fastened by straps and buckles, or by lacing, the better plan. In the centre, the elastic part carries a nearly flat air-cushion, measuring about 3 inches transversely and 2½ vertically. This cushion is placed against the aperture of the belly, and presses back the protrusion. The size of the pad varies with the size of the hernia, but it should always largely exceed the extent of the gap in the abdominal wall. The pad, when the apparatus is used for an infant, should not be too prominent, as it is then more difficult to keep in place, and also by pressing into the aperture hinders it from closing. The pad for an infant is best made of a disc of ivory, 1½ inch broad and ½ an inch to 1 inch thick, stitched in a little case[Pg 166] in the centre of the girdle. The quantity of elastic tissue should be much less in the infant’s belt than in those for adults that the belt may be frequently washed. The difficulty of keeping the belt in place is obviated by attaching two bands to the upper border, to pass over the shoulders and cross behind before fastening to the belt, like braces. Two similar ones may be fastened to the lower border and carried under the thighs. These bands should be of soft webbing, and several pairs kept in store, that they may be frequently changed and washed.
Cauteries.
Cautery irons.—These are masses of iron of different shapes; some pointed, others rounded like buttons, &c., set in a stem a foot long, fixed in a thick wooden handle. They are heated in a charcoal brazier or common fire to bright redness if required to destroy deeply, but short of redness if intended only to scorch the surface.
As these irons are inconvenient for many cases from their bulk, and yet soon lose their heat if made small, other cauteries have been devised to which the heat can be quickly renewed.
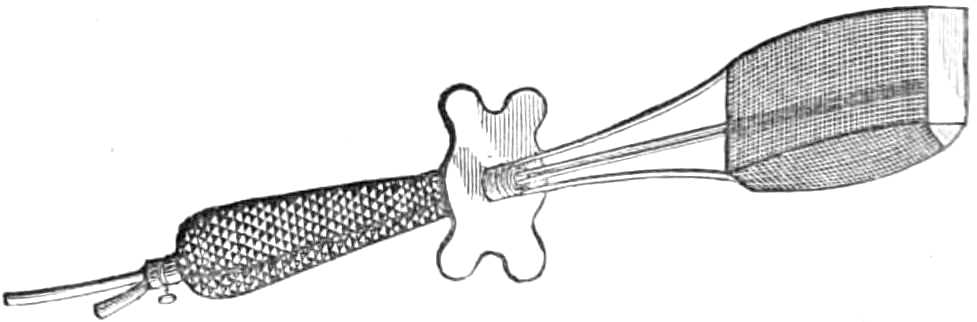
Fig. 112.—Gas cautery for large surfaces.
Gas Cautery.—The late Mr. Alexander Bruce perfected an instrument which employs the gas flame[Pg 167] as a source of heat (see figs. 112, 113). A blowpipe flame plays on platinum discs of various sizes, and keeps them at a glowing heat. This hot solid point can be thrust into the tissue wherever it is desired.
A larger form is also made for cauterising the pedicle in Ovariotomy, &c. In this a large flame is blown on a wedge-shaped surface of platinum, 1 inch long and ½ inch broad, and continued backwards for 2 inches by wire gauze to confine the flame against the platinum. The flame behind these platinum discs quickly heats them again if cooled by the blood. This cautery is very portable, and easily made ready for use.
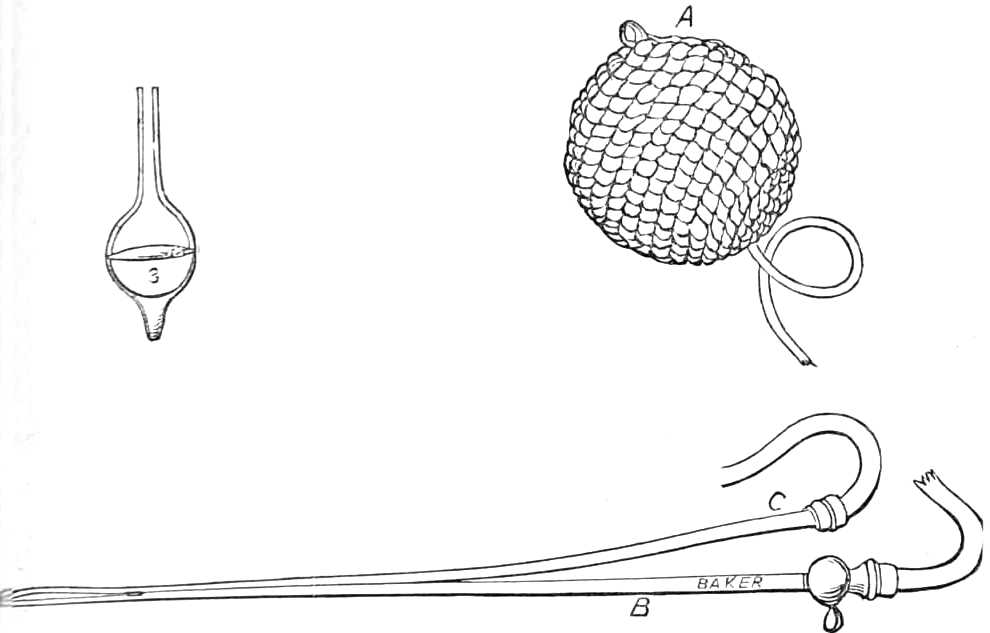
Fig. 113.—Gas cautery. A. Elastic gas reservoir. B. Gas jet. C. Tube for convoying air to the flame. 3. Platinum disc to be heated by the flame.
[Pg 168]
Mr. Clover has also devised a cautery, very useful for small growths. A silver bead, the size of a pea, is set at each end of a horizontal metal rod 4 inches long, which rotates on a vertical pivot half a circle backwards and forwards, so that one or other bead is thrown into the flame of a spirit lamp placed at a proper distance; when the bead is heated, a touch of the finger causes the central pivot to rotate, which brings the hot bead away from the lamp, and carries the cold one into the flame, to be heated while the first is used.
Galvanic Cautery.—The instrument consists of a platinum wire, made to glow by passing through it a powerful galvanic current. The wire should be thick (about 1/12 of an inch), and all the other conducting surfaces sufficiently large to offer no impediment to the current where heat is not desired. The battery best adapted for this purpose is a Grove’s battery.
The main advantage of a galvanic cautery is that the wire can be passed while cold exactly where it is required, and then heated when it is in place. It is exceedingly useful in fistulæ between the urethra and rectum, or in destroying vascular growths, nævi, &c., where it is desirable not to destroy all the skin covering the tumour. Again, by this means, an intense heat can be applied to a very limited area, and more quickly renewed than by any other plan, for the wire, even when plunged in the tissue, is never far below a red heat.
Of chemical caustics a host exist; those most commonly employed are:—nitrate of silver, solid, or in saturated solutions (2 drachms to the oz. of water,[Pg 169] &c.); fuming nitric acid; solution of nitrate of mercury in nitric acid; oil of vitriol made into a paste with powdered charcoal; chloride of zinc mixed with dry starch, then rolled into cakes and cut in slices; Vienna paste, that is, equal parts of potassa fusa and quick lime worked into a paste with spirits of wine; potassa fusa itself; solution of chromic acid. Some surgeons prefer one, some another; as a rule, the liquid caustics are employed where the surface to be destroyed is uneven and spongy, and solid caustics where the surface is smooth, and a long continued action is desired.
Vesicants and irritants.—Of the commonest are mustard poultices, made by mixing mustard flour in a basin with luke-warm water, i.e. about 100° F., to a paste and spreading it on muslin, which is again folded over the exposed surface of the mustard. Boiling water and vinegar should not be used, for they lessen the pungency of the poultice. If the full effect be desired the poultice should remain on the skin fifteen or twenty minutes. If only slight reddening is wanted, the mustard flour should be diluted with its bulk of linseed meal before mixing it with water.
A stronger vesicant is Corrigan’s hammer, a button of polished steel with a flat surface, fixed to a handle; when used it should be plunged for a couple of minutes in boiling water, or heated over a spirit lamp, but care must be taken not to overheat it, or it will bring the cuticle away with it. It is pressed on the skin for ten or fifteen seconds; this is sufficient to cause reddening and vesication.
[Pg 170]
Blisters are raised by the emplastrum lyttæ, lin. cantharidis, or pâte epispastique, which is milder in its effect than the two preceding preparations of Spanish fly. Solution of iodine and iodide of potash, in three times their bulk of spirit of wine, also produces a blister when laid on freely.
Poultices are made of linseed meal, bread, or starch, and are means for applying warmth and moisture without absolutely wetting. Bread poultices sodden the parts to which they are applied most, and starch least, of the three kinds.
Before making a poultice all the materials should be at hand and thoroughly warmed before a good fire. They are—boiling water, a broad knife or spatula, soft old linen or muslin, oil silk, tapes, strapping plaster, bandages, a piece of old blanket, flannel or cotton wadding, safety pins, or needle and thread.
The linen on which the poultice is to be spread should be cut of the intended size, and when for use about the neck or shoulder should have some tapes sewn on to it to tie it on to the body. The oil silk should be large enough to cover the poultice next which it is laid to keep in the moisture. The flannel or wadding are used to wrap over and keep in the heat of the poultice; the strapping or bandage to fix every thing in situ as required.
When poultices are continued long, their surfaces should be smeared with lard before application; this protects the skin somewhat from the irritation that arises; also when the poultice is to be laid between folds of skin or on hairy situations, as the buttocks and perinæum, it is better to cover the poultice with[Pg 171] a thin cambric handkerchief lest some of the meal stick to the parts.
The Linseed Poultice is made as follows: pour boiling water into a well-heated basin till the basin is half full, then scatter meal with the left hand on the water while that is kept continually stirred with a broad knife, adding more and more meal until the mass becomes quite soft and gelatinous, but too stiff to cling to the knife; then turn it out on the linen, also well heated at the fire, and spread it in a layer about ½ an inch thick, turn up the edge of the linen for ½ an inch all round, and carry the poultice at once to the patient. If it has to be carried far the poultice should be laid between two very hot plates; apply it to the part to be poulticed, lay on the oil silk, and cover that with the hot flannel or cotton wadding, and fasten these in place with pins or a stitch. Wadding is put where the part is irregular, as the neck or axilla; unless the wadding is well placed and the poultice is fastened by strings, it will soon fall into a narrow band leaving the part exposed that it should warm and moisten.
The Bread Poultice is made as follows: the materials being all at hand, as detailed in the directions for making a linseed poultice, crumble the inside of a moderately stale loaf until about half a pint or a pint of crumbs are prepared; then pour boiling water into a basin, and throw in crumbs gradually in the same manner as the linseed meal, until a soft porous mass is prepared. The remaining steps are the same as those for making the linseed poultice.
The poultice can be made to hold more water if it is[Pg 172] turned into a saucepan after mixing, and a little more water added while it simmers for half an hour at a slow fire. Any superfluous water must be drained off, and the poultice covered with muslin when it is made in this way.
The Starch Poultice is made as follows: rub a little starch in a basin with cold water till it has the consistence of cream, then mix in boiling water till the starch is a thick jelly, and spread it on the linen while hot. Starch poultices retain their heat a long time, but yield very little moisture to the part. They are chiefly used as emollients to inflamed affections of the skin, &c.
Hot fomentations are a means for applying heat when moisture is not desired. A ready mode is to take a piece of blanket or thick flannel, soak it in boiling water and dry it by wringing in a folded towel, and then wrap it over the part to be fomented with a piece of oil silk or a hot dry flannel over it. Laudanum, turpentine, and other applications are sprinkled over the flannel, when soothing or counter-irritating effects are required in addition to the warmth. A bag of bran makes a light warm fomentation if heated in a steam kitchen, or steamer for boiling potatoes.
When absolutely dry heat is desired, chamomile flowers, bran, or sand, may be heated in an oven, and poured into hot flannel bags.
Dry heat is also very agreeably obtained by filling india-rubber bags and cushions with hot water: they are rather heavy, but retain their heat many hours.
Lister’s Method of Dressing Wounds with Carbolic[Pg 173] Acid.—The properties of carbolic acid which concern the surgeon may be briefly recapitulated as follow:—
It is highly volatile, and the putrefaction of organic fluids is indefinitely postponed where its vapour is present. Carbolic acid is soluble in different degrees in water, alcohol, ether, glycerine, fixed oils, gutta percha, india-rubber, and shell-lac. Its varying affinity for these substances enables the surgeon to modify the application of carbolic acid in various ways; these modifications are necessary to fully utilise its properties. Water dissolves the crystallised acid but sparingly, 1 part in 20 being a concentrated solution, and allows it to escape readily. The aqueous solution is therefore useful where the effects of the acid are required copiously, but only temporarily. Glycerine and the fixed oils dissolve a far greater amount of the acid, and part with it unwillingly. Their solutions are adapted for the continuous but abundant application of the antiseptic. Shell-lac, and some other substances, hold the carbolic acid still more tenaciously, and are valuable as solid storehouses which yield up the antiseptic in small quantity for a considerable period.
Carbolic acid stimulates raw surfaces, and when concentrated even destroys animal tissues. It is a local anæsthetic; with moderate doses, wounds lose their sensibility after the first smarting of the application has passed off. When given in large quantities the acid produces a peculiar kind of delirium, and temporary paralysis of sense and motion: fatal results have followed its internal application.
It is rapidly absorbed into the blood from wounded[Pg 174] surfaces, and through the skin, whence it is discharged from the body by the lungs and kidneys. The urine of patients dressed with carbolic acid, though of normal colour when passed, assumes a dark greenish-brown hue after a few hours’ exposure to the air and light.
How much of the antiseptic must float in the atmosphere to prevent fermentative changes has not yet been determined; Bucholtz found that 1 part of carbolic acid in 600 of milk almost entirely prevented lactic fermentation, while 1 in 285 did so altogether. Alcoholic fermentation in sugary fluids was arrested by a similar quantity.
When using the acid in dressing wounds, the watery solution, the solid mixture, and the oily solution are necessary. The first to neutralise the effects of exposure to the atmosphere and water before the wound is closed; the second solid mixture in the form of plaster to provide a very scanty but continuous supply of carbolic vapour close to the wound: too scanty to irritate the raw surface, yet enough to check putrifaction in the discharge oozing from it. The third, or oily solution, is to supply the carbolic vapour abundantly to the linen dressings, appointed to receive the discharge when it has passed from the vicinity of the wound. The tin is used to afford as close a cover as possible to the breach of surface; for this purpose it must be as flexible as possible that it may fit the wound exactly.
The carbolic plaster is made of 3 parts of shell-lac and 1 part of carbolic acid crystals melted together and spread on calico. To render the lac plaster non-adhesive that it may not stick to the tender wound,[Pg 175] it is painted with solution of gutta percha, which dries and leaves a thin film of that substance covering the plaster. This film is easily removed by rubbing the surface with a rough towel should an adhesive quality be desired. In either state the carbolic acid continues to volatilise slowly when the plaster is laid over the wound.
When adopting this method of treating wounds the following materials are necessary:—
1. Aqueous solution of crystallised carbolic acid (1 part in 20).
2. Carbolic oil: 1 part of carbolic acid in 5 of olive oil.
3. Lister’s shell-lac plaster.[1]
4. Sheet tin.
5. Lint; old linen.
6. Diachylon plaster.
7. Glass syringe.
8. Scissors.
9. Thin calico or muslin.
10. Bandage.
11. A wooden splint to rest the limb upon.
To Dress recent Wounds.—When the apparatus is ready, the piece of tin is cut and fitted to the wound, so that it shall overlap the wound to a small extent on all sides; then a piece of lac plaster, large enough to overlap the tin one or two inches all round; this plaster may be cut and notched when the surface is irregular to make it lie pretty closely; then strips of[Pg 176] diachylon, about two inches broad, are cut ready. The parts around the wound are well cleaned; dirt and clots cleared from the wound with cold water, containing about 1 of carbolic acid to 40 of water, and the interior of the wound is freely syringed with water containing 1 of acid in 30 or even 1 in 20 parts. The sides are brought together with sutures, if necessary, in the ordinary way, and the tin laid on the wound; the tin is freely wetted with carbolic water, and the lac plaster laid over it and kept in situ by strips of diachylon plaster. In dressing recent wounds the most dependent side of the lac plaster is left unattached, that the serous discharge, which is often copious, may readily escape. To receive this discharge, a piece of calico, soaked in carbolic oil, is laid over the wound now covered in, and all kept in place by a folded towel or a roller bandage. This oily cloth is to be changed from time to time as it gets soaked with discharge: at first this change is necessary every night and morning, but after three or four days once a day is often enough. The shell-lac plaster and tin need not be removed for a week unless the wound grow hot and painful, when they can be removed at any time if the surface of the wound is immediately smeared with carbolic oil, and kept well imbued with the antiseptic while it is being examined. Should it contain pent-up discharge, the sutures must be loosened and the discharge washed out by injecting the 1 in 30 aqueous solution. The tin and lac plaster may be then replaced, and the dressing renewed. The same precaution must be followed when the sutures have to be removed. Usually there is very little[Pg 177] swelling and no pain, and the healing process goes on tranquilly if undisturbed. Should bruised parts slough, they may be trimmed away with scissors dipped in carbolic oil. When the wound has once been washed with carbolic acid, the antiseptic should not enter the wound a second time, as its irritant qualities excite inflammation in the wound.
Chronic abscesses, besides recent wounds, are treated with carbolic acid. The surface to be punctured is covered with a piece of thin muslin soaked in carbolic oil, and the knife to be used is dipped in the oil also. Then, a second piece of muslin being ready, the surgeon opens the abscess through the muslin, and as he withdraws the knife an assistant lays on the second piece of muslin over the wound. The matter drains away from under this curtain, and the access of atmospheric air is prevented. When the matter ceases to flow, the lac plaster is laid on, and the oily cloth outside, which can be changed as often as is requisite. Abscesses so treated usually soon cease to secrete matter, shrink, and fill up without delay. If the abscess has burst or had communication with the external air, the interior must be filled with watery solution 1 to 20 before it is dressed, that fermentation in the cavity may be prevented; the further treatment is the same as for a recent wound.
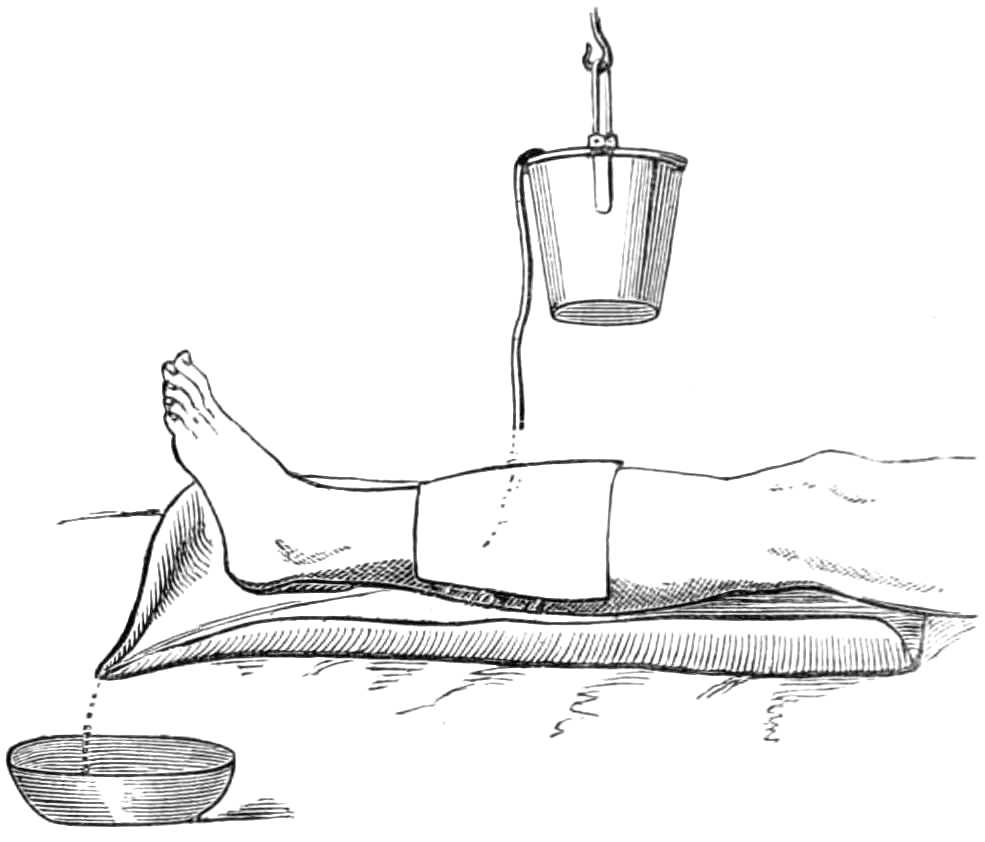
Fig. 114.—Irrigating a wound.
Irrigation.—The continual flow of ice-cold water is used to prevent inflammation of certain wounds. In using cold, it is particularly necessary that the temperature of the water remain steady, for alterations of temperature cause alterations in the capacity of the blood vessels, and promote congestion rather than[Pg 178] diminish it; hence irrigation, badly attended to, becomes an evil instead of a benefit. The simplest way (see fig. 114) of contriving irrigation is to lay the limb in an easy position on pillows, protected by a sheet of india-rubber cloth, weighted at one corner to draw the cloth into a channel, down which the water trickles into a receiver under the bed; over the limb a jar, wrapped in blanket, is suspended. This is filled with water from time to time, and kept charged with lumps of ice. A syphon is made by a few feet of fine india-rubber tubing reaching from the bottom of the jar to the wound, the escape of water through the tube being moderated by drawing the end more or less tightly through a bit of cleft stick. It is sufficient that the wound should be kept constantly[Pg 179] and thoroughly wetted; more than that is waste of cooling power.
Esmarch’s Irrigator.—This is a simple contrivance for washing out wounds and sinuses with a stream of water. It consists of a tall can of block tin (see fig. 115), with an orifice at the lower end, to which a couple of feet of india-rubber tubing are attached. The tube is fitted with an ivory nozzle and a hook, so that when the stream is not wanted the flow of water is stopped by hanging the nozzle on the upper edge of the can. The stream can be made more or less forcible by raising or lowering the can above the wound.

Fig. 115.—Esmarch’s Irrigator.
The Administration of Chloroform.—In administering chloroform the main points to be borne in mind are—1. If the patient is fit to undergo an operation at all he may inhale chloroform. 2. The patient should be fasting; this is the most effectual preventive of sickness. 3. He should be in an easy position, clad in a loose but warm night-dress, which does not interfere with ordinary or artificial respiration, should that be suddenly required. 4. The patient must never inhale more than 4 per cent. of chloroform vapour in the air he respires; on the other hand, the vapour may circulate in the blood without harm for an indefinite time, provided it never pass beyond a certain concentration. 5. Chloroform is a sedative and depressant; the pulse gives the earliest indication[Pg 180] of syncope, and the respiration should be constantly watched the whole time chloroform is inhaled. It should be noted that the pulse often fails suddenly at the first flow of blood in an operation. Again, when the patient is deeply narcotised, the jaw may gape and the tongue sink back till it closes the glottis. From this cause respiration sometimes ceases, and danger quickly arises if the chin is not drawn up to raise the epiglottis. In beginning to inhale, the quantity of vapour should be small, and gradually increased. The patient must be cautioned not to talk, to avoid the irritation and coughing chloroform sometimes excites while he is speaking. He should also shut his eyes lest the vapour make them smart. After inhalation has been continued a few minutes the patient is often quiet and inattentive, though easily roused by pain. His condition at this stage should be tested by asking him to give his hand, or by pinching him gently; if no notice be taken of these, the conjunctiva should be touched, and the amount of winking thus excited will enable the chloroformist to judge if the patient will resist when the knife is applied. Patients vary much in the time passed before recovering consciousness; if they remain soundly asleep, breathing freely and with good pulse, it is better to avoid rousing or moving them until they wake spontaneously; such patients suffer less confusion and vomiting than those who are quickly alive to what is going on around them.
Signs of Danger.—Sudden failure or irregularity of the pulse, with pallor and arrested breathing, are of great importance; if these occur, the chloroform must be at once removed, a free supply of fresh air ensured,[Pg 181] the tongue drawn gently forward, and if the breathing do not quickly begin, it must be set up artificially (see p. 183) without loss of time, and continued, if necessary, for at least an hour before recovery is despaired of. Stertorous breathing is not alarming unless accompanied by feeble pulse, shallow respiration, and dilatation of the pupils; with these it becomes a sign of a comatose condition.
As subordinate adjuvants for faintness the following are useful:—moistening the tongue and lips with brandy from time to time, or letting the patient sip a small quantity from the spout of a feeding cup. In complete syncope, galvanism to the epigastrium, a hot iron or scalding water to the præcordia may be employed, but should never interfere with the maintenance of artificial respiration, which is of far greater efficacy in restoring suspended animation than anything else.
Chloroform is safely given on a handkerchief, or in various ways, if the administrator is careful to watch the pulse and respiration, and to guard against the patient, by a sudden deep inspiration, taking too large a dose of vapour at once. Exact measurement of the quantity of liquid poured on the handkerchief at a time is of no value, as it is no index of the concentration of the air respired by the patient. Of far greater consequence is it to insure a free supply of atmospheric air, by keeping the evaporating surface a few inches from the mouth and nostrils.
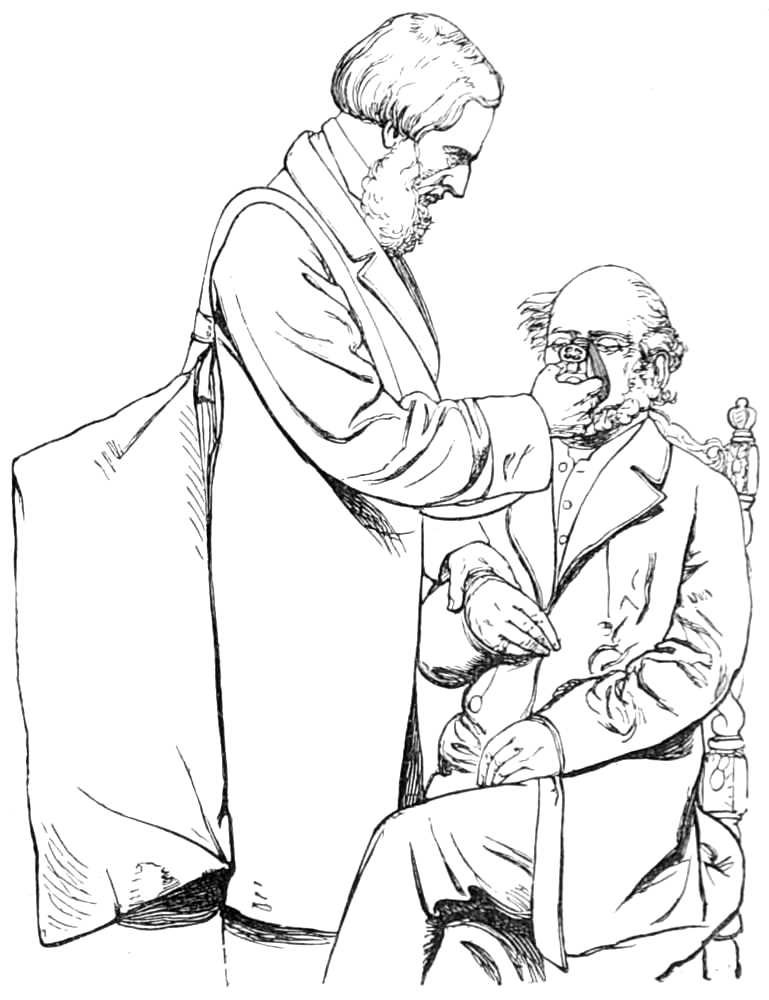
Fig. 116.—Clover’s apparatus for administering chloroform.
The safest mode of giving chloroform is by Clover’s Inhaler (fig. 116), now used in many London hospitals and elsewhere. It renders it impossible to give the patient too strong a dose, by preparing an atmosphere[Pg 182] of known strength for him to breathe. Clover’s apparatus consists of a bag of 8,000 or 10,000 cubic inches capacity, suspended by a loop behind the chloroformist’s back, from this a flexible tube brings the vaporised air to a mask, fitting over the nose and[Pg 183] mouth of the patient. This mask has a flexible metal border for adjusting it to different faces; and a valve that opens and closes, to allow more or less common air to be respired with that drawn from the reservoir if desired.
The reservoir is supplied by injecting into it, from a bellows, 1,000 cubic inches of air, drawn through an evaporating box heated by hot water, into which 32½ minims of chloroform are injected from a graduated syringe each time the bellows are filled. By these means, an atmosphere of known strength is prepared for the inhalation; that is one containing about 4° of vapour. This apparatus is very easy to use, and the most efficient in producing anæsthesia quickly and pleasantly.
Artificial Respiration.—Many plans are employed; but the two most efficient are those to be described.
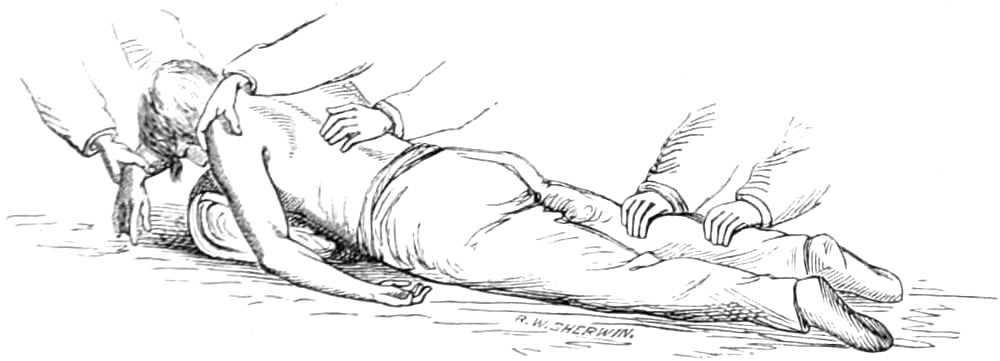
Fig. 117.—Artificial Respiration. Marshall Hall’s method. 1st position.
Marshall Hall’s Method.—Lay the patient on the floor, with the clothing round his neck, chest, and abdomen loose; if wet, remove it, and throw over his body a warm blanket. Clear out the mouth, and turn the patient on his face, one arm being folded under his forehead (see fig. 117), and the chest raised on a folded[Pg 184] coat or firm cushion. Next, turn the patient well on his side, while an assistant supports the head and arm doubled underneath it (see fig. 118), and confines his attention to keeping the head forward and the mouth open during the movements to and fro. When two seconds have elapsed turn the body again face downwards, and allow it to remain so for two seconds, and then raise it as before. This series of movements, occasionally varying the side, should be repeated about fifteen times a minute, and continued until spontaneous respiration is restored, or, until two hours have been thus spent in vain.

Fig. 118.—Artificial Respiration. Marshall Hall’s method. 2nd position.
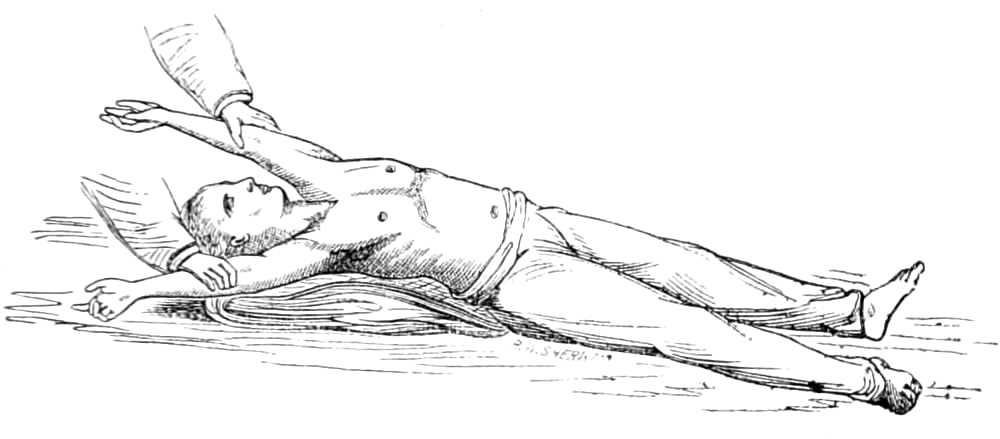
Fig. 119.—Artificial Respiration. Silvester’s Method. Expanding the Chest.

Fig. 120.—Artificial Respiration. Silvester’s method. Compressing the Chest.
Silvester’s Method.—Lay the patient on a flat surface, the head and shoulders supported on his coat folded into a firm cushion. Loosen all tight clothing, and if wet replace it by a warm dry blanket, his arms being outside the blanket. Clear the mouth of dirt, blood, &c., draw the tongue forwards, and fasten it to the chin by a piece of string or tape tied round it and the lower jaw. Next, standing at the patient’s head, grasp the arms at the elbows, and draw them gently and steadily upwards till the hands meet above the head (see fig. 119);[Pg 185] keep them so stretched for two seconds. Then slowly replace the elbows by the sides, and press gently inwards for two seconds (see fig. 120). These movements are repeated without hurry about fifteen times in a minute, until a spontaneous effort to breathe is made, when exertion should be directed to restoring the circulation by rubbing the limbs upwards towards the body, and by placing hot bottles at the pit of the[Pg 186] stomach, to the armpits, between the thighs, and to the feet. Should natural breathing not commence, artificial respiration should be continued for two hours before success is despaired of.
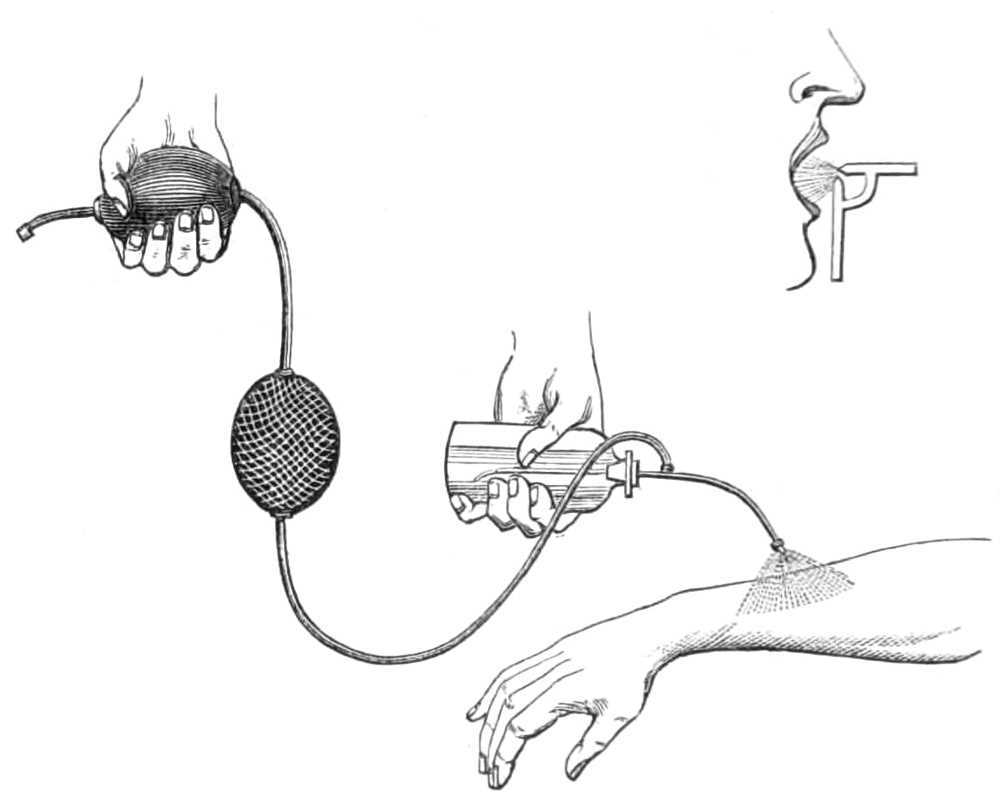
Fig. 121.—The Spray-producer.
Richardson’s Ether Spray-Producer (fig. 121) consists of a tube on which two india-rubber bags are placed; one, protected by a silk net, acts as a reservoir; the other, furnished with a valve, is the pump; these drive a constant stream of air over the tip of a fine tube projecting from a flask of ether; this sucks up the ether and throws it in fine spray on the surface to be chilled by its evaporation. The ether for this purpose must be very pure and dry, having a specific gravity of ·720, or the evaporation will not be sufficiently[Pg 187] rapid to produce congelation. The first effect of the spray is a numbing aching pain with reddening of the surface. This is succeeded by a pricking pain. In ten seconds, if the ether be good, a dead white hue spreads rapidly over the skin, and when this appears the surface is quite insensible.
The bottle and elastic air-pump may be attached to the glass jet seen in the corner of fig. 121, which then makes an apparatus for injecting astringent solutions in spray over the nasal passages, the throat, and air-tubes; but the tubes used for watery fluids are much wider than that for pulverising ether into spray. Tannin in solution of 3-10 grains to the ounce of water, sulphate of zinc, or alum in similar quantity, may be thus inhaled with much benefit by persons suffering from chronic congestion of the mucous membranes.
Injecting Chloroform Vapour into the Uterus is a ready means of relieving pain in cancer of that organ; special apparatus is made for the purpose, but an ordinary elastic clyster syringe will answer the purpose, if the flask is unscrewed and a few drops of chloroform are poured into it, from time to time, while air is pumped through the delivery tube, which is passed up the vagina to the ulcerated cervix-uteri.
Subcutaneous Injection.—The syringe for this operation (fig. 122) consists of a graduated glass tube holding six minims. The piston works in a silver continuation of the graduated tube, and is thus kept clear of the solutions used for injection. To the nozzle of the syringe fine sharp-pointed cannulæ are screwed on; they are of different lengths, some of[Pg 188] steel, others of steel gilt; the gilding renders the points very blunt, and consequently much more painful to insert. In filling the syringe, care should be taken not to draw the fluid above the level of the graduation on the tube, that the exact amount injected may be read off as the liquid sinks in the tube. The finer the cannula, and the sharper its point, the less pain is caused by its introduction.
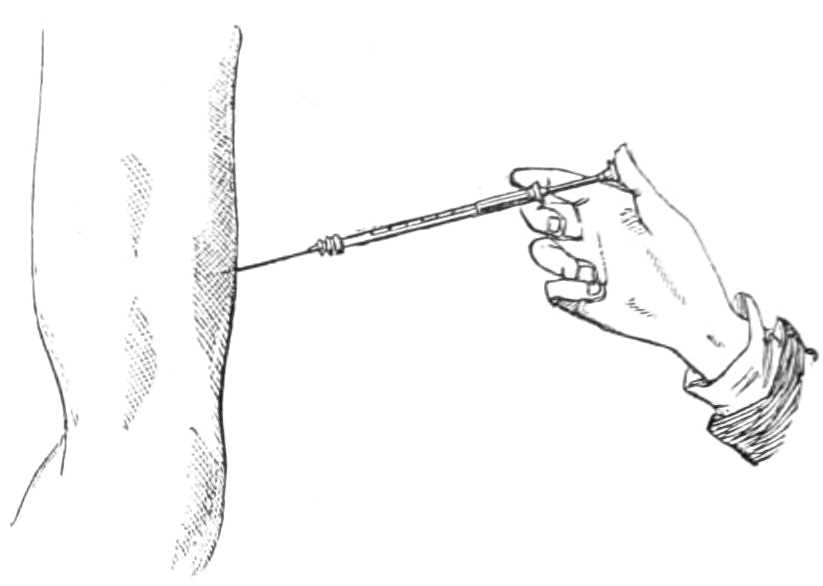
Fig. 122.—Subcutaneous Injection.
The solution of morphia should contain a grain in six drops and be as little acid as possible. In injecting morphia, it should be recollected that ⅙ grain is the usual dose to allay pain, and produce sleep; doses even far smaller often suffice for this purpose, though very much greater quantities can be administered by injection, where long use has rendered the patient tolerant of the drug. Some persons dread the puncture considerably; for them the pain may be entirely prevented by numbing the surface with ether-spray (see page 186) before inserting the syringe, though[Pg 189] usually the prick is of so little consequence that any precaution of this kind is unnecessary.
The cannula should be thrust completely through the skin into the subcutaneous cellular tissue; if the fluid is injected into the skin itself, inflammation and suppuration of the puncture sometimes ensues. After the cannula is withdrawn, the finger should be placed for a few seconds over the puncture, or much of the fluid will leak out again. When large quantities of solution (one or two syringefuls) are injected the cannula need not always be withdrawn, the nozzle can be unscrewed and the syringe charged again; but more than ten or twelve drops injected into one place generally causes much pain, even where the cellular tissue is very loose.
The syringe and cannula should be carefully cleaned, by sending plenty of cold water through them each time they are used, or the cannula will rust and become unfit for use.
Collodion is much used in drawing the edges of small wounds together, &c. Preston’s plastic collodion, or the flexible collodion of the British Pharmacopœia, 1867, have advantages over the common form by furnishing a tougher pellicle, yielding to the movements of the skin beneath without cracking. Collodion should be kept for use in a small wide-mouthed bottle, with stopper and brush, and when employed should be laid on quickly in a thick mass, so that the crust it leaves shall be of one layer. A tougher crust is obtained if a piece of muslin is soaked in the collodion and then laid on the wound, than if the collodion is used alone.
[Pg 190]
Vaccination.—The lymph of the vaccine vesicle, taken between the seventh and tenth days, is preserved for use on lancet-shaped slips of bone 1 inch long, called points. These are dipped in the lymph as it exudes from the vesicle, and exposed to the air till dry; they are then wrapped in paper ready for use. When used, the lymph should be moistened, by holding them over a vessel of steaming water a few seconds before inserting them in the wound made to receive the lymph.
The points often lose the virus in a few days, and should, if possible, be used the same day they are charged.
The lymph may be much longer preserved if hermetically sealed in glass tubes. These are about the thickness of a darning-needle, 3 inches long, and open at both ends. When the tube is to be charged, one end is inserted in the lymph exuding from a punctured vesicle; a drop then enters the tube by capillary attraction, but filling not more than half its interior: a few shakes of the hand will send the drop a little further in. The lymph end of the tube is then taken in the thumb and forefinger, while the unoccupied part of the tube is passed once or twice quickly through the flame of a candle. This rarifies the air, and while it is warm the end is closed by melting it at the edge of the flame. The second end is then closed in the same way as the first. When the lymph is wanted for use, the ends of the tube are broken, and the lymph blown out on the point of a lancet. Lymph preserved in these tubes retains its efficacy an indefinite time. The National Vaccine Institution,[Pg 191] Russell Place, Fitzroy Square, London, W., supplies to medical practitioners both points and tubes gratis on application.
In performing the operation the common lancet does very well; but two or three forms of narrow-grooved lancets are employed by surgeons for this purpose. The operation is most successful when the lymph is transferred direct from arm to arm; the lancet making the puncture is then charged at the vesicle of a child vaccinated a week before, and points are unnecessary. When making the puncture the surgeon grasps the child’s arm in his left hand, puts the skin on the stretch over the insertion of the deltoid with his left forefinger and thumb, pushes the lancet downwards between the cutis and cuticle, about 1-10th of an inch, to raise the latter in a little pocket; he then charges his lancet with lymph and inserts it in the pocket, or if using points, inserts the moistened point for a minute, taking care as he withdraws the point to press the skin down on the point with his left thumb, that the lymph may be well wiped off the point and left in the wound. This process is repeated four or five times and the operation is complete. The corium should not be penetrated, or it will bleed freely and the blood will wash away the lymph; one drop of blood is of little consequence; indeed, it shows that an absorbing surface has been reached.
The phenomena following the insertion of the vaccine virus in an infant’s arm are as follows:—On the second day the puncture is slightly elevated; on the third it begins to grow red; on the fifth it is marked by a distinct vesicle with a depressed centre and red areola;[Pg 192] on the eighth the vesicle is perfect, of pearl-like aspect, full of clear lymph; the areola, often little marked by the eighth day, rapidly increases on the ninth and tenth days, and reaches an inch or more in diameter. This bright-red inflammatory action in the skin is essential to show the system is properly infected with the vaccine disease; by the twelfth day the areola has lessened, the lymph is yellow, and often escapes by rupture of the vesicle; on the fourteenth day the vesicle has dried to a scab, that falls on the twenty-first day, leaving a dotted cicatrix, the vestige of the multilocular structure of the vesicle. The three important marks diagnostic of the vaccination being satisfactory, are—1, the pearly multilocular vesicle of the 8th-9th day; 2, the widely-spread areola on the 9th-12th day; 3, the well-marked foveated cicatrix after the scab has fallen.
Observation shows that the number of people who take small-pox after vaccination is very small indeed, when more than three well-marked scars exist; and this number at least should be secured by making five insertions of lymph at the time of vaccination.
[Pg 193]
[1] Lister’s shell-lac plaster can be obtained of the Glasgow General Apothecaries’ Company, and the sheet tin of Messrs. Compton & Co., 148, Fenchurch Street, E.C.
[Pg 195]
| The Operating Room. | Sedatives and Restoratives. |
| The Sick Bed and Bed-room. | The Arrest of Hæmorrhage. |
Having a good Light and Windows that open readily, and a Fire in Winter.
| 1. Firm table, 4 feet long, 2 feet wide, and 3½ feet high. | 14. Tow. |
| 2. Pillows. | 15. Perchloride of iron. |
| 3. Blankets. | 16. Basins, large and small. |
| 4. Towels. | 17. Hot and cold water, ice. |
| 5. Old linen. | 18. Bucket and slop-jar. |
| 6. Mackintosh sheets. | 19. Sponges. |
| 7. Old carpet, or old sheet to cover the floor. | 20. Chloroform and inhaler. |
| 8. Tray of sawdust or sand. | 21. Oil. |
| 9. Bandages. | 22. Pins. |
| 10. Strapping plaister. | 23. Scissors. |
| 11. Lint. | 24. Brandy. |
| 12. Oiled silk. | 25. Ammonia. |
| 13. Cotton wool. | 26. Fire for heating cauteries. |
[Pg 196]
| 1. Iron bedstead. | 18. Bed-urinal and bed-stool. |
| 2. Wool and hair mattress. | 19. Basins. |
| 3. Several pillows, soft and of different sizes. | 20. Cold water. |
| 4. Air and water cushions. | 21. Condy’s fluid. |
| 5. Blankets, small single ones. | 22. Sir W. Burnett’s fluid. |
| 6. Pieces of soft flannel. | 23. A bed-rest chair. |
| 7. Six sets of sheets and pillowcases. | 24. Night lights. |
| 8. Old soft linen. | 25. A fire, or in summer a lamp to burn in the fireplace, to create a draught of air. |
| 9. Cotton-wool. | 26. Enamelled saucepan. |
| 10. Towels. | 27. Two feeding cups. |
| 11. Soft pocket-handkerchiefs. | 28. Spittoon. |
| 12. Three pieces of Mackintosh, 2 feet 6 inches square. | 29. Tea-equipage. |
| 13. Bed cradle. | 30. Tea-kettle. |
| 14. Light bedgowns. | 31. Medicine measure. |
| 15. Flannel jacket, and flannel Zouave drawers. | 32. Apparatus for keeping food warm, with lamp. |
| 16. Hot-water bottle. | 33. Flowers. |
| 17. Bed-pan. |
Before a room is occupied by a patient who has been operated on, it should be thoroughly cleaned; the walls and ceiling should be well brushed, the carpet taken away and the floor thoroughly scrubbed with soda. All curtains and chintz furniture should be removed, old window-blinds replaced by new green ones, and the window made to open readily at the top and bottom. A fire or oil-lamp should be lighted in the fireplace to maintain a circulation of air. If the season require a fire, the iron fender should be removed and replaced by a wooden tray of sand or ashes, to prevent the noise of cinders and fire-irons falling on the fender and hearth. It is well also to flush all the drains, water-closets and sinks in the house with disinfecting fluid one or two days before the operation, and a store of Sir William Burnett’s, or similar disinfecting fluid, should be made ready to clear away the fœtid odours of discharges as they arise.
When possible, it is a great advantage to have two beds of similar height and size, that the patient may occupy them alternately. The cool bed refreshes the patient greatly, and the vacated bed is easily cleaned and aired without fatigue to the sick person.
[Pg 197]
| 1. Tincture of opium. | 3. Morphia suppository. |
| 2. Solution of morphia and hypodermic syringe. | 4. Ice. |
| 1. Brandy, champagne, sherry. | 10. Milk. |
| 2. Eau-de-cologne. | 11. Lime-water. |
| 3. Liquor ammoniæ. | 12. Soda-water. |
| 4. Smelling salts. | 13. Eggs. |
| 5. Spirit of chloroform. | 14. French bread. |
| 6. A fan. | 15. Biscuits. |
| 7. A Rimmel’s perfume vaporiser. | 16. Arrow-root. |
| 8. Beef-tea. | 17. Liebig’s extract of meat. |
| 9. Chicken-broth. |
| 1. Artery forceps. | 11. Richardson’s styptic colloid. |
| 2. Torsion forceps. | 12. Ice, ice-cold water. |
| 3. Tourniquet. | 13. Cautery irons. |
| 4. Tenaculum. | 14. Galvanic cautery wire. |
| 5. Hare-lip pins. | 15. Ligatures, silk, fine hemp, and whipcord. |
| 6. Acupressure needles. | 16. Lint. |
| 7. Nævus needle. | 17. Amadou. |
| 8. Wire nippers. | 18. Bandages. |
| 9. Solution of perchloride of iron (equal parts of the salt and water). | 19. Compressed sponge. |
| 10. Solid perchloride of iron. | 20. Scissors. |
(See List for the Ligature of Arteries.)
[Pg 198]
| Trephining the Skull. | Cleft Palate. |
| Operations on the Eye. | Excision of Tonsils. |
| Hare-Lip. | Laryngotomy. |
| Resection of the Jaw. | Tracheotomy. |
| Excision of the whole Tongue. |
| 1. Scalpel. | 8. Quill, cut like a tooth-pick, to clear the groove of bone-dust. |
| 2. Trephines—several crowns. | 9. Lenticular knife. |
| 3. Hey’s saw. | 10. Small polypus forceps. |
| 4. Elevator. | 11. Sponges. |
| 5. Stout dissecting forceps. | 12. Lint. |
| 6. Brush to clean away the bone-dust. | 13. Ice. |
| 7. Probe. |
| 1. Chloroform, if used. | 5. Strabismus scissors and hooks. |
| 2. Laurence’s, or other head-fixer. | 6. Fine curved needles, and finest thread. |
| 3. Specula of different sizes. | 7. Lint. |
| 4. Toothed forceps. | 8. Ice, or cold water. |
| 1. Chloroform. | 9. Ice-cold water. |
| 2. Head-fixer. | 10. Perchloride of iron. |
| 3. Speculum. | 11. Fine curved needles, and finest silk thread. |
| 4. Toothed forceps. | 12. Lint. |
| 5. Curved scissors. | 13. Pulled lint. |
| 6. Strabismus hook. | 14. Basin. |
| 7. Small and large sponges. | 15. Bandage. |
| 8. Dissecting forceps. |
[Pg 199]
| 1. Atropine drops. | 6. Toothed forceps, to fix eyeball. |
| 2. Chloroform. | 7. Lint. |
| 3. Head-fixer. | 8. Cold water. |
| 4. Speculum. | 9. Gelatine plaster. |
| 5. Lacerating needles. |
| 1. Atropine drops. | 8. Scoop. |
| 2. Chloroform. | 9. Platinum spatula, to adjust edges of wound. |
| 3. Head-fixer. | 10. Small sponges. |
| 4. Speculum. | 11. Basin and water. |
| 5. Lacerating needles. | 12. Gelatine plaster. |
| 6. Toothed forceps. | 13. Wool and bandage. |
| 7. Cataract knives. | 14. Lint. |
| 1. Chloroform, if used. | 9. Light curved scissors. |
| 2. Head-fixer. | 10. Lint. |
| 3. Specula. | 11. Gelatine plaster. |
| 4. Toothed forceps. | 12. Wool and bandage. |
| 5. Right-angled knives. | 13. Atropine drops. |
| 6. Iris forceps. | 14. Small sponges and basin. |
| 7. Iris hooks. | 15. Hot and cold water. |
| 8. Capsule scissors, if required. |
| 1. Scalpel. | 10. Cheek compressor. |
| 2. Artery forceps, or sharp hook. | 11. Sponges. |
| 3. Hare-lip pins. | 12. Large towel to wrap the child in. |
| 4. Wire nippers. | 13. Chloroform and inhaler. |
| 5. Dentist’s silk twist. | When the bone has also to be bent back— |
| 6. Strapping plaster. | 14. Bone nippers. |
| 7. Silver suture. | 15. Sequestrum forceps. |
| 8. Collodion. | 16. A knitting needle; and |
| 9. Scissors. | 17. Spirit lamp to check deep hæmorrhage by the actual cautery. |
[Pg 200]
| 1. Scalpels. | 16. Wire nippers. |
| 2. Artery forceps. | 17. Actual cautery. |
| 3. Torsion forceps. | 18. Perchloride of iron. |
| 4. Ligatures. | 19. Ice. |
| 5. Retractors. | 20. Sutures, silk and wire. |
| 6. Tooth forceps. | 21. Solution of chloride of zinc. |
| 7. Narrow saw. | 22. Lint. |
| 8. Hey’s saw. | 23. Bandages. |
| 9. Bone-cutting forceps. | 24. Plaster. |
| 10. Lion’s-tooth forceps. | 25. Collodion. |
| 11. Sequestrum forceps. | 26. Mackintosh sheet. |
| 12. Gouges. | 27. Small sponges tied on sticks. |
| 13. Chisel. | 28. Larger sponges. |
| 14. Gag. | 29. Chloroform and inhaler. |
| 15. Hare-lip pins. |
| 1. Scalpel. | 17. Needle for passing the chain. |
| 2. Torsion forceps. | 18. Sharp and blunt hooks. |
| 3. Artery forceps. | 19. Stout silk. |
| 4. Gag. | 20. Metallic sutures. |
| 5. Archimedian bone-drill. | 21. Ligatures. |
| 6. Cheek retractors. | 22. Ice. |
| 7. Incisor tooth forceps. | 23. Perchloride of iron. |
| 8. Narrow saw. | 24. Cautery iron. |
| 9. Nævus needle, and | 25. Solution of chloride of zinc. |
| 10. Half a yard of thick whipcord. | 26. Collodion. |
| 11. Stout copper wire. | 27. Small sponges mounted on sticks. |
| 12. Key for twisting the wire tight. | 28. Brandy. |
| 13. Wire cutters. | 29. Chloroform and inhaler. |
| 14. Stout acupressure needle. | 30. Lint. |
| 15. Hare-lip pins. | 31. Mackintosh sheet. |
| 16. Two ecraseurs. |
[Pg 201]
| 1. Long-handled, narrow-bladed knife, for dividing the palatine muscles. | 8. Scissors. |
| 2. Long-handled curved scissors. | 9. Ice, ice-cold water. |
| 3. Slender hooked forceps, to seize soft palate. | 10. Mackintosh sheet. |
| 4. Long-handled small bistoury, for paring edges of fissure. | 11. Sponges set on sticks. |
| 5. Long-handled needles, with the eye at the point for passing sutures. | 12. Glass syringe for washing the mouth. |
| 6. Fine blue silk, or catgut. | 13. Smith’s gag. |
| 7. Blunt and sharp hooks. | 14. Chloroform and inhaler. |
| 1. Long vulsellum. | 3. Ice, ice-cold water. |
| 2. Tonsil guillotines; or, probe-pointed bistoury, the posterior two-thirds of the blade covered with lint or plaster; or, tonsil excisors of various kinds. |
| 1. A small lump of ice held in a long vulsellum against the tonsil. | 3. Long straight polypus or gullet forceps with padded ends, to compress the tonsil; one blade being passed within the mouth, the other outside against the neck. |
| 2. Small sponge on the end of a stick, dipped in ice-cold solution of perchloride of iron, or other styptic. |
| 1. Scalpel. | 5. Tapes. |
| 2. Artery forceps and ligature silk. | 6. Sharp and blunt hooks. |
| 3. Torsion forceps. | 7. Two hooked forceps. |
| 4. Silver tube, curved on the flat. | 8. Sponges. |
[Pg 202]
| 1. Scalpel. | 9. Trachea-dilator, to assist introduction of tube. |
| 2. Dissecting forceps. | 10. Sponges. |
| 3. Blunt hooks for veins. | 11. Brandy. |
| 4. Sharp hook to draw forward trachea. | 12. Ammonia. |
| 5. Double silver tube and tapes. | 13. If a foreign body is lodged in the larynx, forceps of various kinds to extract with. |
| 6. Torsion forceps. | 14. Strapping plaister. |
| 7. Artery forceps. | 15. Silver suture. |
| 8. Ligatures. |
[Pg 203]
| Removal of the Breast or Tumours. | Extirpation of the Cervix Uteri. |
| Nævus. | Amputation of the Penis. |
| Tapping the Pleura. | Circumcision. |
| Tapping the Belly. | Excision of Testis. |
| Colotomy. | Tapping a Hydrocele. |
| Ovariotomy. | Vesico-Vaginal Fistula. |
| Cæsarian Section. | Retention of Urine. |
| Strangulated Hernia. | External Urethrotomy. |
| Radical Cure of Hernia. | Lithotomy. |
| Hæmorrhoids. | Lithotrity. |
| Fistula in Ano. | Removing Foreign Bodies from the Urethra and Bladder. |
| Cleft Perinæum. |
| 1. Scalpel. | 10. Wire or silk sutures. |
| 2. Artery forceps. | 11. Lint. |
| 3. Torsion forceps. | 12. Diachylon plaster. |
| 4. Dissecting forceps. | 13. Sponges. |
| 5. Double hook. | 14. Scissors. |
| 6. Blunt hooks. | 15. Three-inch wide rollers. |
| 7. Tenaculum. | 16. Folded towel compress. |
| 8. Fine ligatures. | 17. Chloroform and inhaler. |
| 9. Half-yard of stout whipcord, for irremovable glands. | 18. Waterproof sheet. |
| 1. Nævus needles, straight and curved. | 5. Lint. |
| 2. Suture silk, stout compressed whipcord. | 6. Chloroform and inhaler. |
| 3. Scalpel. | 7. Sponge and water. |
| 4. Scissors. |
[Pg 204]
| 1. Acupressure needles. | 3. Galvanic cautery. |
| 2. Spirit lamp. | 4. Gas cautery. |
| 1. Scalpel. | 6. Ligature. |
| 2. Dissecting forceps. | 7. Lint. |
| 3. Blunt hooks. | 8. Bandage. |
| 4. Artery forceps. | 9. Sponge. |
| 5. Sharp hooks. | 10. Sutures. |
| 1. Subcutaneous injecting syringe. | 2. Solution of perchloride of iron. |
| 1. Small fine suture needles. | 2. Fine silk suture. |
| 1. Small scalpel. | 5. Collodion. |
| 2. Trocar, fitted with india-rubber tube. | 6. Strapping. |
| 3. Bucket. | 7. Scissors. |
| 4. Lint. | 8. Brandy. |
| 1. Body bandage (see p. 10). | 6. Scissors. |
| 2. Scalpel. | 7. Lint. |
| 3. Trocar. | 8. Bucket. |
| 4. Suture. | 9. Diachylon plaster. |
| 5. Collodion. | 10. Brandy. |
[Pg 205]
| 1. Scalpel. | 9. Retractors. |
| 2. Probe-pointed bistoury. | 10. Sponges. |
| 3. Director. | 11. Large trocar. |
| 4. Dissecting forceps. | 12. Tow. |
| 5. Nævus needle, threaded with thick whipcord. | 13. Sponges. |
| 6. Silver sutures. | 14. Large syringe full of warm water. |
| 7. Artery forceps. | 15. Chloroform and inhaler. |
| 8. Fine ligatures. |
| 1. Room raised to temperature of 70° F. | 13. Wire nippers. |
| 2. Scalpel. | 14. Strong whipcord. |
| 3. Clamp. | 15. Silk sutures and silver wire. |
| 4. Vulcanised india-rubber tubing, to fix on cannula. | 16. Diachylon plaster. |
| 5. Torsion forceps. | 17. Catheter for emptying the bladder. |
| 6. Artery forceps and ligatures. | 18. Soft napkins. |
| 7. Fine ligatures. | 19. Bandage or laced napkin. |
| 8. Broad retractors. | 20. Chloroform and inhaler. |
| 9. Blunt hooks. | 21. Cautery iron. |
| 10. Ovariotomy trocar. | 22. Silver pins. |
| 11. Nævus needles, threaded. | 23. Sponges. |
| 12. Hare-lip pins. |
| 1. Room maintained at temperature of 70° F. | 11. Hare-lip pins, stout and long. |
| 2. Catheter to empty bladder. | 12. Suture silk. |
| 3. Large scalpel. | 13. Fine sutures. |
| 4. Straight probe-pointed bistoury. | 14. Folded linen compress. |
| 5. Director. | 15. Broad body roller. |
| 6. Large blunt hooks. | 16. Flannel. |
| 7. Large syringe and vaginal tube, for washing out uterus per vaginam. | 17. Cotton wool. |
| 8. Artery forceps. | 18. Warm flannels. |
| 9. Ligatures, fine and stout whipcord. | 19. Chloroform and inhaler. |
| 10. Torsion forceps. |
[Pg 206]
| 1. Scalpel. | 12. Ligatures. |
| 2. Straight bistoury. | 13. Sutures. |
| 3. Probe-pointed bistoury. | 14. Lint. |
| 4. Hernia knife. | 15. Diachylon plaster. |
| 5. Narrow director. | 16. Three-inch wide roller. |
| 6. Broad director. | 17. Compress. |
| 7. Dissecting forceps. | 18. Razor. |
| 8. Blunt hooks. | 19. Sponges. |
| 9. Fine hook, in case the sac is very tense. | 20. Half grain of morphia suppository. |
| 10. Artery forceps. | 21. Chloroform and inhaler. |
| 11. Torsion forceps. | 22. Scissors. |
| 1. Razor, or scalpel, for shaving the groin. | 7. Lint. |
| 2. Tenotomy knife. | 8. Bandage. |
| 3. Needle. | 9. Scissors. |
| 4. Compressed whipcord, well waxed and soaped. | 10. Suture. |
| 5. Glass or box-wood compress. | 11. Collodion. |
| 6. Two pads of lint. |
| 1. Vulsellum, or hook, or ringed forceps. | 4. Lint and T-bandage. |
| 2. Knife-edged scissors curved on the flat. | 5. Smith’s clamp. |
| 3. Torsion forceps. | 6. Cautery iron. |
| 1. Enema of warm water. | 6. Smith’s clamp. |
| 2. Hook, vulsellum, or ring-forceps. | 7. Ice. |
| 3. Thin compressed whipcord. | 8. Solid perchloride of iron. |
| 4. Nævus needles threaded, to transfix the base of the pile. | 9. Lint and cotton wool. |
| 5. Scissors. | 10. Opium suppository. |
[Pg 207]
The same.
| 1. Probes of various sizes, some grooved. | 9. Stout ligature. |
| 2. Grooved director. | 10. Cautery iron. |
| 3. Probe-pointed curved bistoury. | 11. Lint, cotton wool. |
| 4. Straight sharp-pointed bistoury. | 12. Sponges. |
| 5. Tenaculum. | 13. Compress. |
| 6. Threaded curved needle set in a handle. | 14. Three-inch wide roller. |
| 7. Torsion forceps. | 15. Oil. |
| 8. Artery forceps. | 16. Chloroform and inhaler. |
| 1. Scalpel. | 7. Glass rods, or No. 12 bougies. |
| 2. Hook forceps. | 8. Collodion. |
| 3. Curved nævus needles, threaded. | 9. Lint. |
| 4. Stout whipcord. | 10. Sponges on handles. |
| 5. Suture silk. | 11. Oil. |
| 6. Wire suture. | 12. Chloroform and inhaler. |
| 1. Two hooked forceps, or long vulsella. | 13. Hare-lip pins. |
| 2. Specula (bivalve and duckbill). | 14. Dentists’ silk. |
| 3. Ecraseur. | 15. Cautery irons. |
| 4. Two wool holders. | 16. Perchloride of iron. |
| 5. Small sponges on sticks. | 17. Solution of chloride of zinc. |
| 6. Scalpel. | 18. Ice. |
| 7. Straight probe-pointed bistoury. | 19. Lint (if plugging necessary, see pp. 127, 128). |
| 8. Bistoury curved on the flat. | 20. Compressed sponge in pieces. |
| 9. Long-handled straight scissors. | 21. Soft silk handkerchief. |
| 10. Long-handled curved scissors. | 22. Cotton wool. |
| 11. Artery forceps. | 23. Suppository. |
| 12. Ligatures. |
[Pg 208]
| 1. Tape to tie round the root of penis. | 8. Fine ligatures. |
| 2. Straight bistoury. | 9. Fine suture, to fix the flap of mucous membrane of the urethra. |
| 3. Scalpel. | 10. Flexible catheter. |
| 4. Artery forceps. | 11. Lint. |
| 5. Torsion forceps. | 12. Tape. |
| 6. Dissecting forceps. | 13. Ice. |
| 7. Scissors. | 14. Chloroform and inhaler. |
| 1. Small straight bistoury. | 7. Torsion forceps. |
| 2. Polypus forceps. | 8. Scissors. |
| 3. Half-inch wide tape. | 9. Lint. |
| 4. Artery forceps. | 10. Ice. |
| 5. Fine ligatures. | 11. Chloroform and inhaler. |
| 6. Silk suture. |
| 1. Scalpel. | 6. Artery forceps. |
| 2. Large sharp hook. | 7. Sutures, silk or wire. |
| 3. Blunt hooks. | 8. Scissors. |
| 4. Stout whipcord. | 9. Chloroform and inhaler. |
| 5. Fine ligature. | 10. Lint. |
| 1. Trocar. | 5. Lint. |
| 2. Vulcanite syringe, with nozzle to fit cannula. | 6. Collodion. |
| 3. Tincture of iodine. | 7. Plaister. |
| 4. Suspender for the testicles. |
[Pg 209]
| 1. Duckbill speculum. | 14. Lead clamp. |
| 2. Scalpels set in long handles, curved blades. | 15. Awl for perforating the clamp. |
| 3. Long-handled curved scissors. | 16. Clamp adjuster. |
| 4. Long-handled forceps. | 17. Split shot. |
| 5. Long-handled hooked forceps. | 18. Forceps for placing and pinching the shot. |
| 6. Long-handled sharp hook. | 19. Small sponges set on slips of wood. |
| 7. Narrow curved spatula. | 20. Large sponges. |
| 8. Needles to carry silver wire suture. | 21. Sims’ catheter. |
| 9. Silver wire. | 22. Ice-cold water. |
| 10. Probes. | 23. Syringe and flexible catheter for injecting the bladder, to test the perfect closure of the fissure. |
| 11. Short curved needles, to carry fine silk suture. | 24. Chloroform and inhaler. |
| 12. Needle holder. | 25. Oil. |
| 13. Suture tightener. |
| 1. Flexible catheters (Nos. 8 to ½) (English and French). | 8. Tapes and string. |
| 2. Finest gum bougies (No. ¼). | 9. Strapping plaister. |
| 3. Silver catheters. | 10. Scissors. |
| 4. Long prostatic catheter. | 11. Trocar for tapping per rectum. |
| 5. Oil. | 12. Tincture of opium. |
| 6. Glass syringe. | 13. Morphia suppository. |
| 7. Injecting bottle. | 14. Chloroform and inhaler. |
| 1. Scalpels. | 10. Tapes. |
| 2. Catheters, silver. | 11. Sponges. |
| 3. Catheters, flexible. | 12. Tenaculum. |
| 4. Four feet of india-rubber tubing to fit catheter. | 13. Artery forceps. |
| 5. Probes, straight and grooved, with flat handles. | 14. Ligatures. |
| 6. Syme’s shouldered narrow grooved staff. | 15. Oil. |
| 7. Marshall’s long jointed grooved sound, with flexible catheter sliding on it. | 16. Ice. |
| 8. Curved director. | 17. Chloroform and inhaler. |
| 9. Lithotomy tapes or anklets. |
[Pg 210]
| 1. Firm table, of convenient height. | 15. Syringe, various nozzles. |
| 2. Folded blankets. | 16. Gorget. |
| 3. Mackintosh sheet. | 17. Tubes, with and without petticoats. |
| 4. Tray of sand, or saw-dust. | 18. Lithotrite. |
| 5. Pair of lithotomy tapes, or anklets. | 19. Catheter to fit syringe. |
| 6. Lint. | 20. Artery forceps. |
| 7. Sound. | 21. Tenaculum. |
| 8. Staff. | 22. Ligatures. |
| 9. Catheter to fit syringe, for injecting the bladder. | 23. Half grain morphia suppository. |
| 10. Lithotomy scalpels. | 24. Chloroform and inhaler. |
| 11. Forceps. | 25. Oil. |
| 12. Scoops. | 26. Sponges. |
| 13. Searcher. | 27. Bandages and tape. |
| 14. Bistouri caché. | 28. Brandy, ammonia. |
| 1. Lithotrites, fenestrated and flat. | 6. Urethral forceps. |
| 2. Hollow sound, with short beak. | 7. Injecting bottle, with nozzle to fit the hollow sound. |
| 3. Clover’s apparatus for washing out the bladder. | 8. Half grain morphia suppository. |
| 4. Oil. | 9. Hot linseed poultice. |
| 5. Lithotrite catheters. | 10. Firm bolster or pillow. |
| 1. Catheters, silver, gum, elastic. | 15. Three-branched forceps. |
| 2. Sounds of different curves. | 16. Endoscope. |
| 3. Bougies olivaires. | 17. Oil. |
| 4. Urethral forceps with long blades. | 18. Glass syringe. |
| 5. Fine dressing forceps. | 19. Scalpel. |
| 6. Fine polypus forceps. | 20. Dissecting forceps. |
| 7. Coxeter’s urethral forceps. | 21. Hook. |
| 8. Urethral lithotrite forceps. | 22. Artery forceps. |
| 9. Hunter’s tube forceps. | 23. Ligature. |
| 10. Loop of wire set in long handle. | 24. Sutures. |
| 11. Leroy d’Etiolles’ jointed scoop. | 25. Tapes. |
| 12. Leroy’s tube, and sliding hook. | 26. Sponges. |
| 13. Charrière’s hair-pin retractor. | 27. Chloroform and inhaler. |
| 14. Charrière’s bougie retractor. |
[Pg 211]
| Ligature of the Larger Arteries. | Amputations at the Shoulder-Joint, Joint, Arm, Forearm and Wrist; Metacarpus, Hip, Thigh and Leg; by Syme’s and Chopart’s Operations; Metatarsus. |
| Resections, of the Head of the Humerus, Elbow, Hip, and Knee. | |
| Removal of Necrosed Bone. |
| 1. Scalpel. | 11. Artery forceps. |
| 2. Grooved director. | 12. Fine ligatures. |
| 3. Dissecting forceps. | 13. Sutures. |
| 4. Broad grooved director. | 14. Scissors. |
| 5. Probe. | 15. Sponges on sticks. |
| 6. Blunt hooks. | 16. Larger sponges. |
| 7. Metallic retractors. | 17. Strapping. |
| 8. Aneurism needle. | 18. Lint. |
| 9. Ditto, helix curve. | 19. Bandage. |
| 10. Waxed compressed whipcord. | 20. Chloroform and inhaler. |
| 1. Scalpels. | 12. Sutures. |
| 2. Saw (Irish bow-saw). | 13. Key to compress the subclavian artery. |
| 3. Retractors. | 14. Cautery iron. |
| 4. Lion’s-tooth forceps. | 15. Wire nippers. |
| 5. Blunt hooks. | 16. Lint. |
| 6. Artery forceps. | 17. Bandages. |
| 7. Torsion forceps. | 18. Strapping. |
| 8. Tenacula. | 19. Oiled silk. |
| 9. Acupressure needles. | 20. Sponges. |
| 10. Linen retractors. | 21. Mackintosh sheet. |
| 11. Ligatures. | 22. Chloroform and inhaler. |
[Pg 212]
| 1. Straight bistoury. | 11. Ligatures. |
| 2. Retractors. | 12. Sutures. |
| 3. Blunt hooks. | 13. Lint. |
| 4. Bow-saw. | 14. Oiled silk. |
| 5. Probes. | 15. Bandages. |
| 6. Gouges. | 16. Strapping. |
| 7. Torsion forceps. | 17. Sponges. |
| 8. Artery forceps. | 18. Mackintosh sheet. |
| 9. Lion’s-tooth forceps. | 19. Angular splint to support the arm. |
| 10. Bone forceps. | 20. Chloroform and inhaler. |
| 1. Strong bistoury. | 11. Torsion forceps. |
| 2. Probe-pointed bistoury. | 12. Tenaculum. |
| 3. Long probes. | 13. Ligatures. |
| 4. Bow-saw. | 14. Sutures. |
| 5. Retractor. | 15. Bandages. |
| 6. Blunt hooks. | 16. Lint. |
| 7. Narrow linen retractor. | 17. Sponges. |
| 8. Gouges and chisels. | 18. Straight bracketed long splint and pads. |
| 9. Bone forceps. | 19. Chloroform and inhaler. |
| 10. Artery forceps. | 20. Mackintosh sheet. |
| 1. Straight bistoury. | 11. Ligatures. |
| 2. Scalpels. | 12. Sutures. |
| 3. Metallic retractors. | 13. Tourniquet. |
| 4. Bow-saw. | 14. Sponges. |
| 5. Gouge. | 15. Lint. |
| 6. Chisel. | 16. Bandages. |
| 7. Artery forceps. | 17. Oiled silk. |
| 8. Torsion forceps. | 18. McIntyre’s splint and pads. |
| 9. Acupressure needle. | 19. Chloroform and inhaler. |
| 10. Tenaculum. | 20. Mackintosh sheet. |
[Pg 213]
| 1. Scalpels. | 13. Artery forceps. |
| 2. Straight and curved bistouries, with sharp and probe points. | 14. Tenaculum. |
| 3. Long and short probes. | 15. Torsion forceps. |
| 4. Directors. | 16. Acupressure needles. |
| 5. Retractors. | 17. Ligatures. |
| 6. Gouges. | 18. Sutures. |
| 7. Chisels. | 19. Lint. |
| 8. Bone forceps (various). | 20. Bandages. |
| 9. Gouge forceps. | 21. Oiled silk. |
| 10. Sequestrum forceps. | 22. Mackintosh sheet. |
| 11. Lion’s-tooth forceps. | 23. Chloroform and inhaler. |
| 12. Osteotrites. |
| 1. Tourniquet. | 10. Strapping cut into strips. |
| 2. Long amputating knife. | 11. Bandages. |
| 3. Artery forceps. | 12. Lint. |
| 4. Fine ligatures, stout ligatures. | 13. Oiled silk. |
| 5. Tenaculum. | 14. Sponges. |
| 6. Acupressure needles. | 15. Cautery irons. |
| 7. Needle nippers. | 16. Ice. |
| 8. Key to compress subclavian artery. | 17. Mackintosh sheet. |
| 9. Sutures. | 18. Chloroform and inhaler. |
| 1. Tourniquet. | 13. Bandages. |
| 2. Amputating knife. | 14. Wadding. |
| 3. Saw. | 15. Straight splints. |
| 4. Artery forceps. | 16. Sponges. |
| 5. Torsion forceps. | 17. Mackintosh sheet. |
| 6. Ligatures. | 18. Chloroform and inhaler. |
| 7. Sutures. | If a circular amputation— |
| 8. Tenaculum. | |
| 9. Acupressure needles. | 19. Split linen retractor; and |
| 10. Wire nippers. | 20. Round-pointed straight-edged knife. |
| 11. Strapping. | |
| 12. Lint. |
[Pg 214]
| 1. Tourniquet. | 10. Sutures. |
| 2. Large bistoury, or small amputating knife. | 11. Lint. |
| 3. Torsion forceps, artery forceps, and ligature thread. | 12. Wool. |
| 4. Artery forceps. | 13. Splints. |
| 5. Saw. | 14. Bandages. |
| 6. Acupressure needles. | 15. Oiled silk. |
| 7. Needle nippers. | 16. Sponges. |
| 8. Tenaculum. | 17. Mackintosh sheet. |
| 9. Fine ligatures. | 18. Chloroform and inhaler. |
| 1. Narrow-bladed bistoury. | 10. Splint to support the arm and hand. |
| 2. Bone forceps. | 11. Bandage. |
| 3. Torsion forceps. | 12. Lint. |
| 4. Artery forceps. | 13. Oiled silk. |
| 5. Fine ligatures. | 14. Mackintosh sheet. |
| 6. Small suture. | 15. Sponges. |
| 7. Strapping. | 16. Tourniquet. |
| 8. Narrow bandage. | 17. Chloroform and inhaler. |
| 9. Wadding. |
| 1. Lister’s aorta compressor. | 10. Lint. |
| 2. Long hip knife. | 11. Strapping plaister. |
| 3. Artery forceps. | 12. Sponges. |
| 4. Stout and fine ligatures. | 13. Bandages. |
| 5. Torsion forceps. | 14. Ice. |
| 6. Tenaculum. | 15. A bone-holder, or lion’s-tooth forceps, if the fragment of the bone is too short to grasp in the hand. |
| 7. Acupressure needles. | 16. Chloroform and inhaler. |
| 8. Needle nippers. | 17. Mackintosh sheet. |
| 9. Silk and silver sutures. |
(See also the List for the Operating Room).
[Pg 215]
| 1. Tourniquet. | 15. Bandages. |
| 2. Amputating knife. | 16. Oiled silk. |
| 3. Scalpel. | 17. Cautery iron. |
| 4. Bone forceps. | 18. Ice. |
| 5. Saw. | 19. Sponges. |
| 6. Torsion forceps. | 20. Mackintosh sheet. |
| 7. Artery forceps. | In a circular amputation— |
| 8. Stout and fine ligatures. | |
| 9. Sutures. | 21. A round-pointed knife, and a linen retractor split into two tongues for the thigh and three for the leg, the centre one being well waxed. |
| 10. Tenaculum. | |
| 11. Strapping. | |
| 12. Hare-lip pins. | |
| 13. Wire nippers. | |
| 14. Lint. |
(Syme’s and Chopart’s Operations.)
| 1. Tourniquet. | 11. Strapping. |
| 2. Strong bistoury. | 12. Sutures. |
| 3. Strong scalpel (Syme’s). | 13. Lint. |
| 4. Saw. | 14. Bandages. |
| 5. Bone forceps. | 15. Oiled silk. |
| 6. Artery forceps. | 16. Wool. |
| 7. Torsion forceps. | 17. Sponges. |
| 8. Tenaculum. | 18. Chloroform and inhaler. |
| 9. Acupressure needles. | 19. Mackintosh sheet. |
| 10. Wire nippers. |
| 1. Tourniquet. | 10. Lion’s-tooth, or sequestrum forceps. |
| 2. Straight bistoury. | 11. Strapping. |
| 3. Tenaculum. | 12. Lint and wool. |
| 4. Torsion forceps. | 13. Bandages. |
| 5. Acupressure needles. | 14. Narrow saw. |
| 6. Needle nippers. | 15. Bone forceps. |
| 7. Artery forceps. | 16. Mackintosh sheet. |
| 8. Ligatures. | 17. Chloroform and inhaler. |
| 9. Sutures. |
[Pg 216]
[Pg 217]
THE END.
BRADBURY, EVANS, AND CO., PRINTERS, WHITEFRIARS.